Section 1115 Fourth Quarter and Annual Report
- Report also available in Portable Document Format (PDF)
NEW YORK STATE MEDICAID REDESIGN TEAM (MRT) WAIVER
Project Number #11-W-00114/2
New York State Department of Health Office of Health Insurance ProgramsOne Commerce Plaza Albany, NY 12207
December 27, 2024
Demonstration Year: 26 (4/1/2024-3/31/2025)
Federal Fiscal Quarter: 4 (7/1/2024-9/30/2024)
I. Introduction
In July 1997, New York State (NYS) received approval from the Centers for Medicare and Medicaid Services (CMS) for its Partnership Plan Medicaid Section 1115 Demonstration. In implementing the Partnership Plan Demonstration, it was the State's goal to:
- Improve access to health care for the Medicaid population.
- Improve the quality of health services delivered.
- Expand access to family planning services.
- Expand coverage to additional low-income New Yorkers with resources generated through managed care efficiencies.
The primary purpose of the Demonstration was to enroll a majority of the State's Medicaid population into managed care, and to use a managed care delivery system to deliver benefits to Medicaid recipients, create efficiencies in the Medicaid program and enable the extension of coverage to certain individuals who would otherwise be without health insurance.
The Partnership Plan Demonstration was originally authorized for a five-year period and has been extended several times. CMS had approved an extension of the 1115 waiver on September 29, 2006, for the period beginning October 1, 2006, and ending September 30, 2010. CMS subsequently approved a series of short-term extensions while negotiations continued on renewing the waiver into 2016.
There have been several amendments to the Partnership Plan Demonstration since its initial approval in 1997. CMS approved three waiver amendments on September 30, 2011, March 30, 2012, and August 31, 2012, incorporating changes resulting from the recommendations of the Governor's Medicaid Redesign Team (MRT). CMS approved the Delivery System Reform Incentive Payment (DSRIP) and Behavioral Health (BH) amendments to the Partnership Plan Demonstration on April 14, 2014, and July 29, 2015, respectively.
The NYS Federal-State Health Reform Partnership (F-SHRP) Medicaid Section 1115 Demonstration expired on March 31, 2014. Populations in the F-SHRP were transitioned into the 1115 Partnership Plan Waiver. A final draft evaluation report was submitted to CMS on February 11, 2015, and was approved by CMS on May 24, 2016.
On May 28, 2014, NYS submitted an application requesting an extension of the Partnership Plan 1115 Demonstration for five years. On May 30, 2014, CMS accepted New York's application as complete and posted the application for a 30-day public comment period. A temporary extension was granted on December 31, 2014, which extended the waiver through March 31, 2015. Subsequent temporary extensions were granted through December 7, 2016. New York's 1115 Demonstration was renewed by CMS on December 7, 2016, through March 31, 2021. At the time of renewal, the Partnership Plan was renamed New York MRT Waiver. On April 19, 2019, CMS approved New York's request to exempt Mainstream Medicaid Managed Care (MMMC) enrollees from cost sharing by waiving comparability requirements to align with the New York's social services law, except for applicable pharmacy co-payments described in the STCs. On August 2, 2019, CMS approved New York's request to create a streamlined children's model of care for children and youth under 21 years of age with BH and Home and Community Based Services (HCBS) needs, including medically fragile children, children with a
BH diagnosis, children with medical fragility and developmental disabilities, and children in foster care with developmental disabilities. On December 19, 2019, CMS approved New York's request to limit the nursing home benefit in the partially capitated Managed Long-Term Care (MLTC) plans to three months for enrollees who have been designated as "long-term nursing home stays" (LTNHS) in a skilled nursing or residential health care facility. The amendment also implements a lock-in policy that allows enrollees of partially capitated MLTC plans to transfer to another partially capitated MLTC plan without cause during the first 90 days of a 12-month period and with good cause during the remainder of the 12-month period.
New York submitted a three-year waiver extension request to CMS on March 5, 2021. CMS granted a temporary extension of the 1115 waiver through March 31, 2024. On October 5, 2021, CMS approved an amendment that transitions a set of BH HCBS into Community Oriented Recovery and Empowerment (CORE) rehabilitative services (as such term is defined in Section 1905(a)(13) of the Social Security Act) for Health and Recovery Plans (HARP) and HIV Special Needs Plans (HIV SNP) members.
On March 23, 2024, CMS approved a five-year extension of the New York MRT demonstration. As part of the extension, CMS approved the state's second component of its MLTC amendment request to allow dual eligible to stay in MMMC Plans that offer Dual Eligible Special Needs Plans (D-SNPs) once they become eligible for Medicare.
On January 9, 2024, CMS approved a three-year amendment to the 1115 demonstration through March 31, 2027. Approval of this demonstration amendment will allow the state to advance health equity, reduce health disparities, support the delivery of health-related social needs (HRSN) services, and promote workforce development. In addition, the amendment provides the state with Substance Use Disorder (SUD) demonstration authority.
New York is well positioned to lead the nation in Medicaid reform. Significant federal savings have already been realized through New York's MRT process and substantial savings will also accrue as part of the 1115 waiver.
II. Enrollment: Fourth Quarter
MRT Waiver - Enrollment as of September 2024
| Demonstration Populations (As hard coded in the CMS 64) |
Current Enrollees (to date) |
# Voluntary Disenrolled in Current Quarter |
# Involuntary Disenrolled in Current Quarter |
|---|---|---|---|
| Population 1 - TANF Child 1 - 20 years in Mandatory Counties as of 10/1/06 | 340,820 | 3,921 | 14,885 |
| Population 2 - TANF Adults 21- 64 years in Mandatory Counties as of 10/1/06 ] | 66,732 | 1,613 | 1,745 |
| Population 3 - TANF Child 1 - 20 ('new' MC Enrollment) | 3,193 | 38 | 281 |
| Population 4 - TANF Adults 21 - 64 ('new' MC Enrollment) | 32,170 | 582 | 857 |
| Population 5 - Safety Net Adults | 226,460 | 7,293 | 18,012 |
| Population 6 - Family Health Plus Adults with Children | 0 | 0 | 0 |
| Population 7 - Family Health Plus Adults without Children | 0 | 0 | 0 |
| Population 8 - Disabled Adults and Children 0 - 64 ('old' voluntary MC Enrollment) | 160,727 | 2,544 | 95 |
| Population 9 - Disabled Adults and Children 0 - 64 ('new' MC enrollment) | 54,065 | 6,763 | 376 |
| Population 10 - Aged or Disabled Elderly ('old' voluntary MC Enrollment) | 83,704 | 2,993 | 40 |
| Population 11 - Aged or Disabled Elderly ('new' MC enrollment) | 10,523 | 13,578 | 476 |
MRT Waiver - Voluntary and Involuntary Disenrollment
| Voluntary Disenrollments | |
|---|---|
| Total # Voluntary Disenrollment's in Current Demonstration Year | 39,325 or an approximate 59.38% increase from last Q |
Reasons for voluntary disenrollment: Involuntary disenrollments have decreased by 31.88%. The decrease is primarily due to the Eligibility Ended cases which represent a loss of eligibility due to such factors as a failure to recertify and not specifically due to any type of case closure.
| Involuntary Disenrollments | |
|---|---|
| Total # Involuntary Disenrollment's in Current Demonstration Year | 36,767 or an approximate 31.88% decrease from last Q |
Reasons for involuntary disenrollment: Loss of Medicaid eligibility including death, plan termination, and retro-disenrollment.
WMS continues to send select closed cases to NYSoH. Consequently, the disenrollment numbers now draw on a smaller WMS population contributing to an overall general decline in voluntary disenrollment.
Involuntary disenrollment decreased due to a significant decrease in the number of Modified Adjusted Gross Income (MAGI) case closures that were subsequently sent to NYSoH for redetermination.
MRT Waiver-Affirmative Choices
| Mainstream Medicaid Managed Care | ||||
|---|---|---|---|---|
| Region | Roster Enrollment | New Enrollment | Auto Assigned | Affirmative Choices |
| July 2024 | ||||
| New York City | 659,534 | 22,008 | 4,327 | 17,681 |
| Rest of State | 254,631 | 12,637 | 1,474 | 11,163 |
| Statewide | 914,165 | 34,645 | 5,801 | 28,844 |
| August 2024 | ||||
| New York City | 661,793 | 19,140 | 4,243 | 14,897 |
| Rest of State | 254,519 | 11,376 | 1,623 | 9,753 |
| Statewide | 916,312 | 30,516 | 5,866 | 24,650 |
| September 2024 | ||||
| New York City | 660,478 | 20,800 | 4,132 | 16,668 |
| Rest of State | 250,409 | 12,092 | 1,416 | 10,676 |
| Statewide | 910,887 | 32,892 | 5,548 | 27,344 |
| Fourth Quarter | ||||
| Region | Total Affirmative Choices | |||
| New York City | 49,246 | |||
| Rest of State | 31,592 | |||
| Statewide | 80,838 | |||
| HIV SNP Plans | ||||
|---|---|---|---|---|
| Region | Roster Enrollment | New Enrollment | Auto Assigned | Affirmative Choices |
| July 2024 | ||||
| New York City | 13,491 | 285 | 0 | 285 |
| Rest of State | 33 | 3 | 0 | 3 |
| Statewide | 13,524 | 288 | 0 | 288 |
| August 2024 | ||||
| New York City | 13,558 | 253 | 0 | 253 |
| Rest of State | 36 | 4 | 0 | 4 |
| Statewide | 13,594 | 257 | 0 | 257 |
| September 2024 | ||||
| New York City | 13,651 | 283 | 0 | 283 |
| Rest of State | 36 | 1 | 0 | 1 |
| Statewide | 13,687 | 284 | 0 | 284 |
| Fourth Quarter | ||||
| Region | Total Affirmative Choices | |||
| New York City | 821 | |||
| Rest of State | 8 | |||
| Statewide | 829 | |||
| Health and Recovery Plans Disenrollment | ||||
|---|---|---|---|---|
| FFY 24 - Q4 | ||||
| Voluntary | Involuntary | Total | ||
| July 2024 | 547 | 1,252 | 1,799 | |
| August 2024 | 539 | 1,219 | 1,758 | |
| September 2024 | 553 | 1,287 | 1,840 | |
| Total: | 1,639 | 3,758 | 5,397 | |
Reasons for disenrollment:
Voluntary HARP disenrollments have increased by 3.34%. The primary reason for the increase was "Clients enrolling in other plans".
Involuntary HARP disenrollments decreased by 15.44%. This was primarily due to a decrease in the "Eligibility Ended" cases which represent a loss of eligibility due to such factors as a failure to recertify and not specifically due to any type of case closure. Another factor was "No PCP Coverage or Eligibility Expired."
III. Outreach/Innovative Activities
Fourth Quarter Outreach Activities
A. New York Medicaid Choice (NYMC) Field Observations Federal Fiscal Quarter: 4 (7/1/2024 - 9/30/2024) Q4 FFY 2024
As of the end of the fourth federal fiscal quarter (end of September 2024), there were 2,595,456 New York City Medicaid consumers enrolled in the MMMC Program and 74,654 Medicaid consumers enrolled in a HARP. MAXIMUS, the Enrollment Broker for the New York Medicaid CHOICE program (NYMC), conducted in person outreach, education, and enrollment activities in Human Resources Administration (HRA) facilities throughout the five boroughs of New York City.
During the reporting period, MAXIMUS Field Customer Service Representatives (FCSRs) conducted personal and phone outreach in 31 HRA facilities including 6 HIV/AIDS Services Administration (HASA) sites, 9 Community Medicaid Offices (MA Only), and 16 HRA Benefits Access Centers (Public Assistance). MAXIMUS reported that 4,595 clients were educated about enrollment options and made an enrollment choice including 618 clients in person and 3,977 clients through phone outreach.
The Contract Monitoring Unit (CMU) is responsible for monitoring outreach activities conducted by FCSRs to ensure that the approved presentation script is followed and required topics are explained. Deficiencies are reported to MAXIMUS Field Operation monthly. During the reporting period, 95 Enrollment Counseling sessions were evaluated which generated three applications for a total of three enrollments.
CMU Monitoring of Field Presentation Report - 4th Quarter 2024 Enrollment Counseling - One on One General Information 95 92 Of the three enrollments completed during informational sessions, three (100%) were randomly chosen to track for timely and correct processing. CMU reported that 100% of the clients were enrolled in a health plan of their choice and appropriate notices were mailed in a timely manner.
B. Auto-Assignment (AA) Outreach Calls for Fee-For-Service (FFS) Consumers
In addition to face-to-face informational sessions, FCSRs make outreach calls to FFS community clients and FFS Nursing Home (NH) clients identified for plan auto-assignment. A total of 31,476 FFS community clients were reported on the regular auto-assignment list; 10,407 clients responded to the call that generated 4,974 enrollments. Of the total of 15 FFS NH clients reported on NH auto-assignment list, 2 (13%) client and/or authorized representatives made a plan selection.
Of the 31,476 clients on the regular AA list, CMU monitored a total of 3,418 outreach calls conducted by FCSRs in HRA facilities; 969 responded to these calls. The following captures those observations:
Phone Enrollment Applications General Information (undecided) No Response Regular FFS Nursing Home FFS Total Regular FFS Nursing Home FFS Total Regular FFS 462 0 462 507 0 507 2,449
- Phone Enrollment Applications: 462 (48%) FFS clients made a voluntary enrollment choice for themselves and their family members including 0 NH clients for a total of 716 enrollments.
- 706 (99%) enrollments were randomly chosen to track for timely and correct processing and CMU confirmed that consumers were enrolled in the plan they selected in a timely manner.
- Undecided: 507 (52%) FFS and NH clients did not make an enrollment choice for several reasons that include having to consult a family member and/or physician. No infractions were observed for these calls.
C. NYMC HelpLine Observations July - September 2024
CMU is responsible for observing calls made by Downstate residents, including residents enrolled in managed care, and is committed to observe all Customer Service Representatives (CSRs) answering New York City calls every month. NYMC reported that 47,452 calls were received by the Helpline and 46,028 or 97% were answered. Calls answered were handled in the following languages: English: 28,077 (61%); Spanish:6,903 (15%); Chinese:1,683 (3%); Russian: 846 (2%); Creole:255 (1%); and other:8,264 (18%).
MAXIMUS records 100% of the calls received by the NYMC Helpline. CMU listened to 5,747 recorded calls. The call observations were categorized in the following manner:
CMU Monitoring of Call Center Report - Fourth Quarter 2024 General Information Phone Enrollment Phone Transfer Public Calls Disenrollment Calls Exemption Removal Dual Segment Total 3,226
(56%)567
(10%)293
(5%)1,628
(28%)29
(1%)0
(0%)4
(0%)0
(0%)5,747 A total of 1,775 (31%) recorded calls observed were unsatisfactory. 783 calls had a single infraction and 992 calls had multiple infractions. A total of 4,264 infractions/issues were reported to MAXIMUS. The following summarizes those observations:
- Process: 2,694 (63%) - CSRs did not correctly document or failed to document the issues presented; did not provide correct information to the caller; or did not repeat the issue presented by the caller to ensure the information conveyed was accurately captured or correct.
- Key Messages: 261 (6%) - CSRs incorrectly explained or omitted how to navigate a managed care plan; use of emergency room; preventative care/explanation of PCP; and referrals for specialists.
- Customer Service: 1,309 (31%) - Consumers were put on hold without an explanation or were not offered additional assistance.
A total of 4,264 corrective action plans (CAP) were implemented for the reporting quarter. Corrective actions include, but are not limited to, staff training and an increase in targeted CSR monitoring to ensure compliance.
Annual Outreach Activities
A. NYMC Field Observations Federal Fiscal Year 2024 (10/1/2023-9/30/2024)
As of the end of the federal fiscal year 2024 (end of September 2024), there were 2,595,456 New York City Medicaid consumers enrolled in the MMMC Program and 74,654 Medicaid consumers enrolled in a HARP. MAXIMUS, the Enrollment Broker for the NYMC, conducted in person outreach, education, and enrollment activities in HRA facilities throughout the five boroughs of New York City.
During the reporting period, MAXIMUS FCSRs conducted personal and phone outreach in 31 HRA facilities including 6 HASA sites, 9 Community Medicaid Offices (MA Only), and 16 HRA Benefits Access Centers (Public Assistance). Maximus reported that 18,484 clients were educated about enrollment options and made an enrollment choice including 3,037 clients in person and 15,447 clients through phone outreach.
The CMU is responsible for monitoring outreach activities conducted by FCSRs to ensure that the approved presentation script is followed and required topics are explained. Deficiencies are reported to Maximus Field Operation monthly. During the reporting period, 462 enrollment counselling sessions were evaluated which generated 12 applications for a total of 14 enrollments.
CMU Monitoring of Field Presentation Report - Annual 2024 Enrollment Counseling - One on One General Information 462 450 Of the 14 enrollments completed during informational sessions, 14 (100%) were randomly chosen to track for timely and correct processing. CMU reported that 100% of the clients were enrolled in a health plan of their choice and appropriate notices were mailed in a timely manner.
B. Auto-Assignment (AA) Outreach Calls for Fee-For-Service (FFS) Consumers
In addition to face-to-face informational sessions, FCSRs make outreach calls to FFS community clients and FFS NH clients identified for plan auto-assignment. A total of 140,120 FFS community clients were reported on the regular auto-assignment list, 41,618 (30%) clients responded to the call that generated 20,082 enrollments. Of the total of 110 FFS NH clients reported on NH auto-assignment list, 6 (5%) clients and/or authorized representatives to make a plan selection.
Of the 140,120 clients on the regular AA list, CMU monitored a total of 13,239 outreach calls conducted by FCSRs in HRA facilities; 3,862 responded to these calls. The following captures those observations:
Phone Enrollment Applications General Information (undecided) No Response Regular FFS Nursing Home FFS Total Regular FFS Nursing Home FFS Total Regular FFS 2,216 0 2,216 1,646 0 1,646 9,357
- Phone Enrollment Applications: 2,216 (57%) FFS clients made a voluntary enrollment choice for themselves and their family members including 0 NH clients for a total of 3,157 enrollments.
- 3,127 (99%) enrollments were randomly chosen to track for timely and correct processing and CMU confirmed that consumers were enrolled in the plan they selected in a timely manner.
- Undecided: 1,646 (43%) FFS and NH clients did not make an enrollment choice for several reasons that include having to consult a family member and/or physician. No infractions were observed for these calls.
C. NYMC Helpline Observations October 2023 to September 2024
CMU is responsible for observing calls made by Downstate residents, including residents enrolled in managed care, and is committed to observe all CSRs answering New York City calls every month. NYMC reported that 199,636 calls were received by the Helpline and 193,775 or 97% were answered. Calls answered were handled in the following languages: English: 115,822 (60%); Spanish: 27,867 (14%); Chinese: 7,242 (4%); Russian: 4,549 (2%); Haitian/Creole: 887 (1%); and other: 37,408 (19%).
MAXIMUS recorded 100% of the calls received by the NYMC Helpline 10/1/2023 through 9/30/2024. CMU listened to 22,679 recorded calls for the same period. The call observations were categorized in the following manner:
CMU Monitoring of Call Center Report - October 2023 to September 2024 General Information Phone Enrollment Phone Transfer Public Calls Disenrollment Calls Dual Segment Exemption Removal Total 13,059
(58%)2,336
(10%)1,221
(5%)5,895
(26%)151
(1%)0
(0%)16
(0%)1
(0%)22,67
9A total of 6,760 (28%) recorded calls observed was unsatisfactory including 3,250 calls with single infraction and 3,510 calls with multiple infractions. A total of 12,941 infractions/issues were reported to MAXIMUS. The following summarizes those observations:
- Process: 8,896 (69%) - CSRs did not correctly document or failed to document the issues presented; did not provide correct information to the caller; or did not repeat the issue presented by the caller to ensure the information conveyed was accurately captured or correct.
- Key Messages: 829 (6%) - CSRs incorrectly explained or omitted how to navigate a managed care plan; use of emergency room; preventative care/explanation of PCP; and, how referrals for a specialist works.
- Customer Service: 3,216 (25%) - Consumers were put on hold without an explanation or were not offered additional assistance.
A total of 12,941 CAPs were implemented for the reporting quarter. Corrective actions include, but are not limited to, staff training and an increase in targeted CSR monitoring to ensure compliance.
IV. Operational/Policy Developments/Issues
A. Plan Expansions, Withdrawals, and New Plans
During the fourth quarter of FFY 2023-2024, there were no new plans, plan expansions, or withdrawals.
Annual:
Anthem HP, LLC applied to expand their Medicaid, Child Health Plus (CHPlus), and HARP lines of business into the following counties: Albany, Rensselaer, Saratoga, Schenectady, and Sullivan. This expansion has not received approval at the time of this report.United Healthcare of New York, Inc. applied to expand their Medicaid, CHPlus, HARP, and IB- Dual lines of business into the following counties: Steuben, Hamilton, Saratoga, and Schuyler. This expansion has not received approval at the time of this report.
Independent Health Association, Inc applied to expand their Medicaid and HARP lines of business into Niagara County. This expansion has not received approval at the time of this report.
B. Medicaid Managed Care/Family Health Plus/HIV Special Needs Plan Model Contract
During the fourth quarter of FFY 2023-2024, there were no new MMC/Family Health Plus/HIV SNP Model Contract actions.
Annual:
On March 4, 2022, NYS submitted to CMS amendment #2 to the March 1, 2019, Model Contract that includes contract provisions related to State Directed Payments. On March 31, 2022, this amendment was issued to 15 Managed Care Organizations (MCO) for signature. At the close of FFY 2022-2023, all 15 contracts were executed by NYS and submitted to CMS for final approval. At the close of the fourth quarter of FFY 2023-2024, the DOH has yet to receive approval from CMS on these contracts.On January 26, 2024, NYS submitted to CMS the March 1, 2024, Model Contract. On February 7, 2024, this Model Contract was issued to 14 MCOs for signature. At the close of the third quarter of FFY 2023-2024, all 14 contracts were executed by NYS and submitted to CMS for final approval. At the close of the fourth quarter of FFY 2023-2024, the DOH has yet to receive approval from CMS on these contracts.
C. Health Plans/Changes to Certificates of Authority
During the fourth quarter, the Certificate of Authority for Anthem HP was updated to accurately reflect the counties in NY State whereby the plan is currently certified to provide Medicare Advantage to eligible enrollees.
The Certificate of Authority for New York Quality Health Plan, Inc. was also updated during this to reflect certification for the provision of IB-Dual benefits in the following counties: Genesee, Jefferson, Livingston, Madison, Monroe, Ontario, and Wayne.
Annual:
The DOH updated the Certificate of Authority to reflect a corporate name change for HealthPlus HP, LLC. The new name for this entity is now Anthem HP, LLC effective January 1, 2024.The DOH updated the Certificate of Authority to reflect a corporate address change for Molina Healthcare of New York, Inc effective December 19, 2023.
The Certificate of Authority for Anthem HP, LLC was updated to accurately reflect the counties in NYS whereby the plan is currently certified to provide Medicare Advantage to eligible enrollees effective August 14, 2024.
The Certificate of Authority for New York Quality Health Plan, Inc. was updated to reflect certification for the provision of IB-Dual benefits in the following counties: Genesee, Jefferson, Livingston, Madison, Monroe, Ontario, and Wayne effective July 21, 2024.
D. CMS Certifications Processed
Not applicable during this time frame.
E. Surveillance Activities
Surveillance activity completed during Fourth Quarter FFY 2023-2024 (July 1 - September 30, 2024) include the following:
Three Comprehensive Operational Surveys were completed during Fourth Quarter FFY 2023- 2024. Three Statement of Deficiencies (SODs) were issued, and three Plan of Corrections (POCs) were accepted:
- MetroPlus Health Plan, Inc. (APOC 7/2/2024)
- MetroPlus Special Needs Plan, Inc. (APOC 7/2/2024)
- MVP Health Plan, Inc. (APOC 8/13/2024)
One Targeted Operational Survey was completed during Fourth Quarter FFY 2023-2024. One Plan was found in compliance:
- HealthFirst PHSP, Inc. (Results 7/16/2024)
Three Member Services Phase II Surveys were completed during Fourth Quarter FFY 2023- 2024. Three SODs were issued and three POCs were accepted:
- MetroPlus Health Plan, Inc. (APOC 7/3/2024)
- MetroPlus Special Needs Plan, Inc. (APOC 7/3/2024)
- VNS Choice (APOC 7/9/2024)
Two Provider Access and Availability Surveys were completed during Fourth Quarter FFY 2023- 2024. Two SODs were issued and two POCs were accepted:
- Anthem HP, LLC (fka HealthPlus) (APOC 9/16/2024)
- Capital District Physicians' Health Plan, Inc. (APOC 9/24/2024)
Two Provider Directory Surveys were completed during Fourth Quarter FFY 2023-2024. Two SODs were issued and two POCs were accepted:
- Anthem HP, LLC (fka HealthPlus) (APOC 9/16/2024)
- Capital District Physicians' Health Plan, Inc. (APOC 9/24/2024)
Annual:
Surveillance activity completed during FFY 2023-2024 (October 1, 2023 - September 30, 2024) include the following:Seven Targeted Operational Surveys were completed during FFY 2023-2024. Six SODs were issued and six POCs were accepted. One plan was found in compliance:
- Anthem HP, LLC (fka HealthPlus) (APOC 11/22/2023)
- Excellus Health Plan, Inc. (In Compliance) (Results 6/5/2024)
- Health Insurance Plan of Greater NY, Inc. (HIP Emblem) (APOC 1/29/2024)
- Highmark of Western and Northeastern NY, Inc. (APOC 2/20/2024)
- Independent Health Association, Inc. (APOC 12/22/2023)
- Molina Healthcare of New York, Inc. (APOC 5/3/2024)
- New York Quality HealthCare Corporation (NYQHC/Fidelis) (APOC 10/2/2023)
Seven Comprehensive Operational were completed during FFY 2023-2024. Six SODs were issued and six POCs were accepted. A Letter of Concern was issued to one plan, requiring a self-directed CAPs:
- Amida Care, Inc. (APOC 6/4/2024)
- Capital District Physicians' Health Plan, Inc. (APOC 5/9/2024)
- MetroPlus Health Plan, Inc. (APOC 7/2/2024)
- MetroPlus Special Needs Plan, Inc. (APOC 7/2/2024)
- MVP Health Plan, Inc. (APOC 8/13/2024)
- United HealthCare of New York, Inc. (APOC 6/21/2024)
- VNS Choice (Letter of Concern) (Results 1/12/2024)
15 PCP Ratio Surveys were completed during FFY 2023-2024. Letters of Concern, requiring a self-directed CAP, were issued to 11 Plans. Four Plans were exempt: (Results 4/4/2024)
- Amida Care, Inc. (Exempt)
- Anthem HP, LLC (fka HealthPlus)
- Capital District Physicians' Health Plan, Inc.
- Excellus Health Plan, Inc. (Exempt)
- Health Insurance Plan of Greater NY, Inc. (HIP Emblem)
- Healthfirst PHSP, Inc.
- Highmark of Western and Northeastern NY, Inc.
- Independent Health Association, Inc.
- MetroPlus Health Plan, Inc.
- MetroPlus Special Needs Plan, Inc. (Exempt)
- Molina Healthcare of New York, Inc.
- MVP Health Plan, Inc.
- New York Quality HealthCare Corporation (NYQHC/Fidelis)
- United HealthCare of New York, Inc.
- VNS Choice (Exempt)
14 Provider Access and Availability Surveys were completed during FFY 2023-2024. 14 SODs were issued and 14 POCs were accepted:
- Amida Care, Inc. (APOC 6/24/2024)
- Anthem HP, LLC (fka HealthPlus) (APOC 9/16/2024)
- Capital District Physicians' Health Plan, Inc. (APOC 9/24/2024)
- Excellus Health Plan, Inc. (APOC 6/24/2024)
- Health Insurance Plan of Greater NY, Inc. (HIP Emblem) (APOC 6/25/2024)
- Healthfirst PHSP, Inc. (APOC 6/18/2024)
- Highmark of Western and Northeastern NY, Inc. (APOC 6/17/2024)
- Independent Health Association, Inc. (APOC 6/17/2024)
- MetroPlus Health Plan, Inc. (APOC 6/24/2024)
- MetroPlus Special Needs Plan, Inc. (APOC 6/24/2024)
- Molina Healthcare of New York, Inc. (APOC 6/18/2024)
- New York Quality HealthCare Corporation (NYQHC/Fidelis) (APOC 6/17/2024)
- United HealthCare of New York, Inc. (APOC 6/25/2024)
- VNS Choice (APOC 6/24/2024)
14 Provider Directory Surveys were completed during FFY 2023-2024. 14 SODs were issued and 14 POCs were accepted:
- Amida Care, Inc. (APOC 6/24/2024)
- Anthem HP, LLC (fka HealthPlus) (APOC 9/16/2024)
- Capital District Physicians' Health Plan, Inc. (APOC 9/24/2024)
- Excellus Health Plan, Inc. (APOC 6/24/2024)
- Health Insurance Plan of Greater NY, Inc. (HIP Emblem) (APOC 6/25/2024)
- Healthfirst PHSP, Inc. (APOC 6/18/2024)
- Highmark of Western and Northeastern NY, Inc. (APOC 6/17/2024)
- Independent Health Association, Inc. (APOC 6/17/2024)
- MetroPlus Health Plan, Inc. (APOC 6/24/2024)
- MetroPlus Special Needs Plan, Inc. (APOC 6/24/2024)
- Molina Healthcare of New York, Inc. (APOC 6/18/2024)
- New York Quality HealthCare Corporation (NYQHC/Fidelis) (APOC 6/17/2024)
- United HealthCare of New York, Inc. (APOC 6/25/2024)
- VNS Choice (APOC 6/24/2024)
15 Member Services Phase II Surveys were completed during FFY 2023-2024. 15 SODs were issued and 15 POCs were accepted:
- Amida Care, Inc. (APOC 5/21/2024)
- Anthem HP, LLC (fka HealthPlus) (APOC 5/13/2024)
- Capital District Physicians' Health Plan, Inc. (APOC 5/2/2024)
- Excellus Health Plan, Inc. (APOC 4/29/2024)
- Health Insurance Plan of Greater NY, Inc. (HIP Emblem) (APOC 5/13/2024)
- Healthfirst PHSP, Inc. (APOC 5/2/2024)
- Highmark of Western and Northeastern NY, Inc. (APOC 4/23/2024)
- Independent Health Association, Inc. (APOC 4/25/2024)
- MetroPlus Health Plan, Inc. (APOC 7/3/2024)
- MetroPlus Special Needs Plan, Inc. (APOC 7/3/2024)
- Molina Healthcare of New York, Inc. (APOC 4/29/2024)
- MVP Health Plan, Inc. (APOC 4/30/2024)
- New York Quality HealthCare Corporation (NYQHC/Fidelis) (APOC 4/22/2024)
- United HealthCare of New York, Inc. (APOC 5/7/2024)
- VNS Choice (APOC 7/9/2024)
V. Waiver Deliverables
A. Medicaid Eligibility Quality Control (MEQC) Reviews
No activities were conducted during FY2024. Final reports were previously submitted for all reviews except the one involved in an open legal matter.
- MEQC 2008 - Applications Forwarded to LDSS Offices by Enrollment Facilitators
No activities were conducted due to a legal matter that is still open.- MEQC 2009 - Review of Medicaid Eligibility Determinations and Re-Determinations for Single and Childless Couple Individuals Determined Ineligible for Temporary Assistance
The final summary report was forwarded to the regional CMS office and CMS Central Office on July 1, 2015.- MEQC 2010 - Review of Medicaid Eligibility Determinations and Redeterminations for Persons Identified as Having a Disability
The final summary report was forwarded to the regional CMS office on January 31, 2014, and CMS Central Office on December 3, 2014.- MEQC 2011 - Review of Medicaid Self Employment Calculations
The final summary report was forwarded to the regional CMS office on June 28, 2013, and CMS Central Office on December 3, 2014.- MEQC 2012 - Review of Medicaid Income Calculations and Verifications
The final summary report was forwarded to the regional CMS office on July 25, 2013, and CMS Central Office on December 3, 2014.- MEQC 2013 - Review of Documentation Used to Assess Immigration Status and Coding
The final summary report was forwarded to the regional CMS office on August 1, 2014, and CMS Central Office on December 3, 2014.B. Benefit Changes/Other Program Changes
Transition of Behavioral Health (BH) Services into Managed Care and Development of Health and Recovery Plans (HARPs):
In October 2015 NYS began transitioning the full Medicaid BH system to managed care. The goal is to create a fully integrated BH [mental health (MH) and SUD] and physical health service system that provides comprehensive, accessible, and recovery-oriented services. There are three components of the transition: expansion of covered BH services in MMC, elimination of the exclusion for Supplemental Security Income (SSI), and implementation of HARPs. HARPs are specialized plans that include staff with enhanced BH expertise. In addition, individuals who are enrolled in a HARP can be assessed to access additional specialty services called BH HCBS. For MMC, all Medicaid-funded BH services for adults, except for services in Community Residences, are part of the benefit package.
As part of the transition, the NYS DOH began phasing in enrollment of current MMC enrollees throughout NYS into HARPs beginning with adults 21 and over in New York City in October 2015. This transition expanded to the rest of the state in July 2016. HARPs and HIV SNPs now provide all covered services available through MMC.
In FY 2018, NYS engaged in multiple activities to enhance access to BH services and improve quality of care for recipients in MMC. In June of 2018, HARP became an option on the NYSoH. This enabled 21,000 additional individuals to gain access to the enhanced benefits offered in the HARP product line. The State identified and implemented a policy to allow State Designated Entities (SDE) to assess and link HARP enrollees to BH HCBS, and allocated quality and infrastructure dollars to MCOs in efforts to expand and accelerate access to adult BH HCBS. Additionally, the State continually offers ongoing technical assistance to the BH provider community through its collaboration with the Managed Care Technical Assistance Center (MCTAC).
Effective April 1, 2023, the Medicaid pharmacy benefit was carved out of MMC to Medicaid FFS. Medicaid members enrolled in Mainstream MCOs, HARPs, and HIV SNPs now receive pharmacy benefits through the Medicaid FFS pharmacy program, NYRx. MMC Plans began sending notices to members and their providers about the pharmacy benefit transition in 2022. Transitioning the pharmacy benefit from MMC to FFS provides NYS visibility into prescription drug costs, allows benefit centralization, and provides a single drug formulary with standardized utilization management protocols, simplifying and streamlining the drug benefit for Medicaid members.
Office of Mental Health (OMH) providers received notice that the PHE would expire on May 11, 2023. The notice detailed flexibilities afforded to providers regarding minimum billing standards and documentation requirements coming to an end, unless otherwise specified by OMH through formal regulatory waivers. Areas impacted by the end of the PHE include telehealth, documentation, utilization review, billing standards, Health Insurance Portability and Accountability Act (HIPAA) enforcement, hospital conditions of participants, and program specific guidance for community-based services and residential services.
Additionally, NYS resumed annual Medicaid recertifications in April 2023, having paused since March 2020 due to the federal PHE.
Effective November 1, 2023, NYS will implement Evidence Based Practices (EBPs), pending State Plan Amendment (SPA) approval from CMS. The State will authorize a selected number of qualified Children and Family Treatment and Supports (CFTSS) providers to receive EBP training and bill for new EBP rates. NYS is committed to the promotion and support of EBPs, specific research supported psychotherapeutic interventions with demonstrated outcomes, within CFTSS.
NYS continues to monitor plan-specific data in the three key areas: inpatient denials, outpatient denials, and claims payment. These activities assist with detecting system inadequacies as they occur and allow the State to initiate steps in addressing identified issues as soon as possible.
- Inpatient Denial Report: Each month, MCOs are required to electronically submit a report to the State on all denials of inpatient BH services based on medical necessity. The report includes aggregated provider level data for service authorization requests and denials, whether the denial was pre-service, concurrent, or retrospective, and the reason for the denial.
NYS MH & SUD authorization requests and denials for Inpatient (4/1/2024-6/30/2024)1
Region Total Authorization Total Denials (Admin and Medical Necessity) Utilization Review (Medical Necessity) Denials Medical Necessity Denial Rate NYC 24,969 77 60 0.24% ROS 3,817 40 33 0.86% Total 28,786 117 93 0.32%
- Outpatient Denial Report: On a quarterly basis, MCOs are required to submit a report to the State on ambulatory service authorization requests and denials for each BH service. Submissions include counts of denials for specific service authorizations, as well as administrative denials, internal, and fair hearing appeals. In addition, HARPs are required to report authorization requests and denials of BH HCBS.
NYS MH & SUD authorization requests and denials for Outpatient (4/1/2024-6/30/2024)2
Region Total Authorization Total Denials (Admin and Medical Necessity) Utilization Review (Medical Necessity) Denials Medical Necessity Denial Rate NYC 1,722 108 83 4.82% ROS 272 10 9 3.31% Total 1,994 118 92 4.61%
- Monthly Claims Report: Monthly, MCOs are required to submit the following for all OMH and Office of Addiction Services and Supports (OASAS) licensed and certified services.
MH & SUD Claims (7/1/2024-9/30/2024)
Region Total Claims Paid Claims (Percentage of total claims reported) Denied Claims (Percentage of total claims reported) NYC 714,431 91.05% 8.95% ROS 873,898 91.76% 8.24% Total 1,588,329 91.44% 8.56%
Behavioral Health Adults CORE/HCBS Claims/Encounters 7/1/2024-9/30/2024: NYC
Behavioral Health CORE/HCBS SERV GROUP N Claims N Recip. CPST 356 68 Education Support Services 20 5 Family Support and Trainings 338 27 Intensive Supported Employment 11 4 Ongoing Supported Employment 14 2 Peer Support 3,531 607 Pre-vocational 12 2 Provider Travel Supplements 212 100 Psychosocial Rehab 6,020 558 Residential Supports Services 78 8 Transitional Employment 0 0 TOTAL 10,592 1,092 Note: Total of N Recip. is by unique recipient, therefore the TOTAL might be smaller than sum of rows.
Behavioral Health Adults CORE/HCBS Claims/Encounters 7/1/2024-9/30/2024: ROS
Behavioral Health CORE/HCBS SERV GROUP N Claims N Recip. CPST 2,056 359 Education Support Services 74 22 Family Support and Trainings 660 45 Intensive Supported Employment 39 8 Ongoing Supported Employment 4 3 Peer Support 5,413 994 Pre-vocational 7 3 Provider Travel Supplements 5,665 1,129 Psychosocial Rehab 6,608 1,137 Residential Supports Services 578 66 Transitional Employment 0 0 TOTAL 21,104 2,247 Note: Total of N Recip. is by unique recipient, therefore the TOTAL might be smaller than sum of rows.
- Inpatient Denial Report: Each month, MCOs are required to electronically submit a report to the State on all denials of inpatient behavioral health services based on medical necessity. The report includes aggregated provider level data for service authorization requests and denials, whether the denial was pre-service, concurrent, or retrospective, and the reason for the denial.
NYS Mental Health (MH) & Substance Use Disorder (SUD) authorization requests and denials for Inpatient (7/1/2023-6/30/2024)
Region Total Authorization Total Denials (Admin and Medical Necessity) Utilization Review (Medical Necessity) Denials Medical Necessity Denial Rate NYC 96,365 454 396 0.41% ROS 21,943 150 133 0.61% Totals 118,308 604 529 0.45%
- Outpatient Denial Report: On a quarterly basis, MCOs are required to submit a report to the State on ambulatory service authorization requests and denials for each behavioral health service. Submissions include counts of denials for specific service authorizations, as well as administrative denials, internal appeals, and fair hearing appeals. In addition, HARPs are required to report authorization requests and denials of BH HCBS.
NYS MH & SUD authorization requests and denials for Outpatient (7/1/2023-6/30/2024)
Region Total Authorization Total Denials (Admin and Medical Necessity) Utilization Review (Medical Necessity) Denials Medical Necessity Denial Rate NYC 11,883 455 209 1.76% ROS 1,696 89 88 5.19% Totals 13,579 544 297 2.19% *Due to data submission issue, Healthfirst Q4 utilization review Outpatient data has been excluded in this report
- Monthly Claims Report: Monthly, MCOs are required to submit the following for all OMH and OASAS licensed and certified services.
MH & SUD Claims (10/1/2023-9/30/2024)
Region Total Claims Paid Claims
(Percentage of total claims reported)Denied Claims
(Percentage of total claims reported)NYC 3,979,175 92.22% 7.78% ROS 5,266,743 94.47% 5.53% Totals 9,245,918 93.50% 6.50%
Behavioral Health Adults CORE/HCBS Claims/Encounters 10/1/2023-9/30/2024: NYC
Behavioral Health CORE/HCBS SERV GROUP N Claims N Recip CPST 1,265 148 Education Support Services 137 11 Family Support and Trainings 1,987 50 Intensive Supported Employment 78 10 Ongoing Supported Employment 49 3 Peer Support 19,236 1,177 Pre-vocational 115 7 Provider Travel Supplements 759 1,214 Psychosocial Rehab 25,393 1 Residential Supports Services 382 13 Transitional Employment 0 0 TOTAL 49,401 2,040 Note: Total of N Recip. is by unique recipient, therefore the TOTAL might be smaller than sum of rows.
Behavioral Health Adults CORE/HCBS Claims/Encounters 10/1/2023-9/30/2024: ROS
Behavioral Health CORE/HCBS SERV GROUP N Claims N Recip CPST 9,954 664 Education Support Services 450 42 Family Support and Trainings 2,152 80 Intensive Supported Employment 189 26 Ongoing Supported Employment 40 7 Peer Support 27,598 1,874 Pre-vocational 69 13 Provider Travel Supplements 29,104 2,190 Psychosocial Rehab 31,724 2,111 Residential Supports Services 2,958 124 Transitional Employment 0 0 TOTAL 104,238 3,902 Note: Total of N Recip. is by unique recipient, therefore the TOTAL might be smaller than sum of rows.
Provider Technical Assistance
MCTAC is a partnership between the McSilver Institute for Poverty Policy and Research at New York University School of Social Work and the National Center on Addiction and Substance Abuse (CASA) at Columbia University, as well as other community and State partners. It provides tools and trainings that assist providers to improve business and clinical practices as they transition to managed care. See below for MCTAC.
Fourth Quarter MCTAC Attendance & Statistics (7/1/2024 to 9/30/2024)
Events: MCTAC successfully executed 21 events from 7/1/2024 to 9/30/2024. 19 events were held via webinar and 2 were held in-person. 3 of the 19 webinars were pre-recorded.
Individual Participation/Attendance/Viewing of Resource3 (this includes all the individuals that attended the MCTAC offerings or viewed a resource online)3,671 people attended/participated in MCTAC events/viewed resources of which 1,600 were unique participants.
OMH Agency Participation/Attendance/Viewing of Resource
Overall: 49.15% (261 of 531 total employees)OASAS Agency Participation/Attendance/Viewing of Resource
Overall: 32.56% (141 of 433 total employees)
Annual MCTAC Attendance & Statistics (10/1/2023 to 9/30/2024)
Events: MCTAC successfully executed 64 events from 10/1/2023 to 9/30/2024. 57 events were held via webinar and 7 were held in-person. 10 of the 57 webinars were pre-recorded.
Individual Participation/Attendance/Viewing of Resource: (this includes all the individuals that attended the MCTAC offerings or viewed a resource online)
14,397 people attended/participated in MCTAC events/viewed resources of which 5,060 were unique participants.
OMH Agency Participation/Attendance/Viewing of Resource
Overall: 70.81% (376 of 531 total employees)OASAS Agency Participation/Attendance/Viewing of Resource
Overall: 59.12% (256 of 433 total employees)
Efforts to Improve Access to Behavioral Health Home and Community Based Services
All HARP enrollees are eligible for individualized care management. In addition, BH HCBS were made available to eligible HARP and HIV SNP enrollees. These services were designed to provide enrollees with specialized supports to remain in the community and assist with rehabilitation and recovery. Enrollees were required to undergo an assessment to determine BH HCBS eligibility. Effective January 2016 in NYC and October 2016 for the rest of the state, BH HCBS were made available to eligible individuals.
As discussed with CMS, NYS experienced slower than anticipated access to BH HCBS for HARP members and actively sought to determine the root cause for this delay. Following implementation of BH HCBS, NYS and key stakeholders identified challenges, including: difficulty with enrolling HARP members in Health Homes; locating enrollees and keeping them engaged throughout the lengthy assessment and Plan of Care development process; ensuring care managers have understanding of BH HCBS (including person-centered care planning) and capacity for care managers to effectively link members to rehab services; and difficulty launching BH HCBS due to low number of referrals to BH HCBS providers.
To address the identified challenges, NYS made efforts to ramp up utilization and improve access to BH HCBS. NYS effectuated the following:
- Streamlined the BH HCBS assessment process.
- Effective March 7, 2017, the full portion of the NYS Community Mental Health assessment is no longer required. Only the brief portion (NYS Eligibility Assessment) is required to establish BH HCBS eligibility and provide access to these services.
- Developed training for care managers and BH HCBS providers to enhance the quality and utilization of integrated, person-centered plans of care and service provision, including developing a Health Home training guide for key core competency trainings to serving the high need SMI population.
- BH HCBS Performance - fine-tuned MCO Reporting template to improve Performance Dashboard data for the BH HCBS workflow (Nov 2018, streamlining data collection for both Health Homes and Recovery Coordination Agencies (RCAs)).
- Developed required training for BH HCBS providers that NYS can track in a Learning Management System.
- Implemented rates that recognize low volume during implementation to help providers ramp up to sustainable volumes.
- Enhanced technical assistance efforts for BH HCBS providers including workforce development and training.
- Obtained approval from CMS to provide recovery coordination services (assessments and care planning) for enrollees who are not enrolled in Health Homes. These services are provided by SDEs through direct contracts with the MCO.
- Developed and implemented guidance to MCOs for contracting with SDE to provide recovery coordination of BH HCBS for those not enrolled in Health Home.
- Developed Documentation and Claiming guidance for MCOs and contracted RCAs for the provision of assessments and development of plans of care for BH HCBS.
- Additional efforts to support initial implementation of RCAs include:
- In-person trainings (completed June 2018)
- Weekly calls with MCOs (completed)
- Ongoing technical assistance (completed)
- Continued efforts to increase HARP enrollment in Health Homes including:
- Best practices for embedded care managers in ERs, Clinics, shelters, Comprehensive Psychiatric Emergency Programs and Inpatient units and engagement and retention strategies.
- Existing quality improvement initiative within clinics to encourage Health Homes enrollment.
- Emphasis on warm hand-off to Health Home from ER and inpatient settings.
- Psychiatric Services and Clinical Knowledge Enhancement System (PSYCKES) quality initiatives incentivizing MCOs to improve successful enrollment of high-need members in care management.
- DOH approval of MCO plans for incentivizing enrollment into Health Homes (e.g., outreach optimization).
- Continued work to strengthen the capacity of Health Homes to serve high need SMI individuals and ensure their engagement in needed services through expansion of Health Home Plus (HH+) effective May 2018.
- Provided technical assistance to lead Health Homes, representation on new HH+ Subcommittee Workgroup.
- Implemented Performance Management efforts, including developing enhanced oversight process for Health Homes who have not reached identified performance targets for and key quality metrics for access to BH HCBS for HARP members.
- Disseminated consumer education materials to improve understanding of the benefits of BH HCBS and educating peer advocates to perform outreach.
- NYS OMH contracted with the New York Association Psychiatric Rehabilitation Services (NYAPRS) to conduct peer-focused outreach and training to possible eligible members for HARPs and Adult BH HCBS.
- NYAPRS conducted outreach in two ways:
- 45-90-minute training presentations delivered by peers.
- Direct one-to-one outreach in community spaces (such as in homeless shelters or on the street near community centers).
- Implemented Quality and Infrastructure initiative to support targeted BH HCBS workflow processes and increase in BH HCBS utilization. In-person trainings completed June 2018. NYS worked with the MCOs on an ongoing basis to further monitor and operationalize this program and increase access and utilization of BH HCBS.
- 13 HARPs distributed over $34 million through 95 provider contracts to support the focused and streamlined administration of BH HCBS, including coordination of supports from assessment to service provision.
- Outreach to all HARPs was conducted to discuss best practices identified through the use of Quality and Infrastructure initiative funds that resulted in an increase of members utilizing BH HCBS; NYS also shared a summary of best and promising practices with the HARPs.
- Issued Terms and Conditions for BH HCBS providers to standardize compliance and quality expectations of BH HCBS provider network and help clarify for MCOs which BH HCBS providers are actively providing services.
- Enhanced NYS Adult BH HCBS Provider oversight, including development of oversight tools and clarifying service standards for BH HCBS provider site reviews, including review of charts, interviews with staff or clients and review of policy and procedures.
- Worked with the HARP/BH HCBS Subcommittee (2017-2019) - consisting of representatives from MCOs, Health Homes, Care Management Agencies (CMAs), and BH HCBS provider agencies. Developed and provided a variety of tools to support care manager referrals to BH HCBS, on behalf of the NYS Health Home/MCO Workgroup.
- Established a process for care managers and supervisors to apply for a waiver of staff qualifications for administering the NYS Eligibility Assessments. This was in response to challenges in securing a care management workforce meeting both the education and experience criteria and need for more assessors.
To date, 5,409 care managers in NYS have completed the required training for conducting the NYS Eligibility Assessment for BH HCBS. Also, between July 1, 2024, and September 30, 2024, 550 eligibility assessments were completed.
Transition to Community Oriented Recovery and Empowerment Services
Despite the extensive efforts outlined above, and stakeholder participation to implement strategies for improved utilization of BH HCBS, the number of HARP enrollees successfully engaged with BH HCBS overall remained very low. NYS reviewed a significant amount of feedback from MCOs, Health Homes, care managers and other key stakeholders, and determined the requirements for accessing BH HCBS were too difficult to standardize among 15 MCOs and 30 Health Homes.
As a result, NYS released a draft proposal for public comment in June 2020 to transition 1115 Waiver BH HCBS into a State Adult Rehabilitation Services package, called CORE Services, for HARP enrollees and HARP eligible HIV-SNP enrollees. Public comment resulted in positive feedback, and NYS finalized the proposal and submitted to CMS in September 2020. Objectives of this transition were two-fold: to simplify and allow creativity in service delivery of community- based rehabilitation services tailored to the specific needs of the BH population, and to eliminate access barriers.
To receive the enhanced Federal Medical Assistance Percentage (eFMAP) available through the American Rescue Plan Act (ARPA), NYS revised the September 2020 proposal to comply with eFMAP requirements and resubmitted to CMS in July 2021. CMS approved NYS's 1115 Waiver Amendment Request for CORE Services on October 5, 2021. CORE is a rehabilitation and recovery service array which includes four services previously available through BH HCBS: Psychosocial Rehabilitation (PSR), Community Psychiatric Support and Treatment (CPST), Family Support and Training (FST), and Empowerment Services — Peer Support.
Access to CORE Services does not require an independent eligibility assessment and these services do not have settings restrictions. Currently, all HARP enrollees, HARP-eligible HIV- SNP enrollees, and HARP-eligible MAP enrollees can access CORE Services with a recommendation from a Licensed Practitioner of the Healing Arts (LPHA).
Enrollment in Health Home Care Management continues to be an important piece of the HARP benefit package for the comprehensive, integrated coordination of the care offered by Health Homes. Care managers will always have the important role of ensuring timely access to services reflective of the member's preferences and individual needs, in continued collaboration with MCOs and service providers.
CORE Services went live on February 1, 2022, for new and existing recipients (HARP enrollees and HARP-eligible HIV-SNP enrollees). The transition period for existing recipients of BH HCBS CPST, PSR, FST and Peer Support to CORE CPST, PSR, FST and Peer Support ended April 30, 2022.
Consumer education materials are available on the OMH CORE website and were distributed via provider listserv. In January 2022, OMH participated in a Townhall series hosted by the Access 2 Recovery Coalition with a goal of educating HARP members about benefit changes. NYS conducted a series of implementation trainings in partnership with MCTAC. After a transitional period of provisional designation and attestation, 115 providers received full designation for CORE Services. NYS engaged providers in a significant amount of outreach and technical assistance to ensure the provider system was prepared for this transition, supporting and prioritizing continuity of care for members receiving these services. A list of fully designated CORE providers is available on the OMH CORE website.
In January 2023, in collaboration with Alliance for Rights and Recovery (formerly NYAPRS), a CORE Peer Navigator Project was launched. This project is funded through the Mental Health Block Grant, and focuses on outreach, education, and service navigation to support access to CORE and BH HCBS. In August 2024, the project was approved for a no cost contract extension through February 28, 2025.
As of January 1, 2023, HARP-eligible MAP enrollees can also access CORE Services with an LPHA recommendation. NYS continues to provide technical assistance on this benefit carve-in. NYS provided MAP Plans with CORE Services guidance and training, in addition to MAP benefit package trainings for CORE Service providers and care managers.
NYS continues to consult CORE providers and MCOs to inform future guidelines around MCO responsibilities and oversight, such as utilization management of CORE Services. In August 2023, NYS held its first CORE Summit, a one-day training and networking event for CORE providers and MCOs. A second CORE Summit was held in August 2024. OMH and OASAS continue to provide education via trainings, conference presentations, and regional provider forums based on stakeholder feedback. In April 2024, updates were published to the CORE Services Benefit and Billing Guidance and to the CORE Service Initiation Notification Template to bring information current and to add clarifications in response to stakeholder feedback. In September 2024, OMH and OASAS began hosting the first of 14 regional networking events for CORE providers, MCOs, care managers, and other local service providers to promote collaboration and referral connections.
Habilitation, Education Support Services, Pre-Vocational Services, Transitional Employment, Intensive Supported Employment, and Non-Medical Transportation remain in the BH HCBS benefit package. In January 2022, NYS issued revised Adult BH HCBS Workflow guidance for care managers to reflect this change, as well as training for care managers that included a full overview of the CORE Services. NYS will continue its efforts to increase access to BH rehabilitation services through working collaboratively with Health Homes.
From June 2023 to May 2024, 6,128 unique recipients received CORE Services. Specifically, the count of monthly recipients for the four transitioned services from Adult BH HCBS to CORE Services increased by 57.1%, from 1,935 (January 2022, the month before HCBS/CORE transition) to 3,039 (May 2024).
In addition, in 2021, NYS extended the Adult BH HCBS Infrastructure funding initiative to support BH providers transitioning the four services moving from BH HCBS to the new CORE Service array and continuing support of BH HCBS providers. OMH and OASAS distributed guidance for an Infrastructure Program Extension which allowed HARPs to contract for remaining, unspent funds totaling approximately $31.9 million. Based on a thorough network needs assessment, HARPs competitively awarded the funds to eligible providers. Infrastructure Program Extension contracts were executed between May and September 2022, with contracted activities currently underway. OMH and OASAS continue to work closely with the HARPs to further monitor and operationalize the program.
- 11 HARPs executed 80 provider contracts which account for 59% of all designated BH HCBS and CORE providers to support the transition to CORE Services and the continued provision of BH HCBS.
- Approximately $28.3 million in initial contract base awards and subsequent milestone payments were distributed to providers.4
- The program concluded on July 31, 2024. As of July 5, 2024, 32 out of 80 contracts have concluded. NYS is in process of obtaining final reports and metrics from HARPs.
- NYS developed an Infrastructure Program Extension dashboard which monitors BH HCBS, and CORE Service claims and unique recipients served by BH HCBS and CORE Service providers during the measurement period. The dashboard compares BH HCBS and CORE providers in Infrastructure Program Extension contracts with HARPs to those not in Infrastructure Program Extension contracts. NYS solicited and incorporated feedback from HARPs on the development of the dashboard.
- In July 2024, NYS distributed a compiled list of "best practices", informed by HARPs and providers as they jointly developed innovative solutions to engage HARP members, expedite the BH HCBS and CORE Services workflow, and address barriers to receiving BH HCBS and CORE services.
Transition of School-based Health Center (SBHC) Services from Medicaid Fee-for-Service to Medicaid Managed Care (MMC):
Activities within the DOH were initiated to plan for SBHC services to be included in the MMC benefit package effective April 1, 2025. SBHCs are a critical source of primary care, urgent medical care, and dental care for school-age children. The transition of SBHCs into the MMC benefit package is intended to strengthen and improve the coordination of care, quality of care, and outcomes for children.
Annual: No activity occurred during the reporting period for quarters one, two, and three. In quarter four, the DOH began working towards the April 1, 2025, for SBHC services to be included in the MMC benefit package.
C. Managed Long-Term Care Program (MLTCP)
MLTC plans include Partial Capitation, PACE, MAP, and FIDA-IDD plans. As of October 1, 2024, there are 15 Partial Capitation plans, 9 PACE plans, 12 MAP, and 1 FIDA IDD plan. As of October 1, 2024, there are a total of 364,784 members enrolled across all MLTC products.
1. Accomplishments/Updates
During the July 2024 through September 2024 quarter, the DOH approved the service area expansion for one MAP.
During the annual period of October 2023 through September 2024, the DOH approved six mergers between Partial Capitation plans. DOH also approved service area expansions for one MAP plan, and two Partial Capitation plans. One Partial Capitation plan and one MAP plan withdrew enrollment. One new MAP plan began operations.
New York's Enrollment Broker, NYMC, conducts the MLTC Post Enrollment Outreach Survey which contains questions specifically designed to measure the degree to which consumers may maintain their relationship with the services they were receiving prior to mandatory transitions to MLTC. For the July 2024 through September 2024 quarter, post enrollment surveys were completed for eight enrollees. Of the six surveyed, five (83%) indicated that they continued to receive services from the same caregivers once they became members of an MLTCP. The percentage of affirmative responses is higher than the previous quarter.
Enrollment: Total enrollment in MLTC partial capitation plans increased from 293,378 to 301,679 during the July 2024 through September 2024 quarter, a 3% increase from the last quarter. For this period, 16,786 individuals who were being transitioned into MLTC made an affirmative choice, a 4% decrease from the previous quarter and brings the 12-month total for affirmative choice to 65,917.Monthly plan-specific enrollment for Partial Capitation plans, PACE plans, MAP plans, and FIDA IDD plans during the October 2023 through September 2024 annual period is submitted as an attachment.
2. Significant Program Developments
During the July 2024 through September 2024 quarter:
- The Third Quarter Member Services survey was conducted on 15 Partial Capitation plans and 12 MAP plans. This survey was intended to provide feedback on the overall functioning of the plans' member service performance. No response was required, but, when necessary, DOH provided recommendations on areas of improvement.
- (Round 2) Operational Surveys were initiated for two Partial Capitation plans in prior reporting periods, and are as follows:
- First Partial Capitation plan: The CAP has been received and is under review.
- Second Partial Capitation plan: The CAP has been received and is under review.
- (Round 3) Operational Surveys were initiated for two plans on both their Partial Capitation and MAP lines of business. Initial survey documentation is expected to be received in October 2024.
- One Focused Survey was initiated on all MAP plans based on an analysis of their 2023 Q1 PNDS Submissions in a prior reporting period. Statement of Deficiencies (SOD) were issued to nine plans. Of the nine plans, seven had submitted Partial Capitation CAPs that were inclusive of the MAP line of business, and the remaining two MAP plans were required to submit CAPs. The CAPs have been received and are under review.
- Two Focused Surveys were initiated on one plan for their Partial Capitation and PACE lines of business resulting in two SODs based the identification of expired MSA Agreements. CAPs were received and are being reviewed.
- One Focused Survey was initiated on one plan for their MAP line of business resulting in a SOD based the identification of an expired MSA Agreement. The CAP has been received and is under review.
- One Focused Survey was initiated on all Partial Capitation and MAP plans based on the OSC Audit, Improper Medicaid Managed Care Payments for Durable Medical Equipment, Prosthetics, Orthotics, and Supplies on Behalf of Recipients in Nursing Homes (Report 2023-F-12)to evaluate plan policies and controls. The requested information was received, and no further action is needed at this time.
- One Focused Survey was initiated on MAP and Partial Capitation lines of business for one plan based on their self-disclosure regarding 2,267 notices not being sent out to members, which included approvals, extensions, acknowledgments but also 300 plus denials where the member did not receive fair hearing rights, resulting in a SOD. The CAP has been reviewed and approved.
- One Focused Survey was initiated on one plan based on their non-compliance with annual Social Adult Day Care site evaluation requirements. SODs were issued for their Partial Capitation and MAP lines of business. The CAPs were received and are under review.
- One Focused Survey was initiated on one Partial Capitation plan based on a TAC Complaint (Case #172880) where it was determined the plan failed to provide personal care services, care management, social work support, environmental support, required monthly care management calls and in-person six-month home visits. Additionally, since the plan failed to recognize that the consumer was not receiving core services, the consumer was not educated on the obligations of the program and failed to involuntarily disenroll the consumer in accordance with MLTC Policy 23.03. A SOD has been drafted and is awaiting approval.
- N.Y. Public Health Law § 4403-f. (l l-b) Post Transaction Reporting:
- The Merger between two Partial Capitation plans Post Transaction Review was initiated and the submitted files are under review.
As a matter of routine course:
- Processes for Operational Partial Capitation and MAP surveys continue to be refined;
- The Surveillance tools continue to be updated to reflect process changes.
3. Issues and Problems
There were no issues or problems to report for the July 2024 through September 2024 quarter, nor for the October 2023 through September 2024 annual period.
4. Summary of Self-Directed Options
Self-direction is provided within MLTC plans as a consumer choice and gives individuals and families greater control over services received. The DOH began a procurement process in December 2019 which was subsequently amended in the Executive Budget in April 2022. This procurement process was ultimately repealed in the enacted 2024-25 NYS Budget and was replaced with legislation to procure a single statewide fiscal intermediary. The procurement was issued in June 2024 and a vendor, Public Partnerships LLC (PPL) was awarded on September 30, 2024. Once the contract with PPL is executed, managed care plans will then enter into an administrative service agreement with them as the single statewide fiscal intermediary.
5. Required Quarterly Reporting
Critical incidents: There were 3,314 critical incidents reported for the July 2024 through September 2024 quarter, an increase of 1% from the previous quarter. The names of plans reporting no critical incidents are shared with the surveillance unit for follow up on survey. Critical incidents by plan for this quarter are attached.
For the annual period October 2023 through September 2024, reporting of critical incidents increased by 12% from the previous annual period. During this annual period, DOH issued updated instructions on reporting critical incidents and will continue to monitor plans who report lower than expected.
Complaints and Appeals: For the July 2024 through September 2024 quarter, the top reasons for complaints/appeals changed from last quarter: Dissatisfaction with other covered services, Dissatisfaction with quality of home care (other than lateness or absences), Dissatisfaction with Care Management, Dissatisfaction with member services and plan operations, and Dissatisfaction with Transportation.
Period: 7/1/2024-9/30/2024 (Percentages rounded to nearest whole number) Number of Recipients: 359,307 Complaints Resolved Percent Resolved * # Expedited 3 3 100% # Same Day 2,271 2,271 100% # Standard/Expedited 5,857 4,290 73% Total for this period: 8,131 6,561 81% *Percent Resolved includes grievances opened during previous quarters that are resolved during the current quarter, that can create a percentage greater than 100.
Appeals 10/2023-12/2023 1/2024-3/2024 4/2024-6/2024 7/2024-9/2024 Average for Four Quarters Average Enrollment 331,288 339,930 348,752 359,307 344,819 Total Appeals 10,065 10,918 11,347 11,994 11,081 Appeals per 1,000 30 32 33 33 32 # Decided in favor of Enrollee 1,168 1,150 1,291 1,487 1,274 # Decided against Enrollee 6,765 7,407 8,572 9,101 7,961 # Not decided fully in favor of Enrollee 1,805 2,004 1,209 1,083 1525 # Withdrawn by Enrollee 327 357 275 323 321 # Still pending 1,000 1,200 1,232 1,331 1,191 Average number of days from receipt to decision 7 10 8 8 8
Complaints and Appeals per 1,000 Enrollees by Product Type
July 2024 - September 2024Enrollment Total Complaints Complaints per 1,000 Total Appeals Appeals per 1,000 Partial Capitation Plan Total 299,150 4,470 15 8,888 30 Medicaid Advantage Plus (MAP) Total 50,724 2,484 49 3,019 60 PACE Total 9,507 1,177 123 87 9 Total for All Products: 359,381 8,131 23 11,994 33 Total complaints increased 12% from 7,271 the previous quarter to 8,131 during the July 2024 through September 2024 quarter.
Total appeals increased 6% from 11,347 during the last quarter to 11,994 during the July 2024 through September 2024 quarter.
For the annual period October 2023 through September 2024, the number of complaints increased by 19%, and the number of appeals increased by 19%.
Technical Assistance Center (TAC) Activity
During the July 2024 through September 2024 quarter, TAC opened 922 cases and closed 915 cases. This is higher than the 845 cases opened, and the 805 cases closed from the previous quarter. Upon examination, this quarter's change in cases is equally spread across the different types of case dispositions, outlined in the table below. There was not one specific disposition that caused the change.
76% of Q4 TAC cases were closed in the same month in which they were opened. This is an increase from last quarter's percentage of 73%.
Call Volume 7/1/2024-9/30/2024 Substantiated Complaints 124 Substantiated Complaints with CAP 0 Unsubstantiated Complaints 297 Resolved Without Investigation 10 Inquiries 484 Total Cases Closed 915
The five most common types of calls were related to:
Q4 2024 7/1/2024-9/30/2024 General 22% Aide Service 21% Enrollment 14% Grievance 13% Billing 7% Most of TAC's cases for this quarter were for general inquiries and questions. Complaints regarding home health care services continue to be the highest complaint category.
During the annual period from October 2023 through September 2024, TAC opened 3,898 cases and closed 3,862 cases. The majority of the closed cases are for general questions and inquiries. About 63% of TAC's complaint investigations were found to be unsubstantiated. TAC issued four CAPs in this annual reporting period.
For the entire year, 70% of cases were closed in the same month they were opened. This efficiency decreased over the course of the year, from 74% in October 2023 to 69% in September 2024.
Call Volume 10/1/2023-9/30/2024 Substantiated Complaints 477 Substantiated Complaints With CAP 4 Unsubstantiated Complaints 1,217 Resolved Without Investigation 249 Inquiries 1,915 Total 3,862
The five most common types of calls were related to:
Types of Calls 10/1/2023-9/30/2024 General 21% Grievance 19% Aide Service 16% Enrollment 12% Billing 8% Most of TAC's cases for this year were for general inquiries and questions. Complaints regarding grievances were the highest complaint category.
Evaluations for enrollment: The New York Independent Assessor Program (NYIAP) is conducting initial assessments and clinical exams for personal care and consumer directed personal assistance services as well as continuing to determine MLTC eligibility. For the July 2024 through September 2024 quarter, 8,925 people were evaluated, deemed eligible and enrolled into plans, a decrease of 3% from the previous quarter.
This brings the total for the annual period October 2023 through September 2024 to 35,114.
Rebalancing Efforts 7/2024-9/2024 Enrollees who joined the plan as part of their community discharge plan and returned to the community this quarter 330 Plan enrollees who are or have been admitted to a nursing home for any length of stay and who return to the community 1,576 As of September 30, 2024, there were 3,186 current plan enrollees who were in a nursing homes as permanent placements, a 6% decrease from the previous quarter.
D. Children's Waiver
On August 2, 2019, CMS approved the Children's 1115 Waiver, with the goal of creating a streamlined model of care for children and youth under 21 years of age with HCBS needs, including medically fragile children, children with a BH needs, children with medical fragility and developmental disabilities, and children in foster care with developmental disabilities, by allowing managed care authority for their HCBS. The Children's Waiver Renewal that was submitted to CMS in January 2022, and extended in April 2022, was approved on June 29 , 2022, for an effective date of April 1, 2022. Additionally, two new Children's Waiver
Amendments were approved by CMS on November 1, 2023, and March 1, 2024, to amend a number of activities detailed in the sections below.
Specifically, the Children's 1115 Waiver provides the following:
- Managed care authority for HCBS provided to medically fragile children and/or with developmental disabilities, developmental disability in foster care, and children with a serious emotional disturbance.
- Authority to include current FFS HCBS authorized under the State's newly consolidated 1915c Children's Waiver in MMC benefit packages.
- Authority to mandatorily enroll into managed care the children receiving HCBS via the 1915c Children's Waiver.
- Authority to waive deeming of income and resources, if applicable, for all medically needy "Family of One" children (Fo1 children) who will lose their Medicaid eligibility as a result of them no longer receiving at least one 1915c service due to case management now being covered outside of the 1915c Children's Waiver, including non-Supplemental Security Income Fo1 children. The children will be targeted for Medicaid eligibility based on risk factors and institutional level of care and needs.
- Authority to institute an enrollment cap for Fo1 children who attain Medicaid eligibility via the 1115.
- Authority for Health Home care management monthly monitoring as an HCBS; and
- Removes managed care exclusion of children placed with Voluntary Foster Care Agencies.
Given the approval, the NYS DOH has been engaged in implementation activities, including, but not limited to the following:
- Continuing to refine data collection and data analysis to ensure accurate reporting.
- Engaging a contract vendor for performance and quality monitoring for all elements of the Children's Redesign, including the Children's 1115 Waiver, to ensure consistency and quality in all elements of the initiative.
- Submitted the Preliminary Interim Evaluation Report to CMS, as drafted by the vendor.
- Submitted the Interim Evaluation Report to CMS, as drafted by the vendor.
- Drafting policies and guidance to ensure compliance with State and Federal requirements, as well as working with service providers to confirm understanding and compliance with requirements such as the CMS HCBS Settings Final Rule and Electronic Visitor Verification (EVV).
- Updating manuals, guidance documents, forms and online resources as indicated.
- Reassessing, streamlining, and removing unnecessary or duplicative forms to alleviate administrative burden.
- Conducting refresher training sessions and offering more in-depth training for care managers and HCBS providers, including additional resources and technical assistance with person-centered planning.
- Facilitating relationship building between MCOs, HCBS providers, and care managers to improve communication and care coordination.
- Coordinating stakeholder meetings to obtain feedback from MCOs, Health Homes, HCBS providers, advocate groups, Regional Planning Consortiums, and others regarding the Medicaid Redesign and implementation.
- Evaluating accuracy of MCOs and FFS billing and claiming data.
- Defining performance and quality metrics.
- Responded to the COVID-19 pandemic and implementing emergency 1135 and Appendix K, inclusive of a Retainer Payment for Day and Community Habilitation providers - and supported the recovery of impacted providers and consumers.
- Assisted with a strategic plan for the unwind of the COVID-19 PHE.
- Released a PHE Unwind plan for flexibilities related to the Medicaid Children's Waiver and Health Home Services.
- Working with Health Homes and HCBS providers to enhance capacity monitoring and streamline the referral process.
- Worked with HCBS providers and MMC plans to streamline the authorization process.
- Engaged with providers to understand barriers to service delivery - such as workforce challenges, lack of referral sources/lack of service awareness, travel time for families in rural areas, etc. - and solutions to address these concerns, including launching a state- wide capacity tracking system to monitor waitlists, provider capacity, allow for provider reporting and assess metrics regarding highly utilized HCBS, underutilized HCBS, and overutilized providers.
- Modified the state-wide capacity tracking system, which is based on provider self- reporting, to enhance the understanding of the HCBS waitlist and who is being served by HCBS. An electronic referral and authorization portal was launched, which will provide more accurate information that is not dependent upon self-reports of providers.
- Engaged with providers, consumers, and NYS agency partners to determine how best to use the eFMAP authorized by ARPA to improve access to children's services and reduce administrative burden on providers - including increasing rates for HCBS and directing funding to service providers for workforce development and IT infrastructure.
- Collected stakeholder feedback (from consumers, HCBS providers, Health Homes, MCOs, and advocate groups) to inform the 1915c Children's Waiver renewal - including suggestions on how to streamline the Managed Care processes and improve communication between MCOs, Health Homes, and HCBS providers.
- Organized and conducted workgroups of Health Homes, MCOs, and HCBS Providers to ensure feedback is addressed relating to the referral process and authorization process.
- Engaged with Health Homes, MCOs, and HCBS providers while redesigning the Plan of Care in preparation for digitization.
- Updated public-facing materials to better inform Medicaid members of the available options and help service recipients understand the process.
- Submitted the 1915c Children's Waiver Extension to CMS.
- Submitted the 1915c Children's Waiver Renewal to CMS.
- Submitted a State Transition Plan to CMS to detail how agencies providing services under the 1915c Waiver comply with the HCBS Final Rule.
- Submitted a preprint to CMS for the disbursement of ARPA funding to support and enhance HCBS workforce and infrastructure.
- Worked with MCOs and providers to disseminate ARPA funding through the directed payment process.
- Scheduled and facilitated regional meetings with HCBS providers, Health Homes, care management agencies, Medicaid MCOs to resume in-person collaboration and dialogue.
- Updated the Incident and Reporting Management System (IRAMS) and Children's Capacity Tracker to have updated functionalities to track service delivery and waitlist information.
- Engaged with HCBS providers to re-designate for the Children's Waiver, including collecting updated attestations confirming providers understand and will adhere to all policies and compliance requirements; also provided technical assistance and connection to referral sources for providers who are working to get their HCBS programs up-and running and/or de-designated agencies for all or some services if they are not currently able to actively deliver HCBS.
- Submitted additional preprint to CMS for the disbursement of ARPA funding to support children in need of receiving Environmental Modifications (EMod), Vehicle Modifications (VMod) & Adaptive and Assistive Technology (AATs).
- Conducted Final Rule compliance reviews with newly designated HCBS providers.
- Monitored staff compliance with training and background check requirements through IRAMS.
- Updated and issued the Children's Care Management Authorization and Referral Forms ensuring inclusivity of all requirements per stakeholder feedback.
- Updated IRAMS User Guide used by HH, CMA, HCBS Providers, and C-YES to report critical incidents and complaints/grievances as appropriate for the various populations served to ensure the health, safety, and well-being of members.
- Updated and posted the HCBS Referral and Authorization Portal User Guide and FAQ.
- Hosted webinars providing training and technical assistance on use of the Referral and Authorization Portal.
- Updated and posted documentation and guidance related to HCBS eligibility and enrollment.
Additionally, the NYS DOH has been implementing and altering activities and services, including, but not limited to, the following:
- Submitted Disaster SPA 21-0054, for Health Home one-time assessment fee per member retroactive April 1, 2021, to September 30, 2022.
- Submitted a SPA 22-0088, which would continue the assessment fee effective October 1, 2022.
- Updated documentation and provided guidance to providers regarding the HCBS name changes for "Palliative Care: Counseling and Support Services" (previously "Palliative Care: Bereavement") and "Adaptive and Assistive Technology" (previously "Adaptive and Assistive Equipment").
- Updated documentation and provided guidance to providers regarding the consolidated HCBS of "Caregiver and Family Support and Services" and "Community Self-Advocacy Support" into a new service referred to as "Caregiver/Family Advocacy and Support Services". This combination allowed for a broader array of providers to deliver the service and also broadens the definition of caregivers eligible for training to include all individuals who supervise and care for members.
- Broadened Children and Youth Evaluation Services' (C-YES') Nurse qualifications by requiring two years relevantexperience. The previous requirement that was two years' experience specificallyin home care.
- Reduced the required years of experience for Palliative Care: Expressive Therapists from three years to one year.
- Added a temporary 25% rate adjustment consistent with the approved Spending Plan for Implementation of the ARPA Section 9817 to improve service capacity.
- Added a 5.4% COLA increase for providers starting April 1, 2022.
- NYS supported the continued 25% enhanced HCBS rates on October 1, 2022.
- Added a 4% COLA increase for providers effective November 1, 2023.
- Effective December 1, 2023, rural rate for seven counties was implemented to improve access to services.
- Transitioned the EMod, VMod, and AAT to a Financial Management Service, starting March 1, 2024, based upon approval for Children's Waiver amendment.
- Implemented a 2.84.% COLA increase for Children's HCBS effective April 1, 2024.
- Effective October 1, 2024, MMCP capitation payments were adjusted to include risk- based premium adjustments for Children's Waiver HCBS.
- Developed Electronic Children's Services Staff Compliance Tracker.
- Released the Electronic Children's HCBS Referral and Authorization Portal, which streamlines, standardizes, and ensures timely completion of HCBS referrals and authorizations.
The above-listed activities will help to facilitate oversight and the provision of high-quality services, ensure that the goals of the Children's 1115 Waiver are achieved, and provide the necessary data elements to fulfill future reporting requirements.
The following table demonstrated the number of children enrolled in the 1915c Children's Waiver identified by NYS restriction exception (RE) code of K1 and the current claims for services for these enrolled children/youth. Additionally, as outlined in the 1115 amendment, NYS tracked the enrollment of children/youth who obtained Medicaid through Fo1 Medicaid budgeting as identified by NYS RE code KK. Therefore, the table below also demonstrates the number of children enrolled with this KK flag and the current claims for services for these enrolled children.
This table includes Quarter 4 data from 7/1/2024-9/30/2024 of FY2024.
With K1 Flag - HCBS LOC With KK Flag - Family of One Month Enrolled
ChildrenEnrolled
Children with
HCBS ClaimsEnrolled
ChildrenEnrolled Children
with HCBS Claims10/1/2023 11,627 5,737 1,536 293 11/1/2023 11,280 5,821 1,522 308 12/1/2023 10,838 5,648 1,519 328 Quarter 1 Unique 12,103 6,716 1,577 382 1/1/2024 10,741 5,757 1,527 328 2/1/2024 10,605 5,783 1,512 321 3/1/2024 10,286 5,820 1,507 326 Quarter 2 Unique 11,311 6,630 1,571 391 4/1/2024 10,115 5,690 1,487 331 5/1/2024 10,090 5,780 1,471 333 6/1/2024 10,010 5,645 1,473 313 Quarter 3 Unique 10,606 6,497 1,527 418 7/1/2024 9,889 5,512 1,465 291 8/1/2024 9,756 5,253 1,450 298 9/1/2024 9,576 3,610 1,439 246 Quarter 4 Unique 10,285 6,166 1,502 373 Annual Unique 14,044 8,862 1,767 592 *There is an expected 3-month lag for claims data that may impact the enrolled children with an HCBS claim data.
E. New York Health Equity Reform (NYHER) Amendment
The NYHER 1115 Amendment was approved by CMS on January 9, 2024, and will remain in effect throughout the remainder of the demonstration period. The primary goal of the amendment is "to advance health equity, reduce health disparities, and support the delivery of HRSN." The State seeks to build on the investments, achievements, and lessons learned from the DSRIP 1115 waiver program to scale delivery system transformation, improve population health and quality, deepen integration across the delivery system, and improve access to HRSN services. This will be achieved through targeted and interconnected investments that will augment each other, be directionally aligned, and be tied to accountability. These investments are focused on HRSN services, population health improvement, and increasing workforce capacity.
1. Social Care Networks and HRSN Services
NYS aims to integrate social care with physical and behavioral health care for Medicaid Members in the state by establishing regional Social Care Networks (SCNs) to provide screening, navigation, and delivery of HRSN services. Nine SCN lead entities were selected from among 32 qualified applicants through a competitive Request for Application (RFA) procurement process. These lead entities will create and maintain a network of contracted HRSN service providers with the capacity to screen Medicaid Members for HRSNs, provide navigation to existing federal, state, local, and nonprofit programs or to enhanced HRSN services through the SCN, and deliver enhanced HRSN services to eligible MMC members to address their HRSNs in the domains of housing, nutrition, transportation, and social care management.
Following the public announcement on August 7, 2024, NYS DOH executed contracts with all SCN lead entities by September 2024. NYS DOH is committed to comprehensively supporting each SCN to ensure positive impact throughout and beyond the demonstration period. NYS DOH aims to ensure that each Medicaid Member will receive an HRSN screening annually or following a major life event. Members will be screened using a New York State-standardized version of the Accountable Health Communities (AHC) HRSN screening tool with 12 questions to assess Member needs in the domains of housing, nutrition, transportation, and social care management. Each SCN will embed the screening tool in its IT Platform and have different modalities for conducting screening to ensure broad access (e.g., screening conducted by social care Navigators, health care providers, Member self-screen, etc.). The IT Platform will also have a closed-loop referral functionality to ensure that Members with identified needs receive timely navigation to social care services and Navigators can track service referral outcomes. In addition, the State has set expectations that national social care data standards be adopted into the SCN's conventions for the following program activities: screening (LOINC), assessing (SNOMED-CT, ICD-10), referral (SNOMED-CT), and provisioning enhanced HRSN services (SNOMED-CT, HCPCS). By using these data standards, NYS and participating organizations in the SCN program can more effectively coordinate and measure program activities and impact.
Status Updates
HRSN Implementation Activities: HRSN services are slated to launch on January 1, 2025. NYS DOH is focused not only on preparing for SCN program launch, but also in maintaining a sustainable positive impact on Members and communities. To this end, the State has been engaged in the following program implementation activities:
Operational Readiness
- Provided extensive, in-depth guidance to SCN Lead Entities
- Published a comprehensive Operations Manual to serve as guidance for SCN Lead Entities. The Manual provides program, billing, and data guidance, defines roles and responsibilities of key partners, and details requirements governing the delivery of HRSN services across the four domains of housing, HRSN transportation, nutrition, and social care management. The Manual also outlines instructions related to data security, submitting reports, and data coding (e.g., ICD-10, SNOMED-CT).
- As companion to the manual, produced Frequently Asked Questions (FAQ) guides with additional detail on commonly asked questions and complex workflows, answering over 100 questions spanning operations, finance, and technical domains.
- Hosted one-on-one sessions with each SCN Lead Entity, with NYS DOH leadership meeting with SCN leadership to support progress against a readiness checklist. Readiness domains include contracting, payments, Data & IT, Reporting and Performance Management, Network Access and Capacity, Partnerships, Member / Provider Outreach and Engagement, and Governance.
- Hosted five webinars for Lead Entities with opportunity for Q&A, on topics including SCN data and IT platforms, enhanced HRSN services and delivery workflows, performance management (i.e., reporting required and how the State will use reports to support SCN success), HRSN fee schedule, and more complex workflows for medical respite, home accessibility and safety modifications / home remediation, and asthma remediation.
- Established and led weekly office hours for SCN Lead Entities to troubleshoot issues and enable preparation for program launch.
- Facilitated a learning collaborative for SCN Lead Entities focused on CBO Capacity Funds, fostering candid discussions on challenges and successes while sharing innovative best practices and actionable insights.
- Provided guidance to SCN Lead Entities to support development of region- specific fee schedules that reflect cost of delivering services in each region.
- Developed agreement templates for contracting between MCOs and SCNs, and between SCNs and HRSN service providers. Solicited feedback on draft templates from relevant stakeholders (e.g., Lead Entities, MCO Plan Associations); monitored progress of contracting between ecosystem partners.
Technical Development
- Created a mapping from NYHER activities to SNOMED codes and Fast Healthcare Interoperability Resource (FHIR) through engagement with the Gravity Terminology team. The mapping aligns with national social care data standards for screening (LOINC), assessment (SNOMED-CT, ICD-10), referral (SNOMED-CT), and provisioning HRSN services (SNOMED-CT, HCPCS). These were incorporated into the Operations Manual to further advise the SCN Lead Entities.
- Created a SHIN-NY FHIR Implementation Guide. This 1115 SHIN-NY FHIR Implementation Guide was created for the exchange of HRSN data for NYS NYHER 1115 Waiver Amendment. Specifically, this guide defines FHIR exchange between an organization supporting the Waiver and a Qualified Entity (QE) here in NYS. Link to SHIN-NY FHIR Implementation Guide5.
- Established a data lake and Master Person Index for Medicaid Members through collaboration with New York ehealth Collaborative (NYeC), designed and tested the integration of healthcare and social care data, and worked to connect nine SCN Lead Entities to regional QEs for data exchange via the SHIN-NY platform.
- Defined the Minimal Viable Dataset (MVD), drafted initial use cases for the NYS DOH data book, and began building NYHER-focused datamarts to support future HRSN data products that support business intelligence and program oversight through horizon reports within NYS DOH.
- Created detailed business requirements (DBRs) for each of the metrics across phases of implementation by identifying the logic for calculating each of the metrics using elements of the MVD and specifying assumptions and exclusions across each metric.
- Developed connections between critical systems, including QEs, SHIN-NY data lake, and the DOH Medicaid Data Warehouse, ensuring seamless data flow for NYHER.
- Developed and tested the MCO Enhanced Member Services Files and worked closely with NYeC to develop a comprehensive SCN / SHIN-NY Interoperability Guide and FHIR-based implementation guide.
- Conducted extensive testing to validate data exchange, including pushing 350K sample screening records to the Medicaid Data Warehouse.
- Designed, built, and tested multiple data reporting templates (e.g., allowing SCNs to manage performance, track infrastructure spending, and assess SCN adequacy, ensuring interoperability and consistent data exchange across regions).
- Designed SCN Performance Management Dashboards (e.g., with stakeholder input, defined detailed business requirements (DBRs), set up data flows). Created SCN Lead Entity guidance to drive performance management activity once data begins to flow.
Stakeholder Engagement
- Hosted regular NYHER Systems Workgroups focused on providing MCOs and SCNs information on billing, claims, and other technical guidance.
- Engaged MCOs in monthly meetings on their roles and responsibilities in the SCN program; presented to New York MCO Medical Directors with considerations for their clinical teams related to the SCN program.
- Presented at numerous conferences to engage broader stakeholders (e.g., housing support service providers at OTDA (Office of Temporary and Disability Assistance) Housing Bureau meetings, nutrition service providers at Food as Medicine convening, etc.).
- Kept DOH website up-to-date with relevant SCN program information, including selected SCN Lead Entities and their website, information tailored to healthcare providers or HRSN service providers, etc.
HRSN: Monitoring Metrics for Contracted or Participating Organizations
Performance management will be a collaboration between NYS DOH and SCN Lead Entities. The State's goal is to enable timely and actionable improvements for SCNs to achieve 1115 demonstration objectives. Performance management reports will help facilitate ongoing engagement between NYS DOH and SCN Lead Entities, as well as a robust evaluation design.As part of the performance management approach, SCN Lead Entities will be responsible for generating specific inbound reports both before the program's start and on an ongoing basis. Complementing these SCN-generated reports will be a set of NYS DOH generated outbound reports. These outbound reports from NYS DOH will provide SCN Lead Entities with transparency into their performance (and peer performance) and enable continuous improvement.
In addition to planned reporting, SCN Lead Entities will be expected to submit real-time updates to the State to enable timely assessment and management of SCN operations. The real-time updates include but are not limited to network changes, governing body changes, and changes to SCN Lead Entity financials.
HRSN Performance Metrics: NYS will be tracking performance metrics throughout the program to describe progress quantitatively. Baseline data will be collected, and progress will be shown over time. Data will also be stratified by key demographic subpopulations of interest. The State is exploring ways to use these and other metrics to demonstrate impact on quality, access, outcomes, and medical cost for Medicaid (with an objective of program success not only through the demonstration period, but long-term).
IT and data systems are fundamental to the delivery, monitoring, and assessment of impact of HRSN services. NYS DOH has held ongoing meetings with IT partners (including the Gravity Project, SHIN-NY qualified entities, and NYeC) to gather technical requirements and best practices to ensure each SCN IT Platform vendor creates or enhances their products to become interoperable and capable of meeting local, state, and federal stakeholder needs and requirements.
Maintenance of Effort (MOE)
The MOE Baseline Estimate and Plan was submitted to CMS on April 8, 2024. As of this reporting period, spending levels have been maintained or increased. DOH continues to adhere to all MOE requirements.HRSN: Operational Updates - Challenges Addressed
The below reflects key challenges encountered, underlying causes, actions taken to address them, and lessons learned (including some that may apply for other states contemplating similar programs). Key achievements and the efforts to which these successes can be attributed are outlined in the HRSN Implementation Activities section of this report.Complex IT infrastructure build and data sharing among multiple stakeholders
NYS DOH is committed to establishing a robust data and IT infrastructure to support the goals of the SCN program, including expanding access to HRSN services, advancing health equity, and ensuring accountability through accurate impact measurement. This requires data sharing and collaboration among diverse stakeholders, including SCN Lead Entities, MCOs, HRSN service providers, and healthcare organizations. It also requires coordination of multiple types of data - social care, healthcare, payment / financial - which adds inherent complexity and introduces a need to navigate silos between distinct healthcare and social service systems.To address these interoperability challenges, the NYHER program has built infrastructure to pull multiple datasets into a single system. NYS DOH took a proactive and collaborative approach with SHIN-NY stakeholders including NYeC, qualified entities, and other agencies involved, hosting regular workgroups, identifying all data flows that would be required early on, and creating a calendar for testing activities. The State also worked closely with SCN Lead Entities and their IT platform vendors to clarify technical requirements, security requirements, resolve issues, and ensure alignment. Privacy and security-focused sessions were added to address the high standards required for social care, healthcare, and financial / payment data exchange. Additionally, NYS DOH has provided stakeholders with regularly updated guidance and templates for data-sharing agreements. These efforts increase the likelihood that all parties are equipped to navigate the complexities of IT infrastructure and data-sharing.
Managing SCN Lead Entity readiness:
Implementing a standardized and comprehensive readiness checklist or assessment was a key piece of success in the State's ability to support SCN Lead Entities in preparing for the program. It enabled structured conversations during one-on-one meetings. It also provided a clear and intuitive snapshot to NYS DOH and Lead Entity executives stakeholders when needing to escalate any particular risk (i.e., an area in which a Lead Entity may be behind or have less mature capabilities).
2. Workforce
NYS is implementing two statewide workforce initiatives, Career Pathways Training (CPT) and Student Loan Repayment (SLR) to support workforce recruitment and retention and increase supply of high-demand physical health, BH, and social care providers.
Career Pathways Training: To address workforce shortages, the CPT Program will fund education and training activities and provide job placement support for health workers newly entering the workforce or advancing their careers. Participants in the CPT Program will make a three-year commitment of service, in their new professional title, to providers who serve at least 30% Medicaid members and/or uninsured individuals. The program is organized to support two career pipelines, New Careers in Healthcare for individuals newly entering the healthcare workforce, and Healthcare Career Advancement for individuals currently in the healthcare workforce. Professional titles eligible for this program include nursing, professional technical, and frontline healthcare workers.
Workforce Investment Organizations (WIOs): In Q4 2024, the NYS executed contracts with three regional Workforce Investment Organizations (WIOs), following the Governor's public announcement on August 15. The WIOs are:
- Region 1 (Hudson Valley, New York City, and Long Island): 1199SEIU Training and Employment Funds
- Region 2 (North Country, Capital Region, Southern Tier, and Central New York): Caring Gene Healthcare Career Pathways
- Region 3 (Finger Lakes and Western New York): Finger Lakes Performing Provider System
The three WIOs were chosen from existing WIOs first established as part of the 2018 Managed Long Term Care Workforce Investment Program (MLTC WIP). WIOs were evaluated and selected using the following criteria: deep connections to their respective regions; demonstrated success in operationalizing workforce training programs; expansion beyond the MLTC WIP titles; and capacity to stand up the CPT program rapidly and effectively in their region. The selected WIOs will partner with job training and educational institutions, providers, and SCNs and be responsible for conducting outreach to recruit prospective students and providers. WIOs will utilize recruitment toolkits and multimedia campaigns to target diverse participants, and ultimately, increase diversity of the workforce.
In addition to CPT program infrastructure and administration, the WIOs will provide support for participants to ensure completion of programs, including case management, tutoring, other academic support, coordinated educational programs; payments for books, academic fees, and backfill for current employees' time spent in training programs. They will also provide support in job placement and career supports to meet service commitments. WIOs will monitor student performance to understand where they can provide additional support as early as possible during the semester.
CPT Implementation Activities: NYS DOH has engaged in activities including but not limited to the following:
- Finalized year one budgets and work plans for each WIO.
- Executed contracts with each WIO in September 2024, including initial payments to begin immediate program implementation.
- Reviewed and approved WIO marketing materials to enable recruitment through conferences, partnerships, and other public channels.
- Launched monthly one-on-one meetings with WIOs to support program execution.
- Distributed draft program guidance and finalized program design decisions.
- Engaged potential partners in disseminating information about the CPT program, including the OMH and OASAS given importance of filling behavioral health roles to serve Medicaid Members.
CPT: Monitoring Metrics for Contracted WIOs
NYS DOH is committed to performance enablement of WIOs, which requires understanding their progress, strengths, and any needs that the State can help address. NYS DOH's goal is to support timely and actionable improvements for WIOs to achieve 1115 Waiver objectives. A regular reporting cadence will facilitate ongoing engagement between the State and WIOs and will enable robust evaluation design.
As part of the performance enablement approach, WIOs will be responsible for generating specific data on an ongoing basis. A summary overview table of required inbound reports from WIOs to NYS DOH is below.
Report Name Description Cadence Narrative / Qualitative Report Summarizes the services rendered during the quarter and details how the Contractor has progressed toward attaining the qualitative goals enumerated in the workplan. The report addresses all goals and objectives of the program and includes a discussion of problems encountered and steps taken to solve them. Quarterly Performance Metrics Report Summarizes the quantitative aspects of the program plan (e.g., number of applicants, number of individuals who enrolled by program, etc.) Quarterly Cost Report Comprehensive financial report, including the Budget Statement and Reporting of Expenditures (BSROE). This includes all quarterly expenses reported against approved budget expenses. Quarterly Annual Budget Created by WIO and confirmed by NYS DOH; the budget is the source data for determining WIO quarterly spending. Annually Workforce Performance Metrics: The State will be tracking the following quantitative performance metrics; additional metrics may be added as program design continues or evolves. Baseline data will be collected and reported on over time. Data will also be stratified by demographic subpopulations, as applicable.
- Number of enrolled students
- Number of students completing educational or training program
- Number of students who have obtained a requisite credential
- Number of students meeting three-year service commitment at provider serving 30% Medicaid and/or uninsured individuals
- Regional vacancy rates by title
Student Loan Repayment: To support recruitment and retention of high-demand practitioners, healthcare professionals who make a four-year commitment to maintain a personal practice panel or work at an organization that includes at least 30% Medicaid and/or uninsured members may be eligible for student loan repayment. Healthcare titles eligible for repayment include psychiatrists, with a priority on child/adolescent psychiatrists; primary care physicians and dentists; and nurse practitioners and pediatric clinical nurse specialists. The State has engaged in in-depth planning to identify program and eligibility parameters, develop application and monitoring processes, define priority partners and initiate outreach, and consider additional aspects of the program's design and implementation. The application process will consider, among other factors, geographic distribution of applicants, regional needs to ensure the program benefits high-needs communities, and linguistic and cultural competency of applicants. NYS DOH is in the process of selecting a vendor to administer the program and is preparing to open applications for Student Loan Repayment in 2025.
Workforce: Operational Updates - Challenges Addressed
The information below reflects key operational, policy, or administrative challenges encountered, the underlying causes, and actions taken to address these issues and increase alignment with program goals. Key achievements and the efforts to which these successes can be attributed are outlined in the Implementation Activities section of this report.WIOs faced a short turnaround time to initiate recruitment and enrollment activities for CPT. To address, NYS DOH provided tailored support to each WIO in monthly one-on-one meetings while also encouraging collaboration and shared learning between the WIOs given their complementary areas of expertise. The three WIOs submitted consolidated lists of questions to the State, demonstrating their partnership and ongoing coordination for a more successful statewide program.
NYS's efforts to enable a rapid program start after WIO selection has generated several lessons learned. First, the collaboration between WIOs supported a rapid program start - e.g., WIOs sent in consolidated questions for a faster turnaround of clarifications. Convening WIOs to facilitate knowledge-sharing and best practices is critical for any state establishing a similar program. NYS DOH also learned during Q4 that beyond capabilities in recruitment and enrollment, visibility into each WIO's preparedness to place students upon completion of the program is key. For titles with shorter educational programs that may be only a few months long, such as Community Health Workers (CHWs), it is essential to have employment opportunities fully established ahead of student enrollment. Moreover, NYS DOH translated lessons learned from the SCN program and vice versa to strengthen both WIO and SCN operations. Efforts are underway to facilitate connections between WIOs and SCNs by region and will be accelerated going forward with the help of the HERO.
3. Health Equity Regional Organization (HERO)
The NYS HERO will be wholly dedicated to advancing health equity and closing health disparities in a data-driven way across NYS. The HERO will be an independent statewide entity responsible for data aggregation for health and social care data to support population health improvement activities; regional needs assessment and planning to identify health equity-related needs, service delivery, and workforce-related gaps contributing to health disparities; value- based payment (VBP) design and development that addresses health, behavioral health and HRSNs; and program evaluation through an ongoing review of waiver programs and access to new services to support continuous improvement in program design, implementation, and impact. In Q4, the State continued to build out the HERO design, activities, and requirements with a focus on contracting. HERO health equity planning work is anticipated to begin in 2025.
Next steps include executing the HERO contract in Q1. NYS DOH will then partner with the HERO entity to set it up for success, including ensuring it builds on work to date. The HERO will operate independently to produce research and support data-driven strategic planning for entities across the state.
4. Medicaid Hospital Global Budget Initiative (MHGBI)
The goal of the MHGBI is to stabilize and transform targeted financially distressed voluntary hospitals to advance health equity and improve population health in communities with the most evidence of health disparities. This goal aligns with the Center for Medicare and Medicaid Innovation (CMMI) States Advancing All-Payer Health Equity Approaches and Development (AHEAD) model. This initiative is structured through incentive funding to stabilize Medicaid- dependent financially distressed safety net hospitals and develop necessary capabilities to advance health equity; transition to global budget models; participate in advanced VBP arrangements; and deepen integration with primary care, BH, and HRSN services.
Participating hospitals will be required to submit hospital health equity plans that align with statewide priorities, participate in quality improvement activities that address community specific health disparities in alignment with health equity plans, and create a roadmap outlining activities required to transition to a global budget and support community wide population health.
On March 26, 2024, the NYS submitted a Letter of Intent (LOI) expressing the desire to partner with CMS to design and implement the AHEAD model. This submission also included the LOI's from all hospitals eligible for MHGBI. On March 31, 2024, the State submitted a detailed plan for how participating hospitals will collect beneficiary demographic and HRSN data and related metrics. NYS is considering questions around the region definition, timing, and path to authority in Fee For Service and Managed Care for the MHGBI. The State's view was documented in its application to participate in the AHEAD demonstration during the second Notice of Funding Opportunity (NOFO) period with Cohort 3. The State submitted its application on August 12, 2024.
After the application was submitted, NYS focused on pre-implementation activities such as developing a detailed workplan, conducting a data and IT infrastructure gap analysis, and drafting a pre-implementation roadmap. The State plans to begin engaging and recruiting providers for the AHEAD model after the award announcement, scheduled for October 2024.
MHGBI Implementation Activities: NYS DOH has been engaged in implementation activities, including but not limited to the following:
- Submitted AHEAD application August 12, 2024.
- Drafted an internal pre-implementation roadmap for AHEAD, covering HGB model design, operations, hospital technical assistance, including other key areas.
- Developed a preliminary, internal perspective across elements of the Medicaid HGB model top-of-mind for stakeholders (e.g., shared savings with PCPs, supplemental payments, and total cost of care (TCOC) performance adjustment).
- Drafted and reviewed internal strategies to help hospitals meet 1115 Waiver requirements and internal pre-implementation roadmap, in preparation for HGB.
- Explored required payment authorities for HGB payments in both fee-for-service and managed care populations.
- Preliminarily identified potential impacts of HGB implementation on hospital partnerships.
- Conducted an internal, preliminary assessment of National Association of Health Data Organizations (NAHDO) non-claims payment data layout for integration into All Payer Claims Database (APD).
- Developed templates for 1115 MHGBI deliverables.
Performance Metrics:
Performance metrics may be included in future reports as available. Examples include number of planned initiatives by hospital, compliance on quality data submission, percentage of key milestones achieved across hospitals, and incremental members with enhanced demographics and HRSN data collected.
MHGBI: Operational Updates - Challenges Addressed
One potential challenge is that NYS may need multiple regulatory mechanisms, including a new 1115 Waiver, to authorize HGB payments across its Medicaid population, which is divided between MMC and FFS beneficiaries. Aligning the regulatory pathway and securing timely approval from CMCS could be difficult for the planned April 2027 implementation. To address this, the State is engaging CMCS early and drafting a written proposal with key questions on the regulatory pathway and timing.
5. Provider Payment Rate Increase
In accordance with STCs 7.1 through 7.12, DOH attests that the Primary Care Services, Obstetric Care Services, and Behavior Health Care Services categories continue to meet a ratio at or above 80 percent in both fee-for-service and managed care delivery systems.
F. IMD Transformation Demonstration
State and National Medicaid Redesign initiatives recognized the critical role of SUD services; including residential treatment services, within the full continuum of services required to meet the triple aim of improving the quality/experience of care, improving the health of populations, and reducing per capita costs of health care.
Historically, Federal and NYS Medicaid funding authorities (e.g., SPA and 1115 waivers) did not provide coverage for residential treatment. As such, this level of treatment was not included in either the Medicaid FFS or MMC benefit package. Therefore, individuals were frequently served in higher levels of care than clinically appropriate (i.e., withdrawal management and inpatient treatment) and care coordination was fragmented between physical and BH services.
Individuals experienced difficulty with transitioning from the hospital/inpatient setting to the residential level of care and often had re-admissions to higher levels of care.
To address this gap in the treatment continuum, The Federal ACA/Parity Legislation, the NYS 1115 MMC Waiver Program, and New York SPA's: 16-0004, 21-0064, NY-23-0003 were amended to support strengthening residential services within the full continuum of services. Collectively, these required OASAS Certified residential SUD programs and their treatment services to be covered by Medicaid and included within the required MMC benefit package. Via the changes to the 1115 Waiver and the 1115 Waiver NYHER and IMD transformation amendments, NYS received comprehensive Federal approval for the residential redesign initiative. The collective Federal approvals support NYS' community based residential levels of care that provide a safe environment for Medicaid recipients who are: beginning opioid treatment, experiencing mild to moderate withdrawal or significant urges or cravings that cannot be managed, or have mental health symptoms that are not stable. Residential Redesign is a cornerstone to NYS's ability to respond to this need by strengthening community service access as alternatives to detoxification and providing recovery oriented, supportive residential step downs.
OASAS Certified Title 14 NYCRR Part 820 Residential Service Programs: Service Description:
- Part 820 programs are designed to help persons who lack a safe and supportive residential option in the community to achieve changes in their SUD behaviors within an appropriate setting. The Part 820 Residential Model has three elements of care:
Stabilization: Requires the supervision of a physician and clinical monitoring to address: Mild to moderate withdrawal, severe cravings, psychiatric and medical symptoms, emotional crisis. Individuals will receive medically directed care to stabilize acute medical, mental health and addiction symptoms. For patients who seek services at the emergency department and who are not in need of a hospital-level detox, the stabilization element will offer an alternative and provide these patients a safe place to stabilize and engage in treatment.
Rehabilitation: Staffing to provide monitoring, support and case management. Designed for individuals with significant functional impairment related to: Social skills, employment, inability to follow social norms and maintaining housing.
Reintegration: in a congregate setting or scattered site setting will provide:
Opportunities to actualize skills learned in treatment in the community; Linkages to community services/resources; Services for those transitioning to long term recovery and independent living. Staffing includes case managers, housing experts, employment supports, recovery wellness.- Medication for addiction treatment - the Part 820 Programs6 Regulations:
Require that Individuals receive medically directed care to stabilize acute medical, mental health and addiction symptoms. For patients who seek services at the emergency department and who are not in need of a hospital-level detox, the stabilization element will offer an alternative and provide these patients a safe place to stabilize and engage in treatment. To facilitate access to full opioid agonist medication for patients who are maintained on such medication at the time of admission or who choose to start such medication during admission, the program shall develop a formal agreement with at least one Opioid Treatment Program (OTP) certified by OASAS to facilitate patient access to full opioid agonist medication, if clinically appropriate.
Developing the Title 14 NYCRR Part 820 Provider Network:
- Effective 2015, OASAS began the process of re-designating all approved OASAS certified residential programs from Title 14 NYCRR Part 819 and Title 14 NYCRR Part 816.9 to Title 14 NYCRR Part 820 programs.
- Comprehensive Title 14 NYCRR Program regulations were enacted to define the Part 820 Program model and related operations requirements.
- Programs must complete and receive approval of the required application documents to obtain OASAS certification as Title 14 NYCRR Part 820 and complete the application for designation to provide each of the three elements (stabilization; rehabilitation; or reintegration). Programs may seek designation to offer any or all of the elements. Designation will be based upon a program's assessment of its current and future patient needs and overall program vision for the services it is best positioned to deliver to the community. Programs converting from the prior models are required to submit the Part 820 conversion application7 and new programs must follow the certification process for new programs.
- During the demonstration time frame OASAS provided Part 820 residential programs with technical assistance sessions and developed a comprehensive set of technical assistance tools: readiness guidance documents, clinical manuals and fiscal modeling tools.9 For the remainder of the demonstration year OASAS will continue to work with the remaining providers to transition to the part 820 model.
- Quarter four (July 1, 2024, to Sept 30, 2024) concluded with a total of 156 Part 820 Programs. As such, at the conclusion of the three applicable quarters of the overall demonstration year, there has been a 5.4% increase in the total number of Part 820 Programs and a 4.7% increase in the total number of Part 820 beds statewide. For the remainder of the demonstration year, OASAS will continue to work with the remaining programs to transition to the Part 820 model.
- There are 47 remaining programs to convert from the previous residential or medically. monitored model.
Q2 1/1/2024 to 3/31/2024 Q3 4/1/2024 to 6/30/2024 Q4 7/1/2024 to 9/30/ 2024 Annual Service Total Number of Programs Total Number of Beds Total Number of Programs Total Number of Beds Total Number of Programs Total Number of Beds Total Number of Programs Total Number of Beds Stabilization 9 227 9 227 9 227 9 227 Rehabilitation 10 491 10 491 12 540 12 540 Reintegration 69 1,682 69 1,717 75 1,841 75 1,841 Stabilization and Rehabilitation 15 622 16 658 16 658 16 658 Rehab and Reintegration 14 459 16 492 14 474 14 474 Stabilization Rehab and Reintegration 31 1,890 30 1,882 30 1,882 30 1,882 Grand Total 148 5,371 150 5,467 156 5,622 156 5,622
Managed Care Coverage of Title 14 NYCRR Part 820 Residential Service Programs
- Under the NYS 1115 MRT waiver, Title 14 NYCRR Part 820 services and programs were incorporated into the MMC benefit package and became a required network provider type.
- The current model contract10 network requirements are:
- Urban counties: The network must include two providers per county.
Rural counties: The network must include two providers per region.- NYS monitors network adequacy of Part 820 as part of routine plan compliance reviews.
Level of Care Determination
NYS utilizes the LOCADTR11 tool to support level of care determination. The tool has been utilized over 2 million times by SUD providers and managed care utilization managers since 2014. The tool is a web-based decision algorithm that includes the full continuum of care and has a continuing care module to support continuing care decisions. OASAS supports the tool with asynchronistic training available and webinar trainings to support updates. Providers, MMC and commercial payers in NYS are required to use LOCADTR (unless otherwise approved by OASAS).
Effective August 27, 2013, prescribers are required to consult the Prescription Monitoring Program (PMP) Registry when writing prescriptions for Schedule II, III, and IV controlled substances, with limited exceptions. The PMP Registry provides practitioners with direct, secure access to view dispensed controlled substance prescription histories for their patients. The PMP is available 24 hours a day/7-days a week via an application on the Health Commerce System (HCS)12. Patient drug utilization reports include all controlled substances that were dispensed in NYS and reported by the pharmacy/dispenser for the past year. This information allows practitioners to better evaluate their patients' treatment with controlled substances and determine whether there may be misuse or non-medical use.
The Bureau of Narcotic Enforcement (BNE) continues to enhance and support clinicians in their usage of the NYS PMP registry with improved functionality and education, through combined support from NYSDOH and the CDC funded Overdose Data to Action - States Grant. The BNE works closely with NYS Information Technology Service (ITS) to build out the technical architecture to the PMP as needed for functionality. This includes the continuous monitoring of the NYS PMP registry for potential enhancements and weekly status meetings with NYS ITS. To enhance clinicians in their usage of the NYS PMP registry through education, BNE has reviewed the Opioid Prescriber Training for any language and technical deficiencies, which satisfies educational requirements in Public Health Law Article 33 §3309-a13 to raise healthcare provider awareness of the risks associated with prescribing and taking opioid pain medications. BNE will work with the contracted entity, State University of New York at Buffalo, to implement these necessary changes. When a healthcare provider takes the Opioid Prescriber Training course, there is a required pre and post-test. During the timeframe of 7/1/2024 through 9/30/2024, more than 4,700 healthcare providers took the Opioid Prescriber Training across nine different provider types. There was significant improvement in knowledge when comparing pre and post test scores, ranging from an increase of 20.74% to 29.49% for each category type. During the year (10/1/2023-9/30/2024), more than 30,000 healthcare providers took the Opioid Prescriber Training with an overall increase in knowledge of more than 20%. The training was taken by individuals in every county in NYS, as well as all 50 states.
BNE continues to enhance interstate data sharing. BNE has managed interstate PMP data sharing through the PMP Interconnect (PMPi) since 2015. In June 2021, BNE began interstate data sharing through the RxCheck hub. As of 7/1/2024, BNE has data sharing agreements with 36 states, as well as Puerto Rico, Washington DC, and Military Health Services through the PMPi and RxCheck hubs. During this time frame, BNE successfully connected the state of Vermont through a second hub. This allows for a PMP query to be routed through the secondary hub if the primary hub has a technological failure This is to mitigate the risk of disruption in interoperability searches. During the year (10/1/2023-9/30/2024), two states were connected to a secondary hub and one previously unconnected state was onboarded. BNE continues to work with the RxCheck Governance Board to aid in identification of state partners for interstate data sharing. In May 2022, BNE successfully integrated with the US Department of Veterans Affairs (VA). BNE continues to monitor the integration and collaborate with the VA, as needed.
In 2019, BNE directly integrated a pilot site's Electronic Health Records (EHR) system with the NYS PMP. Since then, BNE has expanded the number of users for this site from 13 to more than 6,500. The pilot site has continued to keep the Bureau apprised of successes and challenges. By assessing the challenges, BNE has determined two viable options for enhancing clinical workflow for prescribers and other state and federal stakeholders via EHR integration. The first option is integrating with the RxCheck hub. As of 9/30/2024, NYS ITS built the technical architecture to begin testing this option. The Division of Legal Affairs provides ongoing reviews of data use agreements pertaining to EHR integration. The second option for EHR integration is via the NYS Health Information Exchanges (HIEs). During the reporting period of July 2024 to September 2024, BNE in collaboration with the NYS Information Systems and Health Statistics Group (ISHSG), continued to work with two NYS HIEs to establish EHR integration. All connected facilities from one HIE have access to this functionality. The second HIE has seven facilities that have access and is currently expanding. BNE continues to work with the NYS ISHSG to onboard additional HIEs and increase the number of users querying the PMP via this method. By the close out of the year, BNE had achieved advancements in technical architecture and furthered collaborations with others states and interested parties to gain and expand knowledge on EHR integration.
VI. Evaluation of the Demonstration
On December 14, 2022, DOH submitted the 1115 evaluation design to CMS for review and approval. CMS returned the evaluation design with comments on April 18, 2023. DOH submitted a revised evaluation design to CMS on June 20, 2023, pending their review and approval. The evaluation design for the Managed Care Risk Mitigation COVID-19 PHE amendment was approved by CMS on January 10, 2023. The evaluation design for the Reasonable Opportunity Period (ROP) Extension COVID-19 PHE amendment was approved by CMS on October 25, 2023. On July 5, 2024, DOH submitted a revised 1115 evaluation design, that incorporated the NYHER and IMD waiver amendments, to CMS for review and approval.
VII. Consumer Issues
A. MMC Plan, HARP, and HIV SNP Reported Complaints
MCOs, including MMC plans, HARPs, and HIV SNPs, are required to report quarterly to the DOH on the number and type of enrollee complaints/action appeals that are received. MCOs are also required to report on the number and type of complaints that are received regarding enrollees who are in receipt of SSI.
The following table outlines the complaints MCOs reported by category for the most recent quarter and compared to the last four quarters:
MCO Product Line Total Complaints FFY 24 Q4
7/1/2024-9/30/2024FFY 24
10/1/2023-9/30/2024MMC 6,277 22,478 HARP 746 2,643 HIV SNP 76 328 Total MCO Complaints 7,099 25,449 As described in the table, MCOs reported 7,099 total enrollee complaints for the current quarter. This represents a 9.9% increase from the prior quarter's total of 6,462 enrollee complaints.
MCOs reported 6,277 MMC complaints this quarter, which is a 10.6% increase from the 5,677 of the previous quarter. The number of HARP complaints increased 3.9%, from 718 in the prior quarter to 746 this quarter. There were 76 HIV SNP complaints this quarter, which is an increase of 13.4% when compared to the 67 from the previous quarter.
The following table outlines the top five most frequent categories of complaints reported for MMCs, HARPs, and HIV SNPs, combined, for the most recent quarter and compared to the last four quarters:
Description of Complaint Percentage of Complaints FFY 24 Q4
7/1/2024-9/30/2024FFY 24
10/1/2023-9/30/2024Balance Billing 17% 15% Difficulty with Obtaining: Dental/Orthodontia 15% 12% Dissatisfied with Provider Services (Non-Medical) or MCO Services 13% 13% Reimbursement/Billing 6% 8% Dissatisfaction with Quality of Care 5% 5%
The following table outlines the top five most frequent categories of complaints reported for HARPs for the most recent quarter and compared to the last four quarters:
Description of Complaint Percentage of Complaints FFY 24 Q4
7/1/2024-9/30/2024FFY 24
10/1/2023-9/30/2024Dissatisfied with Provider Services (Non-Medical) or MCO Services 20% 21% Dissatisfaction with Quality of Care 8% 8% Difficulty with Obtaining: Dental/Orthodontia 7% 7% Difficulty with Obtaining: Personal Care 7% 5% Balance Billing 6% 5%
The following table outlines the top seven most frequent categories of complaints reported for HIV SNPs for the most recent quarter and compared to the last four quarters.
Please note: the bottom four categories are tied on both a percentage and true value level.
Description of Complaint Percentage of Complaints FFY 24 Q4
7/1/2024-9/30/2024FFY 24
10/1/2023-9/30/2024Dissatisfied with Provider Services (Non-Medical) or MCO Services 41% 27% Difficulty with Obtaining: Dental/Orthodontia 9% 12% Balance Billing 8% 5% Problems with Advertising/ Consumer Education/ Outreach/ Enrollment 5% 17% Dissatisfaction with Quality of Care 5% 8% Difficulty with Obtaining: Personal Care 5% 3% Difficulty with Obtaining: Eye Care 5% 2% The DOH notes a significant increase in the percentage of complaints reported in the Dissatisfied with Provider Services (Non-Medical) or MCO Services. While there is a smaller overall number of complaints reported within the HIV SNP line of business which can skew the percentage calculations, the number of complaints submitted for this category increased from the previous quarter. DOH will continue to monitor this to identify ongoing trends.
B. Monitoring of Plan Reported Complaints
The DOH has been monitoring the complaint activity for NYS Medicaid Section 1115 MRT Waiver. As part of this initiative, the DOH analyzes enrollee complaints by using an Observed to Expected (OE) ratio, to identify trends and potential problems across categories.
The OE ratios are calculated by DOH for each MCO to determine which categories, if any, had a higher-than-expected number of enrollee complaints over a six-month period. The OE ratio compares the number of enrollee complaints the MCO reported to the number that is expected, based on the relative size of the MCO's Medicaid population and its share of enrollee complaints for each category compared to other MCOs. For example, an OE ratio of 6.2 means that the number of enrollee complaints reported for a category was over six times more than what was expected. An OE ratio of 0.5 means that there were half as many enrollee complaints reported for a given category as what was expected.
Based on the OE ratio over a six-month period, DOH requests that MCOs review and analyze applicable categories in which the reported number of complaints was more than twice the expected amount. Where a persistent trend or an operational concern contributing to complaints is confirmed, the MCO is required to develop a CAP.
The DOH continues to monitor the progress of all corrective actions and requires additional intervention if the identified trend/issue persists.
Amida Care
FFY 24 Q2-FFY 24 Q3 (1/1/2024-6/30/2024)Complaint Category O/E Ratio Issue Identified Plan of Action Dissatisfaction with Quality of Care 9.7 The trend identified from the complaints received was that enrollees were dissatisfied with the medication, treatment, and overall care received at various hospitals and physicians' offices. There were no issues identified. The MCO will ensure that all reported issues are fully resolved. The MCO will also more closely monitor and strengthen communication with its skilled nursing facilities to ensure proper quality of care is being rendered. The DOH will continue to monitor progress in the next reporting period. Dissatisfaction with Provider Services (Non-Medical) or MCO Services 11.2 The trends identified from the complaints received were that enrollees were dissatisfied with the information and customer service provided by call center representatives at the MCO and its provider offices, and the MCO's incentive cards. The issues identified were that representatives did not provide adequate information and that the incentive cards were not delivered timely. The MCO will provide its call center representatives with continuous coaching and quality assurance monitoring. The MCO will also follow up with providers who enrollees report customer service issues about and coach them on communication skills. The MCO will hold weekly meetings to quickly resolve issues with mailing incentive cards. Difficulty with Obtaining: Dental/ Orthodontia 6.6 The trends identified from the complaints received were that enrollees were dissatisfied with the care and service given by their providers, the bills they received for services not performed or for uncovered services, lack of communication by their providers, missing paperwork for their procedures, and the difficulty to find available appointments with providers that were nearby. The issues identified were that some providers were making mistakes such as not submitting required forms and having poor communication with their enrollees. The MCO's vendor sends resolution letters with its determination and recommendations to its providers after a complaint is resolved. The MCO's vendor reminds its providers to review claim submissions diligently to reduce errors. The MCO's vendor provides coaching to its providers to correct their mistakes. The MCO's vendor reminds its providers of the importance of reviewing treatment plans with enrollees to reduce dissatisfaction. Difficulty with Obtaining: Mental Health or Substance Abuse Services/Treatment 161.8 The trends identified from the complaints received were that enrollees were dissatisfied with the quality of their mental health care, authorization errors, billing issues, the attitude and service of their providers, and issues finding in- network providers with available appointments. The issues identified were provider non- responsiveness and poor quality of care given by providers. The MCO will continue to issue corrective action when needed to providers who do not meet quality of care standards. The MCO will assist enrollees with finding providers when they report difficulty.
Capital District Physicians Health Plan
FFY 24 Q2-FFY 24 Q3 (1/1/2024-6/30/2024)Complaint Category O/E Ratio Issue Identified Plan of Action Dissatisfaction with Quality of Care 4.8 The trends identified from the complaints received were that enrollees were dissatisfied with the quality of care and service provided and that enrollees were experiencing difficulty accessing dental care. The issues identified were that enrollees were experiencing pain during their dental procedures and there were insufficient providers in the area. The MCO will review quality of care complaints by sharing feedback with providers, grading incidents based on severity, and review all quality-of-care complaints for any trends or multiple complaints regarding the same provider. Reimbursement/Billing 3.4 The trend identified from the complaints received was that enrollees were being billed for services. The issues identified were that enrollees were unknowingly being seen by and referred to out-of-network providers, enrollees were unaware that their eligibility was notactive at the time of service, and enrollees had coordination of benefit issues. The MCO will send a newsletter to their enrollees highlighting the importance of providing their accurate member information at the time of appointment scheduling and calling member services to confirm providers are in network prior to the appointment. The MCO will continue to monitor all billing complaint submissions and issue corrective action to providers exhibiting poor adherence to guidelines.
Healthfirst
FFY 24 Q2-FFY 24 Q3 (1/1/2024-6/30/2024)Complaint Category O/E Ratio Issue Identified Plan of Action Long Wait Time 3.1 The trend identified from the complaints received was that enrollees were dissatisfied with the length of time spent waiting in the office upon arriving to their dental appointments. The issue identified was that appointments were overbooked without adequate staffing. The MCO distributed reminders regarding Access and Availability standards to its provider network multiple times through email, fax, and updates to the provider manual. The MCO will complete its survey of all of its dental providers confirming whether they meet the one hour wait time limit and reaching out to those who do not. The MCO will continue to send monthly email reminders to call center representatives regarding the process of handling enrollee complaints about appointment availability, including long wait times. Dissatisfaction with Provider Services (Non-Medical) or MCO Services 2.0 The trend identified from the complaints received was that enrollees were experiencing issues related to delays in receiving authorized durable medical equipment (DME). The issue identified was that DME vendors were delayed in their deliveries to enrollees. The MCO established a monthly DME Oversight Committee to review key performance indicators, create member experience improvement initiatives, and escalate issues for resolution. The MCO is developing an enhancement to their provider portal requiring the correct information to be captured when authorizations are initially requested to speed up the process of delivering DME. The MCO's call center has been trained and will receive monthly reminders on the new DME process so they can properly advise providers. Difficulty with Obtaining: Eye Care 2.2 The trends identified from the complaints received were that enrollees were dissatisfied with their provider, or the service received, enrollees had billing and reimbursement concerns, enrollees were dissatisfied with benefit limitations, and enrollees were experiencing delays in obtaining glasses. The issues identified were that enrollees were not finding eyewear within the covered selection that fit their preferences, enrollees were not expecting 4-6 week wait times for the lab to produce their eyewear, and enrollees were not aware that they were receiving care from out- of-network providers. The MCO selected a new vision vendor and increased the vision network by over 80% to provide more options for its enrollees. The MCO introduced a new survey for enrollees to complete after each eye care visit so that the MCO can track and correct issues as they occur. Reimbursement/Billing 2.5 The trend identified from the complaints received was that enrollees were dissatisfied with being billed for services rendered. The issues identified were that enrollees were being billed for services when private pay agreements had been signed for non-covered services, out-of-network providers were billing enrollees directly after failing to verify eligibility or being dissatisfied with the reimbursement rates from the MCO, and enrollees were misinterpreting explanation of benefits as a bill. The MCO's vendor will continue to conduct education and outreach to all providers with existing complaints. The MCO's vendor will continue to send regular reminders to providers about acceptable and unacceptable scenarios for entering into private pay agreements. The MCO will send monthly emails to its call center staff and develop job aids to assist in educating the enrollees on their rights when entering into private pay agreements. Difficulty with Obtaining: Private Duty Nursing (PDN) 4.1 The trend identified from the complaints received was that enrollees were dissatisfied with their PDN agencies and aides. The issues identified were that due to staffing issues with in-network vendors, enrollees were seeing independent PDN's or making single case agreements with out-of- network vendors and experiencing a decrease in quality of care. The MCO is performing a network analysis on the PDN network and reevaluating its goals on network adequacy to reduce the amount of independent and out-of- network providers used and to reassign cases as more providers are added to the network. Difficulty with Obtaining: Personal Care 2.9 The trends identified from the complaints received were that enrollees were dissatisfied with the quality of service delivered by the aides, the lack of professionalism of the agency's coordinator, and language barriers. The issues identified were that enrollee expectations were not aligned with the care they were receiving. The MCO's DSE department will continue to meet monthly with providers to establish expectations for level of care and to identify the root causes that impact aide performance and professionalism. The MCO has targeted conversations to educate providers who have a grievance filed against them and ensure that the level of care meets the MCO's expectations. The MCO is developing a scorecard to track and trend poor performing agencies. Difficulty with Obtaining: CDPAS 2.6 The trend identified from the complaints received was that enrollees indicated that their aides were unpaid or not paid timely. The issue identified was delays in start dates and renewed authorizations due to missing paperwork even when the enrollee was reminded ahead of time. The MCO will continue to mail renewal paperwork and make reminder phone calls one month prior to their authorization expiration date. The MCO will continue to notify enrollees to obtain a doctor's order when denials are issued due to a missing doctor's order. The MCO's fiscal intermediary (FI) will continue to assist with outreaching enrollees when their authorization is close to expiring. The DOH will continue to monitor progress in the next reporting period. Dissatisfaction with BH Provider Services 2.6 The trend identified from the complaints received was that enrollees found that providers were unresponsive, inexperienced, and did not provide satisfactory service or make the enrollees feel safe. The issue identified was that providers were not meeting enrollee expectations. The MCO will issue corrective action plans to providers including sending email reminders to internal account managers emphasizing that providers are required to adhere to the roles and responsibilities outlined in the provider manual and sending communication to all account managers informing of their responsibility to convey this to their assigned providers during their regular meetings or calls.
Highmark
FFY 24 Q2-FFY 24 Q3 (1/1/2024-6/30/2024)Complaint Category O/E Ratio Issue Identified Plan of Action Appointment Availability: Specialist 20.2 The trend identified from the complaints received was that enrollees were having trouble finding in- network care within their desired distances with certain specialties, such as rheumatology, ENT, pain management, and cardiology. The issues identified were that enrollees were unfamiliar with available tools such as the MCO website's "Find a Doctor" feature, Sydney Health app, and contacting the MCO's Member Services. The MCO will continue to have its customer service representatives provide at least three (3) suitable providers and coach enrollees on how to find participating providers when enrollees report difficulty locating one. The MCO is upgrading its website and will create an electronic and paper instruction guide to assist enrollees in using the MCO's tools for locating in- network providers. The DOH will continue to monitor progress in the next reporting period. Dissatisfaction with Provider Services (Non-Medical) or MCO Services 2.2 The trends identified from the complaints received were that enrollees were experiencing poor interactions with their providers and administrative personnel, administrative delays in their care, communication issues, delays in technical support, and perceived rudeness from MCO associates. The issues identified were the MCO's phone system and web support help desk were causing issues for enrollees, and customer service representatives not meeting the needs of enrollees who need special assistance. The MCO identifies trends with wait time issues and perceived rudeness by issuing surveys to ensure needs are met, and educates its providers when issues are identified. The MCO holds regular meetings with staff who conduct home visits for enrollees who need assistance navigating their benefit and establishing connections with their PCPs. These staff can discuss barriers and issues and come up with new approaches tailored to the enrollees' specific needs. Difficulty with Obtaining: Specialist and Hospitals 3.0 The trends identified for the complaints received were that there were service delays and difficulties with obtaining authorizations, and that enrollees were experiencing difficulty with contacting their case managers. The issues identified were that authorization requests had missing information, authorizations for refills of DME supplies were requested before the permitted timeframe, calls were misrouted leading to delays in authorizations, and the MCO lacked a robust mechanism for tracking calls to and from its case managers. The MCO reaches out to provider groups when a pattern of authorization delays are observed to review the service authorization process, discuss submission methods, and clarify what information is needed for a timely turnaround. The MCO also conducts provider refresher trainings to reinforce the importance of screening and routing incoming calls. The MCO has implemented shared email for staff to submit contact requests for case managers and a way to track those requests. The MCO also performs regular random audits to ensure appropriate turnaround times and that the call records are accurately updated. Difficulty with Obtaining: Eye Care 7.6 The trends identified from the complaints received were that enrollees were experiencing difficulty locating in-network vision providers, were dissatisfied with their current vision providers, were dissatisfied with coverage limitations and replacements, and were experiencing difficulty with vision care authorizations. The issues identified were that enrollees were having difficulty navigating the MCO's online provider directory and were confused about the coverage in the benefit. The MCO will continue to assist enrollees in understanding their coverage and locating participating providers, and will keep its provider directory up to date. The MCO is also developing an educational document on the vision benefit which will be posted to its member website. Difficulty with Obtaining: Dental/ Orthodontia 2.4 The trends identified from the complaints received were that enrollees were experiencing difficulty finding available appointments or nearby providers, obtaining authorizations, accessing plan representatives by phone, understanding limitations of the benefit, understanding their bills, and receiving care up to their standards. The issues identified were that the MCO's provider directory was out of date, there were not enough practicing specialists in certain rural areas, call volumes and subsequent wait times were higher, and a lack of enrollee understanding of the changes to the benefit. The MCO will continue to address network gaps quarterly and assist enrollees who experience access issues. The MCO will continue to monitor call hold times and service levels and address any emerging performance issues. The MCO will train its contact center representatives with talking points on the Medicaid benefit, what is covered, and medical necessity requirements, so that they can provide point of contact education to its enrollees. Balance Billing 4.9 The trend identified from the complaints received was that enrollees were being billed by out-of- network providers and facilities for services rendered. The issues identified were that out-of- state providers were not complying with guidelines and were sending enrollees bills for claims. The MCO will continue to educate in-network providers on the laws surrounding balance billing, including via a fax blast newsletter scheduled for 10/31/2024. The MCO will continue to include language in its single case agreements informing of balance billing guidelines. DOH will continue to monitor progress in the next reporting period.
Health Insurance Plan of Greater New York
FFY 24 Q2-FFY 24 Q3 (1/1/2024-6/30/2024)Complaint Category O/E Ratio Issue Identified Plan of Action Difficulty with Obtaining: Dental/Orthodontia 9.9 The trends identified from the complaints received were that enrollees were dissatisfied with billing issues, customer service received from the MCO and its providers, inadequacy of the network and, quality of care issues. There were no issues identified. The MCO's vendor will reach out to practices which receive complaints and re-educate their staff. The MCO's vendor will more diligently review claims submissions to ensure accurate processing. Difficulty with Obtaining: Mental Health or Substance Abuse Services/Treatment 7.6 The trends identified from the complaints received were that enrollees were having difficulty accessing their care and experiencing communication issues and bad attitudes from administrative staff. The issues identified were regarding timeliness and adequacy of referrals, the MCO's provider directory, workforce challenges, and increased demand for services. The MCO will expand their provider availability verification activities and remind providers to attest to the accuracy of their data. The MCO has launched a digital survey platform for their provider directory audits. The MCO has piloted a mystery shopper program to test the accuracy of its provider directory. Reimbursement/Billing 5.6 The trend identified from the complaints received was that enrollees were dissatisfied that they received bills. The issues identified were that enrollees misinterpreted Explanations of Benefits (EOBs) as bills and enrollees were being balance billed by contracted and non- contracted providers. The MCO will educate enrollees on the differences between bills and EOBs and educate providers on not balance billing Medicaid enrollees. Difficulty with Obtaining: Home Health Care 8.6 The trend identified from the complaints received was that enrollees were dissatisfied with the number of hours they were approved for. The issue identified was that enrollees believe they need additional hours even after receiving an assessment. The MCO will continue to educate its enrollees regarding the clinical basis of their approved hours as well as the process for requesting a reassessment as their needs change. Difficulty with Obtaining: Personal Care 2.0 The trend identified from the complaints received was that enrollees were dissatisfied with the number of hours they were approved for. The issue identified was that enrollees believe they need additional hours even after receiving an assessment. The MCO will continue to educate its enrollees regarding the clinical basis of their approved hours as well as the process for requesting a reassessment as their needs change. Difficulty with Obtaining: CDPAS 6.0 The trend identified from the complaints received was that enrollees were dissatisfied with the number of hours they were approved for. The issue identified was that enrollees believe they need additional hours even after receiving an assessment. The MCO will continue to educate its enrollees regarding the clinical basis of their approved hours as well as the process for requesting a reassessment as their needs change.
Independent Health Association
FFY 24 Q2-FFY 24 Q3 (1/1/2024-6/30/2024)Complaint Category O/E Ratio Issue Identified Plan of Action Difficulty with Obtaining: Dental/ Orthodontia 2.6 The trends identified from the complaints received were that enrollees were dissatisfied with the quality of their dental care (especially dentures), experiencing difficulty locating in-network providers with available appointments, and experiencing coverage issues. The issues identified were that the changes in the criteria for services in the benefit led to an increase in overall enrollee utilization, enrollee expectations regarding service outcomes were due to poor communication between enrollees and providers, and enrollees did not understand what was covered. The MCO will create and send a provider education flyer to the network providing tips and resources on how to educate enrollees and set realistic expectations regarding the denture process. This will be re- sent to providers who receive any complaints regarding the quality of dentures they provided. The MCO will create a similar enrollee education piece to be sent with pre-estimates when dentures are being requested. The MCO will train its contact center on how the benefit works, what is covered, and the medical necessity requirements for these services.
MetroPlus Health Plan
FFY 24 Q2-FFY 24 Q3 (1/1/2024-6/30/2024)Complaint Category O/E Ratio Issue Identified Plan of Action Difficulty with Obtaining: Emergency Services 5.4 The trend identified from the complaints received was that enrollees were being balance billed for the emergency services they received. The issues identified were that providers did not submit claims to the MCO because they did not confirm the enrollees' coverage, enrollees did not present their insurance cards at the time of visit. In many cases, the providers rendering services were either out-of- state or disagreed with the MCO's reimbursement rates. The MCO will educate providers regarding proper billing by using targeted meetings, contractual education, trainings, and direct contact with the appropriate department. The MCO will educate enrollees during calls about their rights and responsibilities to protect against being balance billed, such as presenting insurance information at appointments and accessing information online or over the phone. Balance Billing 2.2 The trend identified from the complaints received was that enrollees were being balance billed for services they thought were covered. The issues identified were that one particular provider group altered its billing process, leading to errors and billing enrollees for covered services. The MCO will provide a monthly summary of complaints to its provider network team so they can identify and stop potential problems. The MCO will meet regularly with key providers to discuss claim concerns.
Molina Healthcare
FFY 24 Q2-FFY 24 Q3 (1/1/2024-6/30/2024)Complaint Category O/E Ratio Issue Identified Plan of Action Appointment Availability: PCP 6.0 The trends identified from the complaints received were that enrollees were having difficulty finding primary care physicians (PCPs) and that some physicians were not following the Access and Availability Standards. The issue identified was that enrollees were unaware of how to locate participating PCPs. The MCO will recommend that a tutorial on navigating its website be included in the member orientation. The MCO will reach out and educate providers that are not meeting the Access and Availability standards. The MCO will follow a quality improvement process including corrective action plans if necessary for providers who fail an internal survey. The MCO will closely monitor its network for any gaps through its PNDS system and will contract with additional providers when gaps are identified. The DOH will continue to monitor progress in the next reporting period. Difficulty with Obtaining: Specialist and Hospitals 8.1 The trend identified from the complaints received was that enrollees were having difficulty finding specialists and hospitals. The issue identified was enrollee difficulty with navigating the MCO website to search for specialist providers. The MCO will recommend that a tutorial on navigating its website be included in the member orientation. The MCO will closely monitor its network for any gaps and will contract with additional providers based on specialty when gaps are identified through its PNDS system. DOH will continue to monitor progress in the next reporting period. Difficulty with Obtaining: Eye Care 2.2 The trends identified from the complaints received were that enrollees were unable to locate vision providers in specific regions, and enrollees were dissatisfied with the service quality of the provider's office. The issue identified was that enrollees were unaware of providers available in their region and were provided a list once they contacted the MCO. The MCO will continue to have its customer service representatives address enrollee concerns. The MCO will continue to monitor provider adequacy and address any gaps. The MCO will outreach providers to address member concerns and will continue to ensure members are not dissatisfied. Pharmacy/Formulary 13.9 The trends identified from the complaints received were length in the review/approval process and limited medication availability and coverage for certain necessary treatments. The issues identified were the multiple steps of submitting prior authorization requests, providers were not submitting authorization requests timely, enrollees were unaware of the steps involved in the authorization process, and there were issues with medication availability of specific drugs at pharmacies. The MCO will educate its enrollee-facing staff on the authorization process by reviewing the current reference guide and editing to provide the steps required for submitting prior authorization requests. The MCO will collaborate with its provider relations team to implement enhanced provider education on submitting prior authorization requests. The MCO will develop and distribute clear enrollee materials explaining the authorization process and necessary steps. The DOH will continue to monitor progress in the next reporting period. Problems with Advertising/ Consumer Education/ Outreach/ Enrollment 11.5 The trend identified from the complaints received was that enrollees were not receiving materials. The issue identified was that enrollees had incorrect demographic information on file which was contributed to the enrollee not receiving the requested information. The MCO will call enrollees to verify demographic information once there is confirmation of undeliverable mail. The DOH will continue to monitor progress in the next reporting period. All Other 14.2 The trend identified from the complaints received was that enrollees were dissatisfied with prior authorization requirements. The issue identified was that enrollees and providers did not understand the authorization process. The MCO will use its website to educate its providers on the authorization process. The MCO will share a report of complaint types with leadership to identify opportunities to educate enrollees. DOH will continue to monitor progress in the next reporting period. Balance Billing 8.3 The trend identified from the complaints received was that providers were billing enrollees for services received. The issues identified were that enrollees failed to present insurance ID cards. The MCO will contact providers who balance bill and remind them that this is not allowed. The MCO will educate enrollees at enrollment and when they are balance billed to remind them to provide their insurance information. DOH will continue to monitor progress in the next reporting period. Difficulty with Obtaining: Home Health Care 5.1 The trend identified from the complaints received was that enrollees were dissatisfied with a delay in service authorizations. The issue identified was a lack of employee adherence to the MCO's workflow. The MCO reeducated its employees on its process and their responsibilities. The MCO will follow a process to ensure NYIAP cases are pulled twice a day and processed within 24 hours. Authorizations will be loaded to appropriate software and care managers will contact members for welcome calls. DOH will continue to monitor progress in the next reporting period.
MVP Health Plan
FFY 24 Q2-FFY 24 Q3 (1/1/2024-6/30/2024)Complaint Category O/E Ratio Issue Identified Plan of Action Difficulty with Obtaining: Dental/ Orthodontia 2.6 The trends identified from the complaints received were that enrollees were receiving bills for non- covered services received, having difficulty getting appointments, dissatisfied with the quality of their care, dissatisfied with their providers and their staff, experiencing long wait times, dissatisfied with the plan benefits, and unable to find in-network providers nearby. The issues identified were that enrollees did not understand their dental benefit including access to participating providers, providers were not receiving appropriate education and support, and the MCO's vendor's customer service staff were not receiving appropriate education and support. The MCO's dental vendor will continue to coach its customer service staff and monitor for quality concerns. The MCO's vendor will reach out to individual providers and reeducate their staff as necessary, including access to educational materials available to them. The MCO will send out a monthly newsletter to providers with reminders on quality expectations.
United Healthcare
FFY 24 Q2-FFY 24 Q3 (1/1/2024-6/30/2024)Complaint Category O/E Ratio Issue Identified Plan of Action Appointment Availability: Specialist 2.5 The trend identified from the complaints received was that enrollees could not find in-network providers (dermatology, dental, endodontic, periodontic, physical therapy, endocrinology, pain management, cardiac rehab, and cancer treatment). The issue identified was that provider network changes caused providers to remove themselves or be discontinued from the network. The MCO will educate enrollees on network changes and assist them with finding a participating provider to best suit their needs. The MCO also will assist enrollees with locating out-of- network care if in-network providers are not available or do not have the needed experience to care for the enrollee. Dissatisfaction with Quality of Care 2.6 The trend identified from the complaints received was that enrollees were dissatisfied with their care. This is related to a variety of care related topics. Concerns related to accessing in-network providers is also noted. The MCO will issue corrective actions to providers who have been found with a substantiated quality of care concern. This will involve providing educational materials, requesting formal continued medical education, reporting to state boards, and restriction, suspending, or terminating network participation, if necessary. Denial of Clinical Treatment 10.6 The trend identified from the complaints received was that enrollees were receiving denials for services. The issue identified was that enrollees requested services that are excluded from the plan. The MCO will continue to monitor denials. Otherwise, minimal proactive measures cannot be taken for these types of complaints other than additional services becoming covered under the plan. Communications/ Physical Barrier 8.1 There were no trends identified from the complaints received. The majority of complaints in this category were miscategorized by the MCO, causing its reported numbers in this category to be higher than expected. The MCO will retrain staff on proper complaint categorization. Problems with Advertising/ Consumer Education/ Outreach/ Enrollment 2.6 The trends identified from the complaints received were that enrollees received materials in the incorrect language, received materials meant for another enrollee, received paper correspondence after requesting paperless correspondence, did not receive the member handbook, and were dissatisfied with the member ID cards. The majority of complaints in this category were miscategorized by the MCO, causing its reported numbers in this category to be higher than expected. The MCO will remediate to resolve discrepancies between coding and reporting complaints moving forward. Balance Billing 3.6 The trend identified from the complaints received were that enrollees were being balance billed. The issue identified was that non-participating providers were not accepting the Medicaid rates of payment and were billing enrollees for the balance. The MCO will continue to discuss ways to prevent surprise bills. The DOH will continue to monitor progress in the next reporting period.
VNS Choice
FFY 24 Q2-FFY 24 Q3 (1/1/2024-6/30/2024)Complaint Category O/E Ratio Issue Identified Plan of Action Problems with Advertising/ Consumer Education/ Outreach/ Enrollment 66.6 The trends identified from the complaints received were that enrollees were dissatisfied with delays in receiving and non-receipt of the VISA reward cards, the amount issued on the reward card, the choice of available merchants that enrollees can use with the reward card, receiving mail in the wrong language and dissatisfaction with the plan's member ID cards. The issues identified were that there was a supply chain issue with the plan's reward card vendor, as well as one complaint in which the member was not eligible to receive the card due to health activities not being completed. The MCO continues to address complaints received from members regarding the merchant list and will add/expand the VISA reward card benefit as long as required guidelines are met. The MCO also works with the VISA card vendor to help mitigate potential delays. All Other 8.3 The trends identified from the complaints received were dissatisfaction with providers for reasons such as discrimination, accusations, and lack of prescription submission for DME, dissatisfaction with the assigned care manager, communication issues with the MCO, and timesheet/communication from LHCSAs. The issues regarding provider complaints were unsubstantiated due to the providers not being identified, and complaints regarding care management and LHCSAs were miscategorized by the MCO, causing its reported numbers in this category to be higher than expected. The MCO educated enrollees and level set expectations. The MCO educated its staff regarding appropriate categorizing of complaints. C. Long Term Services and Supports (LTSS)
As SSI recipients typically access LTSS, DOH monitors complaints and action appeals filed with MCOs by SSI recipients. Of the 7,099 total reported complaints/action appeals, MCOs reported 676 complaints and action appeals from their SSI recipients. This compares to 571 SSI complaints/action appeals from the previous quarter, representing an 18.4% increase.
The following table outlines the total number of complaints/action appeals MCOs reported for SSI recipients by category for the most recent quarter and compared to the last four quarters:
Description of Complaint Number of Complaints/Action Appeals Reported for SSI Recipients FFY 24 Q4
7/1/2024-9/30/2024FFY 24
10/1/2023-9/30/2024Appointment Availability: PCP 2 5 Appointment Availability: Specialist 7 19 Appointment Availability: BH HCBS 1 5 Long Wait Time 4 13 Dissatisfaction with Quality of Care 34 140 Denial of Clinical Treatment 17 55 Denial of BH Clinical Treatment 1 3 Dissatisfied with Provider Services (Non- Medical) or MCO Services 171 570 Dissatisfaction with BH Provider Services 6 21 Dissatisfaction with Health Home Care Management 9 27 Difficulty with Obtaining: Specialist and Hospitals 45 138 Difficulty with Obtaining: Eye Care 7 17 Difficulty with Obtaining: Dental/Orthodontia* 49 145 Difficulty with Obtaining: Emergency Services 1 2 Difficulty with Obtaining: Mental Health or Substance Abuse Services/Treatment 0 3 Difficulty with Obtaining: RHCF Services 4 4 Difficulty with Obtaining: Adult Day Care 0 0 Difficulty with Obtaining: Private Duty Nursing 13 49 Difficulty with Obtaining: Home Health Care 12 36 Difficulty with Obtaining: Personal Care 71 224 Difficulty with Obtaining: PERS 1 2 Difficulty with Obtaining: CDPAS 17 73 Difficulty with Obtaining: AIDS Adult Day Health Care 0 0 Pharmacy/Formulary 4 17 Access to Non-Covered Services 9 25 Access for Family Planning Services 0 1 Communications/ Physical Barrier 3 8 Problems with Advertising/ Consumer Education/ Outreach/ Enrollment 13 33 Recipient Restriction Program and Plan Initiated Disenrollment 0 1 Reimbursement/Billing 47 206 Balance Billing 57 175 Transportation 1 10 All Other 70 218 Total 676 2,245
The following table outlines the top five most frequent categories of SSI recipient complaints/action appeals MCOs reported for the most recent quarter and compared to the last four quarters:
Description of Complaint Percentage of Total Complaints/Appeals Reported for SSI Recipients FFY 24 Q4
7/1/2024-9/30/2024FFY 24
10/1/2023-9/30/2024Dissatisfied with Provider Services (Non- Medical) or MCO Services 25% 25% Difficulty with Obtaining: Personal Care 11% 10% Balance Billing 8% 8% Difficulty with Obtaining: Dental/Orthodontia 7% 6% Reimbursement/Billing 7% 9%
The DOH requires MCOs to report the number of enrollees in receipt of LTSS as of the last day of the quarter. During the current reporting period of July 1, 2024, through September 30, 2024, MCOs reported LTSS enrollment of 62,310 enrollees. This compares to 60,223 LTSS enrollees from the previous quarter, representing a 3.5% increase. The following table outlines the number of LTSS enrollees by MCO for each of the last four quarters:
Plan Number of LTSS Enrollees FFY 24 Q4
7/1/2024-9/30/2024FFY 24 Q3
4/1/2024-6/30/2024FFY 24 Q2
1/1/2024-3/31/2024FFY 24 Q1
10/1/2023-12/31/2023Amida Care 1,043 1,260 1,265 1,261 Anthem 4,210 3,601 3,684 3,608 Capital District Physicians Health Plan 680 655 346 770 Excellus Health Plan 1,800 1,800 1,800 1,821 Fidelis Care 21,297 21,154 20,680 20,875 Healthfirst 17,994 16,604 15,718 15,278 Highmark 333 322 315 297 HIP of Greater New York 652 617 431 445 Independent Health Association 751 743 769 757 MetroPlus Health Plan 4,350 4,045 3,646 3,544 Molina Healthcare 3,235 3,311 3,107 3,050 MVP Health Plan 1,911 2,260 2,586 2,505 United Healthcare 3,485 3,425 3,414 3,408 VNS Choice 569 426 446 432 Total 62,310 60,223 58,207 58,051
The following table outlines the total number of complaints/action appeals received from all enrollees, regardless of product line, regarding difficulty with obtaining LTSS that MCOs reported for each of the last four quarters:
Description of Complaint Number of Complaints/Action Appeals Reported FFY 24 Q4
7/1/2024-9/30/2024FFY 24 Q3
4/1/2024-6/30/2024FFY 24 Q2
1/1/2024-3/31/2024FFY 24 Q1
10/1/2023-12/31/2023Difficulty with Obtaining: AIDS Adult Day Health Care 0 0 1 0 Difficulty with Obtaining: Adult Day Care 2 0 0 0 Difficulty with Obtaining: CDPAS 46 64 58 69 Difficulty with Obtaining: Home Health Care 58 43 26 55 Difficulty with Obtaining: RHCF Services 13 6 4 0 Difficulty with Obtaining: Personal Care 213 178 129 149 Difficulty with Obtaining: PERS 3 5 2 1 Difficulty with Obtaining: Private Duty Nursing 14 12 20 19 Total 349 308 240 293 D. Critical Incidents:
The DOH requires MCOs to report critical incidents involving enrollees in receipt of LTSS. There were 315 critical incidents reported for the July 1, 2024, through September 30, 2024, period, most of which have a resolved status. Many of the incidents stemmed from falls. The DOH continues to work with MCOs to maintain accuracy in reporting of their LTSS critical incident numbers.
The following table outlines the total number of LTSS critical incidents reported by MMCs, HARPs, and HIV SNPs for each of the last two quarters, the net change over the last two quarters, and the total for the last four quarters:
Plan Name Critical Incidents FFY 24 Q4
7/1/2024-9/30/2024FFY 24 Q3
4/1/2024-6/30/2024Net Change FFY 24
10/1/2023-9/30/2024Medicaid Managed Care Plans Anthem 1 4 −3 9 Capital District Physicians Health Plan 0 0 0 0 Excellus Health Plan 3 7 −4 38 Fidelis Care 93 66 +27 161 Healthfirst 80 74 +6 264 HIP of Greater New York 0 0 0 0 Highmark 0 0 0 0 Independent Health Association 0 0 0 0 MetroPlus Health Plan 2 0 +2 2 Molina Healthcare 0 0 0 0 MVP Health Plan 0 1 −1 1 United Healthcare 0 0 0 0 Total 179 152 +27 475 Health and Recovery Plans Anthem 0 0 0 1 Capital District Physicians Health Plan 0 0 0 0 Excellus Health Plan 1 1 0 6 Fidelis Care 48 51 −3 99 Healthfirst 63 63 0 180 HIP of Greater New York 0 0 0 0 Independent Health Association 0 0 0 0 MetroPlus Health Plan 0 0 0 0 Molina Healthcare 0 0 0 0 MVP Health Plan 0 0 0 0 United Healthcare 0 0 0 0 VNS Choice 0 0 0 0 Total 112 115 −3 286 HIV Special Needs Plans Amida Care 0 0 0 0 MetroPlus Health Plan 0 0 0 0 VNS Choice 24 3 +21 31 Total 4 3 +21 31 Grand Total 315 270 +45 792
The following table outlines the total number of critical incidents MCOs reported for enrollees in receipt of LTSS by category for each of the last two quarters, the net change over the last two quarters, and the total for the last four quarters:
Plan Name Critical Incidents FFY 24 Q4
7/1/2024-9/30/2024FFY 24 Q3
4/1/2024-6/30/2024Net Change FFY 24
10/1/2023-9/30/2024Medicaid Managed Care Plans Any Other Incidents as Determined by the Plan 11 14 −3 36 Crimes Committed Against Enrollee 2 3 −1 14 Crimes Committed by Enrollee 2 4 −2 10 Instances of Abuse of Enrollees 7 8 −1 19 Instances of Exploitation of Enrollees 0 0 0 2 Instances of Neglect of Enrollees 2 8 −6 14 Medication Errors that Resulted in Injury 0 1 −1 2 Other Incident Resulting in Hospitalization 52 42 +10 117 Other Incident Resulting in Medical Treatment Other Than Hospitalization 89 67 +22 242 Use of Restraints 14 5 +9 19 Wrongful Death 0 0 0 0 Total 179 152 +27 475 Health and Recovery Plans Any Other Incidents as Determined by the Plan 13 16 −3 32 Crimes Committed Against Enrollee 3 12 −9 18 Crimes Committed by Enrollee 4 1 +3 5 Instances of Abuse of Enrollees 5 3 +2 11 Instances of Exploitation of Enrollees 0 0 0 0 Instances of Neglect of Enrollees 0 3 −3 3 Medication Errors that Resulted in Injury 0 0 0 1 Other Incident Resulting in Hospitalization 27 14 +13 46 Other Incident Resulting in Medical Treatment Other Than Hospitalization 56 56 0 154 Use of Restraints 4 10 −6 15 Wrongful Death 0 0 0 1 Total 112 115 −3 286 HIV Special Needs Plans Any Other Incidents as Determined by the Plan 0 0 0 0 Crimes Committed Against Enrollee 1 0 +1 1 Crimes Committed by Enrollee 0 0 0 0 Instances of Abuse of Enrollees 0 0 0 0 Instances of Exploitation of Enrollees 1 0 +1 1 Instances of Neglect of Enrollees 7 2 +5 9 Medication Errors that Resulted in Injury 0 0 0 0 Other Incident Resulting in Hospitalization 1 0 +1 1 Other Incident Resulting in Medical Treatment Other Than Hospitalization 14 1 +13 19 Use of Restraints 0 0 0 0 Wrongful Death 0 0 0 0 Total 24 3 +21 31 Grand Total 315 270 +45 792 The DOH notes an increase in critical incidences reported under the description of "Other Incident Resulting in Medical Treatment Other Than Hospitalization" from quarter three to quarter four. This is the result of clarifications made in communications to the MCOs pertaining to the types of critical incidents that are to be included in this report.
E. Enrollee Complaints Received Directly by the DOH
In addition to the MCO reported complaints, the DOH directly received 79 enrollee complaints this quarter. This total is a 1.3% decrease from the previous quarter, which reported 80 enrollee complaints.
Annually, the DOH directly received 365 MCO member complaints regarding MMCs, HARPs, and HIV SNPs. The following table represents previously reported complaints filed directly with DOH, including complaints from enrollees and their representatives.
MCO Enrollee Complaints Received Directly by DOH FFY 24 Q4
7/1/2024-9/30/2024FFY 24 Q3
4/1/2024-6/30/2024FFY 24 Q2
1/1/2024-3/31/2024FFY 24 Q1
10/1/2023-12/31/2023Total FFY 23
10/1/2023-9/30/202479 80 99 107 365 The following table outlines the top six most frequent categories of enrollee complaints/action appeals received directly by the DOH involving MCOs for the most recent quarter and compared to the last four quarters:
Percentage of MCO Enrollee Complaints Received Directly by DOH Description of Complaint FFY 24 Q4
7/1/2024-9/30/2024FFY 24 Q3
4/1/2024-6/30/2024FFY 24 Q2
1/1/2024-3/31/2024FFY 24 Q1
10/1/2023-12/31/2023Problems with Advertising/ Consumer Education/ Outreach/ Enrollment 13% 8% 14% 8% Difficulty with Obtaining: Home Health Care 11% 26% 18% 11% Reimbursement/Billing 10% 5% 7% 10% Difficulty with Obtaining: Dental/Orthodontia 9% 10% 9% 8% Difficulty with Obtaining: CDPAS 9% 6% 3% 6% Difficulty with Obtaining: Specialist and Hospitals 9% 4% 3% 4% DOH monitors and tracks enrollee complaints reported to the DOH related to new or changed benefits and populations enrolled into MCOs.
As per the NYS of Health Marketplace: "Under the Families First Coronavirus Response Act's continuous coverage requirement, NYS Medicaid, CHPlus and Essential Plan (EP) members have not had to renew their health insurance since early 2020. The Consolidated Appropriations Act of 2023 requires states to begin the process of redetermining enrollees in April 2023. This process is also referred to as the ‘unwind.' NYS began sending renewal notices in the early spring to enrollees in Medicaid, CHPlus, and EP with June 30, 2023, coverage end dates. This process will continue each month until every renewal cycle of enrollees, referred to as a cohort, has had their eligibility redetermined."
Please note: the PHE Unwind was completed in May 2024.
F. Fair Hearings
There were 176 fair hearings involving MMCs, HARPs, and HIV SNPs during the period of July 1, 2024, through September 30, 2024. The dispositions of these fair hearings for each of the last four quarters are as follows:
Fair Hearing Decisions (includes MMC, HARP and HIV SNP) Hearing Dispositions FFY 24 Q4
7/1/2024-9/30/2024FFY 24 Q3
4/1/2024-6/30/2024FFY 24 Q2
1/1/2024-3/31/2024FFY 24 Q1
10/1/2023-12/31/2023In favor of Appellant 60 74 93 118 In favor of Plan 98 105 104 99 No Issue 18 9 15 14 Total 176 188 212 231 For fair hearing dispositions occurring for each of the last four quarters, the following table describes the number of days from the initial request for a fair hearing to the final disposition of the hearing, including time elapsed due to adjournments.
Fair Hearing Days from Request Date till Decision Date (includes MMC, HARP and HIV SNP) Decision Days FFY 24 Q4
7/1/2024-9/30/2024FFY 24 Q3
4/1/2024-6/30/2024FFY 24 Q2
1/1/2024-3/31/2024FFY 24 Q1
10/1/2023-12/31/20230-29 1 0 2 0 30-59 21 28 32 8 60-89 27 42 45 23 90-119 26 25 27 41 =>120 101 93 106 159 Total 176 188 212 231
G. Medicaid Managed Care Advisory Review Panel (MMCARP) Meetings
The MMCARP met on September 19, 2024. The meeting included presentations provided by state staff and discussions of the following: updates on the status of the MMC program, current auto-assignment statistics and state and local district outreach and other activities aimed at reducing auto-assignment, and an update on the status of the MLTC program. There were two additional agenda items, a SCN Implementation Update given by Selena Hajiani and Emily Engel, and a PHE Unwind Status Update given by Sonia Sekhar and Gabrielle Armenia. A public comment period is offered at every meeting. The next MMCARP meeting is scheduled for December 12, 2024.
Annual: The MMCARP is required to meet quarterly. Meetings were held on December 21, 2023, March 21, 2024, June 20, 2024, and September 19, 2024.
VIII. Quality Assurance/Monitoring
A. Quality Measurement in Managed Long-Term Care
In October 2023, the 2022 MLTC Consumer Guides were released on the DOH website14 and Health Data NY15. DOH staff also worked with New York Medicaid Choice, our facilitated Medicaid enroller, to ensure printable versions were included in new members' enrollment packets.
In December 2023, the DOH publicly released the 2022 MLTC Report16. Later that month, the 2024 MLTC Quality Incentive Methodology document was released to MLTC plans.
During the January through March 2024 reporting period, preparations began for calculating MLTC quality, satisfaction, and compliance measures. Activities included: attributing MLTC members to accountable health plans based on annual assessment data, securing all data sources necessary for the calculation of the 2023 MLTC Quality Incentive, and updating the programs used to calculate measures to ensure agreement with the publicly released methodology. Additionally, the NYSDOH and our EQRO, IPRO, hosted a kick-off meeting on January 16, 2024, with MLTC plans to launch the 2024-25 PIP topic, "Decreasing Rates of Depression among Medicaid MLTC Members". Health plan representatives were provided with topic background and briefed on expectations, measure specifications, timelines, and deliverables.
During the April through June 2024 reporting period, staff activities were focused on calculating MLTC quality, satisfaction, efficiency, and compliance measures. Activities included: testing over time quality and potentially avoidable hospitalizations measures that had not been calculated since before the COVID pandemic when assessments were performed every six months, running satisfaction measures, and sharing output with health plans for review and feedback. Additionally, DOH staff work closely with IPRO on finalizing the 2023 MLTC Satisfaction Survey Report which was published on the DOH's public website17.
The Crude Percent Reports for the January through December 2022 reporting period were released in September to MLTC plans. These reports are plan-specific and reflect each plan's cohort of UAS-NY CHA assessments, and utilize the latest, finalized patient assessment during this twelve-month period. The Crude Percent Report provides a breakout by percentage (unless a metric is reported as an average) of each response level for most components of the Community Assessment, Functional Supplement, and Mental Health Supplement the twelve- month period. Plans also received rest of the state percentages with their plan excluded for comparison purposes. Plans were encouraged to review the reports, compare their results to previous data, and look at areas with changes from the previous reporting period to ensure data completeness. The January - December 2023 MLTC measure results were added to Health Data NY18. In addition to accessing MLTC quality data dating back to 2014, users may also download the data dictionary and measure definitions to fully explore MLTC health plan performance. Finally, the DOH in collaboration with IPRO, hosted two webinars for MLTC plans to present an overview of their PIP projects including implemented interventions, preliminary measures results, and discuss barriers encountered. Also, during the July through September 2024 reporting period, significant progress was made on several high-value MLTC deliverables including the 2023 MLTC Consumer Guides, the 2023 MLTC Report, and the 2023 Quality Initiative. These products were in the final editing stages with release dates anticipated in late fall 2024.
B. Quality Measurement in Medicaid Managed Care
Quality Measure Benchmarks 2022 (Measurement Year 2022)
Quality of care remained high for MMC members for the Demonstration Year. In measurement year 2022, national benchmarks were available for 64 measures for Medicaid. Out of the 64 measures that NYS Medicaid plans reported, 75% of measures met or exceeded national benchmarks. NYS consistently met or exceeded national benchmarks across measures, especially in MMC. The NYS Medicaid rates exceed the national benchmarks for BH on adult measures (e.g., receiving follow-up within seven and 30 days after an emergency department visit for mental illness), and child measures (e.g., metabolic monitoring for children and adolescents on antipsychotics, the initiation/continuation of follow-care for children prescribed ADHD medication, and the use of first-line psychosocial care for children and adolescents on antipsychotics). NYS managed care plans also continue to surpass national benchmarks in several women's preventive care measures (e.g., postnatal care, as well as screening for Chlamydia, and cervical cancer), and children and adolescent preventative measures (Well- child visits during first 30 months of life, well-care visits among children aged 3-21 years old, and immunization). Considering this was during a period of COVID-19 impacts in NYS, the data demonstrates that many aspects of quality of care remained high for New Yorkers on Medicaid.2023 Satisfaction Survey
In the fall of 2023, the DOH conducted a satisfaction survey of adults enrolled in MMC, HARP, and SNP plans. The Consumer Assessment of Healthcare Providers and Systems (CAHPS®)
5.1H Adult Medicaid survey was administered. The administration methodology consisted of a five-wave mixed-mode (mailing and web) protocol, with postcard reminder after the first two questionnaire packets. The survey included 12 MMC plans in New York with a sample of 2,000 members per plan. Questionnaires were sent to 24,000 adult members following a combined mail and web methodology during the period October 30, 2023, through January 22, 2024, using a standardized survey procedure and questionnaire. A total of 2,735 eligible and complete responses were received resulting in a 13.2% response rate.Response options for overall rating questions ranged from 0 (worst) to 10 (best). In the table below, the achievement score represents the proportion of members who responded with a rating of "8", "9", or "10". These results are presented as Medicaid overall, New York City, and Rest of State.
2022 Quality Incentive for Medicaid Managed Care
The 2022 Quality Incentive Awards calculations were finalized in May 2024 which covered the measurement year period for 2022. The quality incentive is calculated on the percentage of total points a plan earned in the areas of Quality of Care and Experience of Care. Points are subtracted from the plan's total points if the plan had SODs in the Compliance category. Plans were classified into five tiers based on the distribution of the final percentage points. The amount of the incentive award is determined by the Division of Finance and Rate Setting and subject to final approval from Division of Budget and CMS. The results for the 2022 Incentive included two plans in Tier 1, one plan in Tier 2, six plans in Tier 3, one plan in Tier 4, and two plans in Tier 5.Quality Assurance Reporting Requirements (QARR)
In June, 26 health plans submitted reporting requirements to stakeholders as identified in QARR (e.g., NYS, IPRO, National Committee on Quality Assurance). Data was being collated and reviewed through the subsequent months. 2022 Data was published in November 2023.C. Quality Improvement External Quality Review
IPRO continues to provide EQR services related to required, optional, and supplemental activities, as described by CMS in 42 CFR, part 438, Subparts D and E, expounded upon in NYS's consolidated contract with IPRO. Ongoing activities include: 1) validation of performance improvement projects (PIPs); 2) validation of performance measures; 3) review of MCO compliance with state and federal standards for access to care, structure and operations, and quality measurement and improvement; 4) validating encounter and functional assessment data reported by the MCOs; 5) overseeing collection of provider network data; 6) administering and validating consumer satisfaction surveys; 7) conducting focused clinical studies; and 8) developing reports on MCO technical performance. In addition to these specified activities, NYSDOH requires our EQRO to also conduct activities administering additional surveys of enrollee experience; and providing data processing and analytical support to the DOH. EQR activities cover services offered by New York's MMC plans, HIV-SNPs, MLTC plans, and HARPs, and include the State's CHPlus. Some projects may also include the Medicaid FFS population, or, on occasion, the commercial managed care population for comparison purposes.
Annual EQRO Technical Reports
IPRO continues to work on the EQR Technical Reports for New York's Medicaid and CHPlus plans. In the first and second quarters, IPRO worked on the Measurement Year 2022 reports (which were for the 2023-2024 reporting cycle). In April, IPRO completed the reports, and NYSDOH submitted the reports to CMS and posted them on the NYSDOH website by the April 30 due date. In June, NYSDOH and IPRO started the process for the Measurement Year 2023 Technical Reports (to be submitted for the 2024-2025 reporting cycle). In the fourth quarter, IPRO continued to work on the 2023 reports. NYSDOH and IPRO are projecting to have first final drafts by the end of quarter one 2024.Provider Related and Access Activities
IPRO continues to work on surveys related to access and network adequacy. During the first and second quarters, IPRO worked on and completed the following surveys: Access and Availability, Provider Directory, PCP, and Member Services. In the third quarter, the results were issued to the plans. In the fourth quarter, NYSDOH and IPRO started discussions and work on the next cycle of surveys.Provider Network Data System (PNDS):
PNDS
IPRO continues to oversee two sub-contracts, RMCI and Quest Analytics, for the management of the rebuild of the PNDS. The PNDS collects network information from approximately 400 active networks in NYS. IPRO and their subcontractors, RMCI and Quest Analytics, facilitated ongoing adjustments and fixes and addressed any continuing issues with the rebuild of the PNDS network, relative to use, expansion, and maintenance. The July-September 2024 PNDS submission deadline was October 24, 2024; plans submitted data based on version 12 of the data dictionary.Provider and Health Plan LOOK-UP:
The NYS Provider & Health Plan Look-Up website helps consumers in their health plan network and provider search. IPRO continues to refresh the data twice a month. The site has close to two million distinct users since its launch in May 2017.PANEL:
Panel data submission opened for Q3 2024 data collection on August 1 and yielded 6,612,389 rows of data which is ~1% less than the previous quarter. Technical assistance was provided by NYSDOH and IPRO throughout the submission, particularly around new edits implemented.NYSDOH provided detailed analytics to plans about failing newly updated requirements.
Managed Long-Term Care:
Performance Improvement Projects (PIPs)
The 2022-2023 Social Determinants of Health (SDoH) PIP final reports were finalized by IPRO and approved by NYSDOH in the second quarter. For the fourth quarter, the summary reports for the 2022-2023 Social Determinants of Health PIP were in production.The 2024-2025 Depression Screening PIP Template and background document were sent out to the plans at the end of the first quarter. In June, all the 2024-2025 Depression Screening PIP Proposals were submitted, and the initial reviews were conducted. By September, IPRO approved all of the 2024-2025 Proposals and hosted two webinars. IPRO completed progress calls for groups of the MLTC plans in September 2024.
MLTC Member Satisfaction Survey
IPRO conducted a member satisfaction survey for MLTC, wrote a report on the findings, and in August, distributed the results to the plans.Focused Clinical Study: Focused Clinical Study of Reliability of the Telehealth Mode for Uniform Assessment System for New York (UAS-NY) Community Health Assessment (CHA) in the Managed Long-Term Care Population.
IPRO conducted a focused clinical study for MLTC plans, and the final report was approved by NYSDOH in August.Quality Measurement
IPRO continues their work on Quality Assurance Reporting Requirements (QARR).
- For Measurement Year 2023, IPRO validated all patient level detail, birth files, and enhancement files and submitted them to NYSDOH by mid-August.
- For Measurement Year 2024, Plans were notified of measure changes and updates in the first and second quarters.
- For the Adult CAHPS survey, IPRO worked with DataStat to draft the survey, letters, and postcards in different languages. The survey was initiated in November 2023, and it was published on the NYSDOH website by June 2024.
PIPs for MMCs:
2022-2023 MMC and HIV SNP PIP: Improving Rates of Preventive Dental Care for MMC and HIV SNP Adult MembersThe 2022-2023 MMC and HIV SNP PIP was completed in December 2023, and in the first quarter, all Plans presented on lessons learned and next steps planned to sustain and spread successful interventions to other populations and processes. In July 2024, all MCOs submitted their final reports. IPRO reviewed the reports, provided feedback, and all final reports were in the process of being finalized in September 2024.
2024-2025 MMC, CHP and HIV SNP PIP: Improving Rates of Cancer Screening and Prevention for MMMC, CHP, and HIV SNP Members
In December 2023, the topic of the 2024-2025 PIP, Improving Rates of Cancer Screening and Prevention for MMMC, CHP, and HIV SNP Members, was introduced to the MCOs via webinar, background document, and additional PIP resources. The PIP focuses on improving rates of screening for colorectal, breast, and cervical cancers and of HPV vaccinations. MMMC Plans are expected to focus on cancer screening and HPV vaccination; CHPlus Plans are expected to focus on HPV vaccination; and HIV SNP Plans are expected to focus on cancer screening. In the second quarter, the PIP Proposals were submitted by the Plans, reviewed by IPRO and NYSDOH, and feedback was provided to the Plans on any necessary revisions. All PIP proposals were approved by July 2024. In the fourth quarter, IPRO held progress calls with each individual Plan on their projects, and MCOs presented their proposals to each other by webinar. Presentations included each individual Plan's barrier analysis, key interventions to address identified barriers, the identified health disparities, and interventions to address a barrier, and how the interventions will be operationalized.2022-2023 HARP PIP: Improving Cardiometabolic Monitoring and Outcomes for HARP Members with Diabetes Mellitus
The 2022-2023 HARP PIP was completed in December 2023, and in the first quarter, all plans presented on lessons learned and next steps planned to sustain and spread successful interventions to other populations and processes. The final reports were submitted in July 2024. All final reports were reviewed by IPRO and NYSDOH and were in the process of being finalized in September 2024.2024-2025 HARP PIP: 2024-2025 Continuous Engagement in Care and Treatment
In April 2024, the topic of the 2024-2025 HARP PIP, Continuous Engagement in Care and Treatment, was introduced to the HARP MCOs via webinar, background document, and additional PIP resources, including a webinar presented by the NYS OMH on the Psychiatric Services and Clinical Knowledge Enhancement System (PSYCKES) platform for their data monitoring. In the third quarter, the HARP PIP proposals were submitted by the MCOs and reviewed by IPRO, NYSDOH, OMH, and the NYS OASAS and feedback was provided on any necessary revisions. All the 2024-2025 HARP PIP proposals were in the process of being finalized in September 2024. All-Plan Webinars were scheduled for October 15, and October 29 to discuss the individual Plan's barrier analysis, key interventions to address identified barriers, the identified health disparities, and interventions to address a barrier, and how the interventions will be operationalized.Breast Cancer Selective Contracting
Staff completed the Breast Cancer Selective Contracting process for state fiscal year 2024-2025 (April 2024 - March 2025). This included: updating the computer programs used to extract and analyze inpatient and outpatient surgical data from the Statewide Planning and Research Cooperative System (SPARCS); identifying low-volume facilities for restriction; notifying restricted facilities of their status; conducting the appeals process; posting both the list of facilities that Medicaid will pay and will not pay for breast cancer surgery to the NYSDOH public website; supplying the updated list of restricted facilities to eMedNY staff so that Medicaid FFS payments can be appropriately restricted; and, sharing the list of restricted facilities with MMC plans' chief executive officers and medical directors via the NYSDOH's Integrated Health Alerting and Notification System (IHANS).In total, the annual review identified 345 facilities performing breast cancer surgery from 2020- 2022. Facility designations were as follows: 111 high-volume facilities, 6 low-volume unrestricted facilities, 13 newly opened, unrestricted facilities and 215 low-volume restricted facilities.
Staff also completed the summer review of breast cancer surgical volume data. Provisional volume designations for contract year 2025-2026 were shared with facilities' SPARCS coordinators in July 2024. Release of these data will give facilities ample time to identify and correct any discrepancies between facility-calculated volume and SPARCS reported volume.
D. Patient Centered Medical Home (PCMH)
Federal Fiscal Quarter: 4 (7/1/2024-9/30/2024)
As of September 2024, there were 8,874 National Committee for Quality Assurance (NCQA)- recognized PCMH providers and 2,141 practices in NYS. All providers are recognized under the standards of NYS PCMH, a new recognition program that was released on April 1, 2018. NYS PCMH is based on NCQA PCMH 2017 recognition standards but requires NYS practices to meet a higher number of criteria to achieve recognition, with emphasis placed on BH, care management, population health, VBP arrangements, and health information technology capabilities. Out of the 8,874 recognized providers in September, 12 were newly enrolled in the program in July and August.
The incentive rate for the New York Medicaid PCMH Statewide Incentive Payment Program as of September 2024 is $6.00 PMPM.
The Adirondack Medical Home demonstration (‘ADK'), a multi-payer medical home demonstration in the Adirondack region, has continued with meetings for participating payers. There is still a commitment across payers and providers to continue 2025 and align on quality metrics.
All quarterly and annual reports on NYS PCMH and ADK program growth can be found on the NYSDOH website19.
Demonstration Year: 10/1/2023-9/30/2024
There has been a decline in overall participation in the PCMH program in NYS since 2020. As of October 2023, there were 9,718 NCQA-recognized PCMH providers in NYS; this number decreased to 8,874 by the end of September 2024. Additionally, the number of NCQA- recognized PCMH practices in NYS fell from 2,274 in October 2023 to 2,141 in September 2024.
IX. Financial, Budget Neutrality Development/Issues
A. Quarterly Expenditure Report Using CMS-64
Quarterly budget neutrality reporting is up to date and on schedule. The State continues to work with CMS in resolving any emergent issues with the reporting template and the Performance Metrics Database and Analytics (PMDA) system and in eliminating delays in the utilization of the Budget Neutrality Reporting Tool for quarterly reporting.
X. Other
A. Transformed Medicaid Statistical Information Systems (T-MSIS)
NYS Compliance
New York State sends the following files to CMS monthly:
- Eligibility
- Provider
- Managed Care
- Third Party Liability
- Inpatient Claims
- Long-Term Care Claims
- Prescription Drug Claims
- Other Types of Claims
The State is current in its submission of these files.
NYS is also addressing the CMS-identified data quality issues associated with the Outcomes Based Assessment (OBA) compliance criteria.
Status as of reporting month of August 2024:
Critical-Priority: 100% (Target 100%)
High-Priority: 96% (Target ≥ 99%)
Expenditures: 97% (Target ≥ 95%)As of the August 2024 reporting month, NYS data meets the Critical-Priority and Expenditures criteria target of OBA and is 3% below the target for High-Priority criterion. The State is actively working on addressing the identified high priority issues to meet the High-Priority criterion of OBA.
NYS continues to work closely with CMS and its analytics vendors to define, identify and prioritize new issues, and engage in efforts to resolve identified data quality issues.
NYS has also instituted a Data Governance workgroup for T-MSIS, to help facilitate the resolution of identified data issues. This group works with the state's T-MSIS team and the SMEs (subject matter experts) to determine when data quality issues are flagged due to reporting nuances as an outcome of program or policy under the state's approved Medicaid plan. The Data Governance workgroup supports the team's SME review(s) and provides supplemental state guidance documentation.
All these joint efforts are used to facilitate a better understanding of the NYS Medicaid program and service population(s) as reflected in the T-MSIS data submissions.
The NYS T-MSIS files are now compliant with the newer DD v3.0.0 layout as per the CMS requirement. The T-MSIS File Layout v4.x.x Specifications are currently being implemented with a target completion date no later than September 30, 2025.
B. 1115 Waiver Public Comment Days
With the implementation of the Medicaid Redesign Team in 2011, New York has prioritized transparency and public engagement as a key element of developing and implementing Medicaid policies. The public comments provided at these forums have been shared with the New York teams working on these programs and has informed implementation activities. We will continue to consider these issues and engage stakeholders as part of our ongoing efforts.
On February 28, 2024, NYS DOH conducted a virtual public forum, which dually served as a public hearing for an upcoming 1115 amendment request. During the public forum, NYS DOH received insightful comment from six speakers on a range of topics, including the proposed amendment request, the recently approved NYHER amendment, and NY's aging population and long-term care services. Comments were shared with the program areas within the state for their consideration in shaping policy and procedures.
A recording of the live webcast, transcript, and presentation slides from the public forum are available for viewing on the NY 1115 webpage 20.
C. HCBS Quality Measures
NYS is working to schedule a technical assistance call with CMS's contractor, New Editions, after reviewing the HCBS quality measures and reporting requirements outlined in the 2014 Center for Medicaid & CHIP Services (CMCS) Informational Bulletin (CIB), Modifications to Quality Measures and Reporting in §1915(c) Home and Community-Based Waivers, regarding Quality Improvement Strategy (QIS).
Attachments:
Attachment 1— MLTC Critical Incidents
Attachment 2— MLTC Partial Capitation Plan, MAP, PACE, MA and FIDA IDD EnrollmentState Contact:
Simone Milos
Medicaid Redesign Analyst II Strategic Operations and Planning Office of Health Insurance Programs Simone.Milos@health.ny.gov
Phone (518) 473-0868
Fax (518) 473-1764Uploaded to PMDA: December 27, 2024
Plan Name Number of Critical Incidents Wrongful Death Use of Restraints Medication errors that resulted in injury Instances of Abuse, Neglect and/or Exploitation of Enrollees Involvement with the Criminal Justice System Other Incident Resulting in Hospitalization Other Incident Resulting in Medical Treatment Other than Hospitalization Any Other Incidents as Determined by DOH Enrollment Critical Incidents as a Percentage of Enrollment Aetna Better Health 17 0 0 0 2 0 11 4 0 6467 0.26% Archcare Community Life 11 0 0 0 0 0 5 5 1 824 1.33% Catholic Health-LIFE 14 0 6 0 0 1 2 5 0 242 5.79% Centerlight PACE 56 0 0 1 0 0 23 26 6 6358 0.88% Centers Plan for Healthy Living 1057 1 0 2 35 4 265 750 0 53599 1.97% Centers Plan for Healthy Living MAP 48 0 0 0 6 1 8 33 0 1887 2.54% Complete Senior Care 5 0 0 0 0 0 5 0 0 136 3.68% Eddy SeniorCare 3 0 0 0 0 0 0 3 0 414 0.72% Elderplan MAP 6 0 0 1 3 0 0 0 2 4551 0.13% Elderserve 480 0 2 0 2 5 104 229 138 19290 2.49% Elderserve MAP 8 0 0 0 0 3 2 0 3 352 2.27% Empire BlueCross BlueShield Healthplus 0 0 0 0 0 0 0 0 0 59927 0.00% Empire BlueCross BlueShield Healthplus MAP 0 0 0 0 0 0 0 0 0 207 0.00% Fidelis Care at Home 53 0 0 0 4 4 20 25 0 19214 0.28% Fidelis MAP 3 0 0 0 0 0 1 2 0 1698 0.18% Hamaspik 175 0 0 0 1 0 81 67 26 8233 2.13% Hamaspik MAP 49 0 0 0 1 0 32 16 0 976 5.02% Healthfirst CompleteCare 202 0 0 1 5 3 83 89 21 32283 0.63% HomeFirst, Inc. (Elderplan) 12 0 0 0 10 0 0 1 1 25781 0.05% Icircle 6 0 0 0 1 4 0 0 1 4229 0.14% Independent Living for Seniors (ILS/ElderOne) 1 0 0 0 0 0 0 0 1 750 0.13% Independent Living Services of CNY (PACE CNY) 19 0 0 0 0 0 14 5 0 582 3.26% Kalos ErieNiagara DBA: First Choice Health 14 0 0 0 2 0 12 0 0 1040 1.35% MetroPlus MAP 0 0 0 0 0 0 0 0 0 199 0.00% MetroPlus 2 0 0 0 0 0 0 2 0 2386 0.08% Senior Health Partners 44 0 0 0 1 3 17 18 5 9772 0.45% Senior Whole Health 0 0 0 0 0 0 0 0 0 28254 0.00% Senior Whole Health MAP 0 0 0 0 0 0 0 0 0 285 0.00% Total Senior Care 14 0 0 0 1 0 2 11 0 128 10.94% Village Care 258 1 0 0 21 5 72 159 0 28943 0.89% Village Care MAP 57 0 0 0 9 1 18 29 0 3470 1.64% VNA Homecare Options (Nascentia Health Options) 175 1 0 1 6 3 52 112 0 6264 2.79% VNS Choice MAP TOTAL 57 0 0 0 4 0 9 44 0 4816 1.18% VNS Choice MLTC 468 0 0 0 28 7 112 321 0 25752 1.82% Total 3314 3 8 6 142 44 950 1956 205 359309 0.92%
Managed Long Term Care Partial Capitation Plan Enrollment Oct 2023 to Sep 2024 Plan Name Oct-23 Nov-23 Dec-23 Jan-24 Feb-24 Mar-24 Apr-24 May-24 Jun-24 Jul-24 Aug-24 Sep-24 Enrollment Enrollment Enrollment Enrollment Enrollment Enrollment Enrollment Enrollment Enrollment Enrollment Enrollment Enrollment Aetna Better Health 5919 6000 6070 6089 6078 6120 6184 6264 6313 6394 6471 6535 Centers Plan for Healthy Living 51557 52051 52418 52712 52623 52674 52982 53051 53079 53315 53596 53885 Elderplan 20598 21083 21444 21918 22146 22676 23188 24438 24806 25399 25743 26201 Elderserve 16793 16949 17098 18367 18374 18478 18624 18813 18900 19083 19300 19488 Fidelis Care at Home 16962 17436 17665 17800 18330 18456 18653 18817 18776 18957 19278 19406 Hamaspik Choice 7490 7533 7649 7706 7735 7811 7907 8006 8066 8216 8220 8262 HealthPlus- Amerigroup 55260 56160 56458 56466 56431 57019 57534 58036 58521 59250 60000 60531 iCircle Services 3568 3602 3624 3682 3683 3771 3911 3999 4054 4159 4221 4307 Kalos Health- Erie Niagara 710 780 850 938 942 935 956 997 1007 1033 1038 1049 MetroPlus MLTC 1527 1565 1620 1652 1735 1777 1878 2002 2141 2284 2392 2481 Senior Health Partners 9118 9113 9182 9157 9455 9460 9460 9515 9509 9624 9804 9889 Senior Whole Health 26870 27079 27410 27672 27796 28297 28648 28900 28799 28488 28261 28014 Village Care 19523 20095 20608 20796 20998 21389 21885 22387 28132 28581 28941 29308 VNA HomeCare Options 4751 4870 5026 5199 5328 5448 5670 5772 5914 6087 6269 6436 VNS Choice 23498 23664 23789 23568 23335 23317 23438 25137 25361 25594 25774 25887 Total 264,144 267,980 270,911 273,722 274,989 277,628 280,918 286,134 293,378 296,464 299,308 301,679
Managed Long Term Care MAP Enrollment Oct 2023 to Sep 2024 Plan Name Oct-23 Nov-23 Dec-23 Jan-24 Feb-24 Mar-24 Apr-24 May-24 Jun-24 Jul-24 Aug-24 Sep-24 Enrollment Enrollment Enrollment Enrollment Enrollment Enrollment Enrollment Enrollment Enrollment Enrollment Enrollment Enrollment Fidelis 1118 1116 1131 1152 1181 1283 1379 1456 1533 1612 1692 1791 Hamaspik 840 848 852 849 900 916 928 925 943 975 980 974 Centers 1641 1588 1553 1698 1745 1768 1803 1846 1858 1866 1895 1900 Elderplan 3485 3524 3647 3795 3927 4005 4136 4238 4348 4437 4558 4658 Elderserve 245 261 282 278 279 291 297 316 327 334 353 369 Healthfirst Complete Care 26897 27297 27649 28341 28866 29416 29962 30568 31233 31745 32326 32777 Healthplus 119 113 116 121 130 135 141 149 171 204 212 205 Metroplus 159 168 173 172 170 177 187 196 196 198 197 201 Senior Whole Health 221 227 249 252 265 286 300 298 294 289 284 283 VNS 3957 3946 3886 4172 4308 4393 4487 4585 4676 4714 4823 4910 Village Care 2689 2672 2629 2787 2869 2952 3061 3118 3188 3297 3478 3635 Total 41371 41760 42167 43617 44640 45622 46681 47695 48767 49671 50798 51703
Managed Long Term Care PACE Enrollment Oct 2023 to Sep 2024 Plan Name Oct-23 Nov-23 Dec-23 Jan-24 Feb-24 Mar-24 Apr-24 May-24 Jun-24 Jul-24 Aug-24 Sep-24 Enrollment Enrollment Enrollment Enrollment Enrollment Enrollment Enrollment Enrollment Enrollment Enrollment Enrollment Enrollment Archcare 793 805 799 807 803 809 807 822 835 821 823 828 CHS Buffalo Life 226 227 228 229 233 233 233 231 235 240 241 244 Complete Senior Care 137 135 133 136 138 135 135 134 135 136 135 137 Comprehensive Care Management 6333 6372 6379 6331 6313 6348 6295 6311 6267 6297 6360 6418 Eddy Senior Care 341 357 370 360 375 383 393 405 408 414 411 416 Fallon Health PACE 155 154 161 168 161 159 157 161 164 168 173 181 Independent Living For Seniors 752 749 750 748 744 755 749 749 748 740 753 757 Pace CNY 556 559 558 551 546 545 561 568 564 576 581 588 Total Senior Care 131 129 127 131 128 129 127 127 126 128 126 130 Total 9424 9487 9505 9461 9441 9496 9457 9504 9479 9520 9603 9699
Managed Long Term Care FIDA-IDD Enrollment Oct 2023 to Sep 2024 Plan Name Oct-23 Nov-23 Dec-23 Jan-24 Feb-24 Mar-24 Apr-24 May-24 Jun-24 Jul-24 Aug-24 Sep-24 Enrollment Enrollment Enrollment Enrollment Enrollment Enrollment Enrollment Enrollment Enrollment Enrollment Enrollment Enrollment Partners Health Plan 1717 1711 1703 1690 1683 1699 1694 1689 1688 1703 1702 1703
____________________________________________
1. Q4 data is not available and will be submitted with the next quarterly update. 1
2. Q4 data is not available and will be submitted with the next quarterly update.. 2
3. As of May 2023, MCTAC included pre-recorded offerings in the total count of events.. 3
4. Q4 2024 award amounts are not yet available and will be submitted with the next quarterly update.. 4
5. https://shinny.org/us/ny/hrsn/. 5
6. Amended Part 820 Effective October 1, 2022. 6
7. Residential Redesign Conversion Application. 7
8. Offie of Addiction Services and Supports. 8
9. Conversion from Part 819 to Part 820 Residential Service. 9
10. Medicaid Managed Care/Family Health Plus/Hiv Special Needs Plan/Health And Recovery Plan Model Contract. 10
11. Level of Care Determination (LOCADTR). 11
12. Health Commerce System (HCS). 12
13. NYS Open Legislation | NYSenate.gov. 13
14. MLTC Consumer Regional Quality Guides. 14
15. Managed Long-Term Care Regional Consumer Guide. 15
16. Managed Long-Term Care (MLTC) Reports. 16
17. Managed Long-Term Care 2023 Member Satisfaction Survey Summary Report. 17
18. Managed Long-Term Care Performance Data: Beginning 2014. 18
19. New York State Patient-Centered Medical Home (NYS PCMH). 19
20. Slides PDF - Recording - Transcript 20
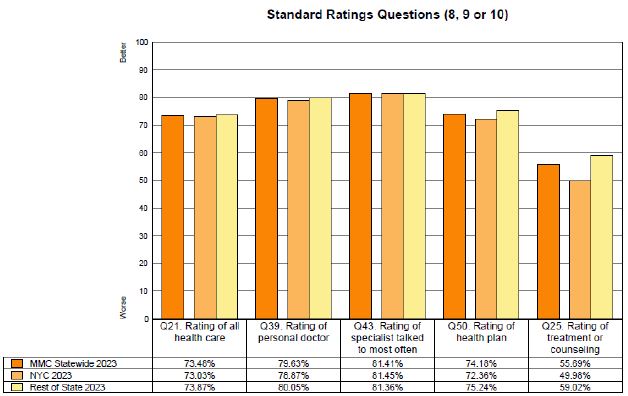
Follow Us