Alpha-gal Syndrome (AGS)
What is alpha-gal and alpha-gal syndrome (AGS)?
- Alpha-gal is a sugar molecule found naturally in some types of food, animal products, and tick saliva.
- Alpha-gal syndrome (AGS) is an allergy to foods containing alpha-gal. This occurs after people are bitten by ticks, especially the lone star tick.
- Other names for AGS include mammalian meat allergy, alpha-gal allergy, red meat allergy, and tick bite meat allergy.
- AGS is not caused by a virus, parasite, or bacteria.
- AGS is a serious and potentially lifelong condition that can occur after a tick bite, even if the tick is removed promptly. Therefore, prevention is extremely important.
Where does AGS occur?
- In the United States (U.S.), many people who have AGS live in Southern, Eastern, and Central states.
- New York State residents are diagnosed with AGS every year, particularly on Long Island where lone star ticks are common.
- Rates of people with positive alpha-gal laboratory test results in the U.S., by county, can be viewed on this CDC map, but viewers should keep in mind that a positive test result doesn't necessarily mean a person has AGS.
How would I get AGS?
- Alpha-gal molecules are a normal part of tick saliva of some tick species, but some people can become sensitive to alpha-gal following tick bites.
- In New York State, AGS is mostly associated with lone star tick bites, but other kinds of ticks have the potential to trigger the allergy.
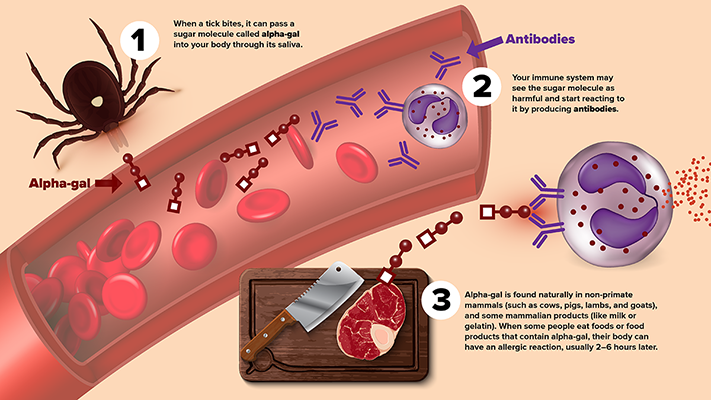
- When a tick bites, it can pass a sugar molecule called alpha-gal into your body through its saliva.
- Your immune system may see the sugar molecule as harmful and start reacting to it by producing antibodies.
- Alpha-gal is found naturally in non-primate mammals (such as cows, pigs, lambs, and goats), and some mammalian products (like milk or gelatin). When some people eat foods or food products that contain alpha-gal, their body can have an allergic reaction, usually 2–6 hours later.
Lone star ticks

(Images courtesy of JL Occi)
- Lone star ticks do not always have a white dot.
- Lone star ticks look different when they reach different stages in their life.
- Bites from larval lone star ticks, the youngest and smallest life stage, are also associated with AGS.
- Not everyone bitten by a lone star tick will develop AGS.
Who is at risk for AGS?
- Anyone can be at risk for AGS, but especially those who spend time outdoors. This includes:
- People who frequently spend time outside (such as hikers, gardeners, and hunters).
- People who work outdoors (such as farmers, construction workers, and landscapers).
- People of all ages can develop AGS, but most cases have been reported in adults.
What does AGS look like?
- AGS symptoms can differ from person-to-person ranging from mild to severe.
- Unlike conditions where symptoms occur without a specific trigger, AGS symptoms are directly related with the consumption of foods or food products that contain alpha-gal.
- AGS symptoms are usually delayed. They appear 2-6 hours after consuming products that contain alpha-gal.
- Anyone who has a severe allergic reaction should seek emergency medical care right away.
- Some people may not be allergic at all.
- 1. Lone star tick bite(s) occur.
- 2. Then, weeks to months later…
- 3. Foods or products that contain alpha-gal are consumed.
- 4. Two to six hours pass. AGS symptoms develop.
- 5-7. Symptoms can include:
- Rash or hives
- Gastrointestinal symptoms (such as stomach pain, nausea, vomiting, diarrhea, heartburn, and indigestion)
- Swelling of the lips, throat, tongue, or eyelids
- Cough, shortness of breath, wheezing, and difficulty breathing
- Severe symptoms can include:
- a drop in blood pressure,
- dizziness,
- feeling faint/fainting,
- severe stomach pain, and/or
- anaphylaxis
Prevention & tick removal
AGS is a serious and potentially lifelong condition that can occur after a tick bite, even if the tick is removed promptly. Therefore, prevention is extremely important.
To help prevent AGS, practice techniques to reduce your chances of a tick bite:
- Consider using EPA-registered repellents. Check the label to make sure the repellent works against ticks and follow the instructions.
- Consider treating clothing and gear with products containing permethrin. Permethrin is an EPA-registered insecticide that kills ticks on contact.
- Wear light-colored clothes so you can easily spot and remove ticks.
- Tuck the ends of your pants into socks or boots and shirts into pants.
- Walk in the center of hiking trails.
- Avoid tick-heavy outdoor places including fallen leaves and wooded, bushy, and grassy areas.
- Regularly check for ticks when outdoors and at home.
- Put clothes on high heat in dryer for 10 minutes to kill ticks.
- Shower after spending time outdoors.
- Remove attached ticks (youtube) right away. Don't wait.
- Make sure to include any outdoor pets in a tick check. Ticks can catch a ride into your home on your outdoor animals, which increases the chances of a tick bite at home.
To help prevent the symptoms of AGS if you already have it:
- Avoid foods with alpha-gal, like meat from mammals (such as beef, pork, rabbit, lamb, and venison) and some mammalian products (including gelatin and milk products). A comprehensive list can be found within CDC’s Fast Facts: Products That May Contain Alpha-gal.
- A person with AGS can still eat meat that does not contain alpha-gal, like poultry (such as chicken and turkey) and fish.
For more information about tick removal and prevention, visit: Lyme Disease and Other Diseases Carried by Ticks.
How is AGS diagnosed?
Diagnosis of AGS involves a combination of symptoms, medical examination, and testing.
To diagnose AGS, an allergy specialist or health care provider needs:
- A detailed patient history,
- A medical examination, and
- A blood test that looks for alpha-gal-specific IgE antibodies.
AGS testing
- Alpha-gal-specific IgE antibody testing is the main type of AGS testing.
- A positive alpha-gal-specific IgE test alone does not necessarily mean someone has AGS. Some people have a positive alpha-gal specific IgE test without an AGS reaction. Therefore, in addition to testing, AGS is diagnosed using a detailed patient history and medical examination.
How is AGS treated?
- AGS should be managed under the care of an allergist or health care provider familiar with AGS.
- People with AGS should practice tick bite prevention techniques because new tick bites may reactivate allergic reactions to alpha-gal. A provider will likely recommend that a patient with AGS avoid food and food products that contain alpha-gal.
- A person with AGS can still eat meat that does not contain alpha-gal, like poultry (such as chicken and turkey) and fish.

