Patient Driven Payment Model (PDPM) CASE MIX PROJECT UPDATE
- Update also available in Portable Document Format (PDF)
OHIP / DFRS / NHLTCRS
May13, 2025
AGENDA
- Introductions
- Project to date
- Where we are now
- MDS analysis details
- Industry guidance
- Next steps
PROJECT TO DATE
- Myers and Stauffer contract began April 15, 2024
- Planning, NYS regulations and rate methodology, preliminary data analysis, etc.
- CMS DUA approved November 19, 2024
- MDS data shared with Myers and Stauffer:
- Quarterly MDS data files from Q1 2022 through Q3 2023
- Daily MDS submission files from Q4 2022 through Q1 2024
- Myers and Stauffer has spent the last few months completing a thorough analysis of the MDS data
WHERE WE ARE NOW
- While some aspects of the data can be used for modeling case mix rate adjustments, other aspects are incomplete and cannot be used
- Only two of the five PDPM components can be accurately discerned from the current data:
- Nursing and Non-Therapy Ancillary (NTA) can be used
- Physical Therapy, Occupational Therapy, and Speech Language Pathology cannot be used
- This increased understanding of PDPM assessments enables us to provide further instruction on what is needed for rate setting
- Additional fields will be requested, which will allow for DOH and Myers and Stauffer to complete a thorough analysis of the impacts of all five PDPM components
- We will discuss these fields and the draft guidance in subsequent slides
- Because this will take additional time, we are looking to implement an interim case mix methodology that may rely only on the Nursing and/or NTA components while we collect and analyze additional data
- This will turn the PDPM case mix transition into a two-step process at least, but will allow for a case mix adjustment to occur sooner.
- Collaborative options for phase in, reconciliation, and impacts will be discussed as a part of this process
- After this thorough data analysis, Myers and Stauffer will be equipped to work more closely with the Department and industry on specific ideas, impacts, and elements of the assessments.
- Though the Nursing component is generally the key element, the other PDPM components could still be fully analyzed.
Myers and Stauffer MDS Data Analysis
ACRONYMS USED IN THIS PRESENTATION
- CMI
Case-Mix Index; a weight assigned to a specific Resource Utilization Group or an average for a given population.
- MDS
Minimum Data Set; a core set of screening, clinical and functional elements, specific instructions and schedule of assessments.
- PDPM
Patient Driven Payment Model; for Medicare Part A SNF resident stays only; replaced RUG-IV 10/1/2019.
- NTA
Non-Therapy Ancillary case-mix component of PDPM.
- HIPPS
Health Insurance Prospective Payment System code set. Reported codes that contain signifiers for PDPM component grouping.
- PT
Physical Therapy case-mix component of PDPM.
- OT
Occupational Therapy case-mix component of PDPM.
- SLP
Speech Language Pathology case-mix component of PDPM.
- RUG-III, RUG-IV
Resource Utilization Group, Versions III and IV, a nursing facility resident classification system used in case-mix reimbursement methodology.
PDPM Reimbursement Model
Resident Characteristic Driven Model
- Rate built upon resident characteristics, not volume of services, and designed to better meet individual care needs.
- Certain rate components include a variable per diem adjustment.
- Rate calculation includes:
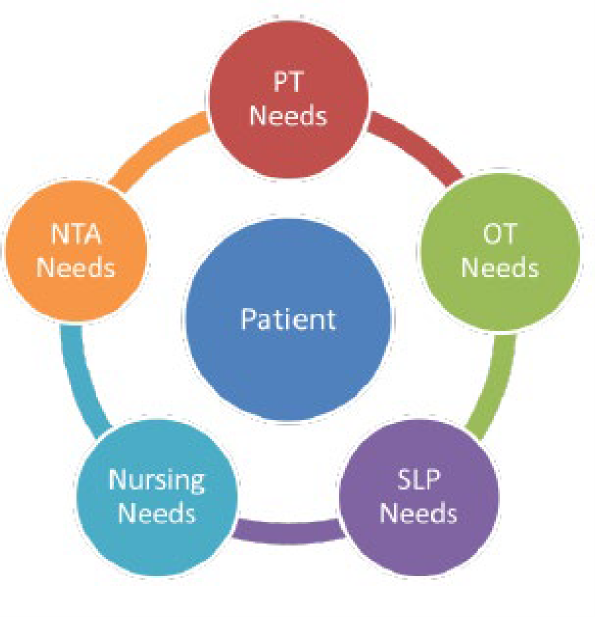
- Five Case-Mix Adjusted Components: PT, OT, SLP, Non-Therapy Ancillary, & Nursing
- One Non-Case Mixed Base Rate Component
- Quarterly MDS data files from Q1 2022 through Q3 2023
- Daily MDS submission files from Q4 2022 through Q1 2024
- Nursing and Non-Therapy Ancillary (NTA) can be used
- Physical Therapy, Occupational Therapy, and Speech Language Pathology cannot be used
- This will turn the PDPM case mix transition into a two-step process at least, but will allow for a case mix adjustment to occur sooner.
- Collaborative options for phase in, reconciliation, and impacts will be discussed as a part of this process
Case-Mix Index; a weight assigned to a specific Resource Utilization Group or an average for a given population.
Minimum Data Set; a core set of screening, clinical and functional elements, specific instructions and schedule of assessments.
Patient Driven Payment Model; for Medicare Part A SNF resident stays only; replaced RUG-IV 10/1/2019.
Non-Therapy Ancillary case-mix component of PDPM.
Health Insurance Prospective Payment System code set. Reported codes that contain signifiers for PDPM component grouping.
Physical Therapy case-mix component of PDPM.
Occupational Therapy case-mix component of PDPM.
Speech Language Pathology case-mix component of PDPM.
Resource Utilization Group, Versions III and IV, a nursing facility resident classification system used in case-mix reimbursement methodology.
- Five Case-Mix Adjusted Components: PT, OT, SLP, Non-Therapy Ancillary, & Nursing
- One Non-Case Mixed Base Rate Component
Source: CMS Presentation, "Patient Driven Payment Model: Background & Finalized Changes to the Skilled Nursing Facility (SNF) Prospective Payment System (PPS)"
MDS Processing Update
Q2 2022 Through Q1 2024
MDS assessment data has been shared with Myers and Stauffer, but numerous deficiencies were noted.
- Around 30% of original MDS assessments generated a HIPPS code capturing PDPM component classifications.
- HIPPS codes issues were due to missing fields from MDS assessments
- The main missing MDS fields are as follows:
- I0020
- J2100
- O0400D
- A provider memo is being disseminated discussing the need to complete these fields on all MDS assessments going forward
Myers and Stauffer completed missing MDS assessment fields in order to calculate partial HIPPS codes to compensate for the data deficiencies.
- PDPM Nursing and NTA calculations reconstructed from MDS assessment data.
- PT, OT, and SLP data unable to be constructed accurately from MDS assessment data.
- Approximately 150-170k usable records per quarter with 70k-90k usable Medicaid records once re-processed.
DOH MDS GUIDANCE AND NEXT STEPS
DRAFT GUIDANCE FOR DISCUSSION
Key text from draft DAL:
Effective June 1, 2025, nursing facilities are required to complete the following three MDS items (in addition to those already required) on all federally required MDS assessment submissions:
- I0020: Indicate the resident's primary medical condition category
- J2100: Recent Surgery Requiring Active SNF Care
- O0400D: Respiratory Therapy
Though these fields are not required by the Centers for Medicare & Medicaid Services (CMS) as part of the Omnibus Budget Reconciliation Act (OBRA) assessment, they are key elements in the Patient Driven Payment Model (PDPM) schema that will assist NYS DOH in analyzing the assessment data for future case mix adjustments. Completion of these items will allow for PDPM categorization of all submitted assessments
QUESTIONS ABOUT DRAFT GUIDANCE
- What will it take for facilities to implement this change?
- Is the start date of June 1, 2025 feasible?
- Would it be possible to update assessment data retroactively?
- Are there technology constraints? Training concerns?
- Are there concerns with this approach?
- Any recommendations based on your expertise?
NEXT STEPS – Final Methodology
- Timeline for collecting additional data and conducting further analysis:
- New data collection beginning June 1, 2025 (feedback appreciated)
- Several months of data are needed, so we are targeting November 1, 2025 for beginning analysis
- We are aiming to have a new model to review with stakeholders in Spring 2026 for feedback and possible recommendations
- Final methodology to be implemented Fall 2026
NEXT STEPS – Interim Methodology
- Timeline for having an interim methodology to review with stakeholders:
- Myers and Stauffer is working on this now
- We are aiming to review with stakeholders around the end of summer 2025
- Once a methodology is agreed to, DOH will do SPA and regs as needed.