MY2024 Value Based Payment Reporting Requirements
Technical Specifications Manual
- Manual is also available in Portable Document Format (PDF)
____________________________________________________________
New York State Department of Health
Email Address: OHSQAVBP@health.ny.gov
Last Revised: January 2025
Table of Contents
- INTRODUCTION
- REPORTING GUIDELINES VBP MAINSTREAM & SUBPOPULATIONS
- REPORTING GUIDELINES VBP MLTC
- INTRODUCTION
- MEASURE CHANGES
- TABLE 2: 2024 MLTC VBP LIST OF REQUIRED MEASURES
- MLTC ATTRIBUTION FILE
- ATTRIBUTION METHODOLOGY
- FILE FORMAT
- FIELD DEFINITIONS
- FILE SUBMISSION
- TABLE 3: 2024 VBP LIST OF CATEGORY 2 MEASURES
- TABLE 4: 2024 VBP MLTC CATEGORY 2 MEASURES
- TABLE 5: NYS FIPS CODES BY COUNTY
- TABLE 6: SUBMISSION EXAMPLES
- TABLE 7: MCO ATTRIBUTION FILE - DATA QUALITY CHECKLIST
- TABLE 8: MLTC ATTRIBUTION FILE - DATA QUALITY CHECKLIST
| Important Dates & Contact Information | ||||
|---|---|---|---|---|
| Mainstream VBP | MLTC VBP | |||
| Contact | OHSQAVBP@health.ny.gov | Contact | MLTCVBP@health.ny.gov | |
| Submission Date | All files must be received electronically by 11:59 p.m. EST Friday, July 25, 2025. | Submission Date | Plan/Provider-VBP Contractor performance to the Department by Friday, July 25, 2025 | |
| MLTC VBP data files: All files must be received electronically by 11:59 p.m. EST Friday, July 25, 2025 | ||||
| Health Commerce System (HCS) | To: OHSQA VBP Evaluation | Health Commerce System (HCS) | To: MLTC VBP Evaluation | |
I. Submission Requirements
INTRODUCTION
In 2022 HEDIS introduced a new naming convention to help reduce confusion about reporting year (RY) and measurement year (MY); going forward, all HEDIS publications referred to measurement year. NYS QARR updated its publication titles to refer to the measure year during this time. To align with these changes, NYS Value Based Payment (VBP) publication titles will also refer to the measure year.
The purpose of this document is to make stakeholders aware of the quality measure reporting requirements for Medicaid Managed Care Organizations (MCOs) participating in the New York State (NYS) Medicaid Value-Based Payment (VBP) program. The 2024 VBP Reporting Requirements refer to data for Measurement Year 2024 (MY2024).
Sections II, III, and IV of this document include guidance for the organizations responsible for reporting, the subset of measures for which reporting will be required by Mainstream VBP Arrangements, and the changes to the reportable set of MY2024 Quality Measure Sets (see TABLE 1: 2024 VBP LIST OF REQUIRED MEASURES). Sections V and VI provide guidance for Managed Long-Term Care (MLTC) VBP Arrangements.
The New York State Department of Health (Department) has completed the first phase of a health transformation effort, known as the Department Innovation Model (SIM) award, which focused on the transformation of primary care delivery and payment models statewide. The New York State Patient Centered Medical Home (NYS PCMH) model was created as part of the SIM initiative. With NYS PCMH, a Primary Care Core measure set was developed, and multi-payer data is used to calculate results for practices for the measure. To reduce the burden on MCOs participating in both the NYS Primary Care measure set model and Medicaid VBP, we are aligning the reporting for both programs and utilizing the NYS Primary Care Core Set Scorecard data request to fulfill reporting requirements for both programs, where possible.
VBP ARRANGEMENTS AND ASSOCIATED QUALITY MEASURES
The VBP Roadmap updated in May 2022, outlines six types of VBP arrangements to be included for MY2024:
- Total Care for the General Population (TCGP) Arrangement: Includes all costs and outcomes for care, excluding certain subpopulations (specified below).
- Total Care for Special Needs Subpopulation Arrangements: Includes costs and outcomes of total care for all members within a subpopulation exclusive of TCGP.
- Children's Subpopulation: to address the unique needs of children at different developmental stages
- Behavioral Health/Health and Recovery Plans (HARP): for those with Serious Mental Illness or Substance Use Disorders
- People Living with Human Immunodeficiency Virus/Acquired Immunodeficiency Syndrome (HIV/AIDS)
- Managed Long Term Care (MLTC)
- Episodic Care Arrangements
- Maternity Care: Includes episodes associated with a pregnancy, including prenatal care, delivery and postpartum care through 60 days post-discharge for the mother, and care provided to the newborn from birth through the first 30 days post-discharge.
CATEGORIZATION OF QUALITY MEASURES
Through a multi-group stakeholder engagement process, a set of quality measures was defined for each arrangement. Based on an analysis of clinical relevance, reliability, validity, and feasibility, each measure was placed into one of three categories:
- Category 1: (CAT 1) Selected as clinically relevant, reliable, valid, and feasible. These measures are outlined in Table 1.
- REQUIREMENT: Only the CAT 1 measures that are indicated in this document as "Required to Report" (✓) are to be reported by the MCO to the Department.
- Category 2: (CAT 2) Seen as clinically relevant, valid, and reliable, but where the feasibility could be problematic.
Category 2 measures are listed in the appendix (Table 3) of this guide. - Category 3: (CAT 3) Rejected based on a lack of relevance, reliability, validity, and/or feasibility. These measures are not included in this manual.
CLASSIFICATION OF QUALITY MEASURES
Each CAT 1 measure is classified as either Pay-for-Performance (P4P) or Pay-for-Reporting (P4R). P4P measures are intended to be used in the determination of shared savings amounts for which VBP Contractors are eligible. P4R measures are intended to be used by the MCOs to incentivize the VBP Contractors for reporting data to monitor the quality of care delivered to members in a VBP contract.
|table of contents|ORGANIZATIONS REQUIRED TO REPORT
Medicaid Managed Care Organizations with Level 1 or higher value based contracting arrangements are required to report. All submissions must be received electronically by 11:59 p.m. EST on Friday, July 25, 2025.
|table of contents|REPORTING GUIDELINES VBP MAINSTREAM & SUBPOPULATIONS
II. Reporting Guidelines VBP Mainstream & Subpopulations
MAINSTREAM & SUBPOPULATION VBP ARRANGEMENTS [OTHER THAN MLTC]
The Department requests that Medicaid Managed Care (MMC) plans submit data files leveraging their 2024 Quality Assurance Reporting Requirements (QARR) (HEDIS®)1 submission which will be used to create aggregated quality results by VBP Contractor for all members in a VBP Arrangement. Specifically, the Department is asking insurers to provide a modified version of the NYS Patient-Level Detail (PLD) file, along with provider and practice information. Submission of the NYS PCMH Patient-Level Detail file for all members in a Level 1 or higher VBP Arrangement will fulfill this reporting requirement. The NYS PCMH Patient-Level Detail File layout is included in Section IV of this manual. The Department is also requesting a separate Patient Attribution file for all members in a Level 1 or higher VBP Arrangement. The Patient Attribution file layout is also included in Section IV, File Specifications - Mainstream VBP.
Table 1: MY2024 VBP List of Required Measures
- Lists, by arrangement, the 2024 VBP Category 1 Measure sets and indicates the 2024 measures the Department is requiring for reporting.
- Section IV:File Specifications required for reporting.
- This manual describes reporting requirements only. For VBP reporting or contracting questions, please contact OHSQAVBP@health.ny.gov.
- Organizations must purchase the HEDIS® 2024 Technical Specifications for descriptions of the required HEDIS® measures. For specifications for other non-HEDIS measures, please contact the measure steward for the correct version of the specification. NYS-specific measures are defined in the 2024 Quality Assurance Reporting Requirements (QARR) Technical Specifications Manual.
MEASURE CHANGES
Changes to the Reporting Requirements for MY2024 Measure Sets were made based on the feedback received by the Department from the Clinical Advisory Groups, HEDIS measurement changes, and other stakeholder groups. Those changes are indicated in the publicly posted MY2024 VBP Measure Sets. All measures required for VBP reporting are included in either the QARR PLD file or NYS PCMH file as outlined in Table 1: 2024 Mainstream VBP List of Required Measures. Please follow any measure changes or updates as indicated by the measure steward, the QARR technical specifications or the NYS PCMH file instructions.
WHERE TO SUBMIT VBP REPORTING DATA
- Electronically submit all files (no later than 11:59 p.m. EST on Friday, July 25, 2025) via a secure file transfer application. Do not mail materials.
- Specific delivery instructions are given for each file.
WHAT TO SEND FOR VBP REPORTING
- The Department is requesting a NYS PCMH file and a Patient Attribution file for ALL members in a VBP Level 1 or higher Arrangement.
*****All submissions must be received electronically by 11:59 p.m. EST on Friday, July 25, 2025.*****
QUESTIONS CONCERNING 2024 VBP REPORTING
Please submit all questions to OHSQAVBP@health.ny.gov.
|top of section| |table of contents|III. Reporting Requirements Mainstream VBP
TABLE 1: 2024 MAINSTREAM VBP LIST OF REQUIRED MEASURES
| Measures | Notes | Arrangement Type | Specifications | Class | |||||
|---|---|---|---|---|---|---|---|---|---|
| TCGP | Maternity | HARP | HIV/AIDS | Children's | |||||
| Total Care for the General Population (TCGP) | |||||||||
| Adherence to Antipsychotic Medications for Individuals with Schizophrenia (SAA) | 3 | ✓ | NA | ✓ | NA | NA | CMS 2024 | P4P | |
| Adult Immunization Status - Electronic (Influenza) (AIS- E) | 3 | ✓ | NA | ✓ | NA | NA | HEDIS 2024 | P4P | |
| Antidepressant Medication Management - Effective Acute Phase Treatment & Effective Continuation Phase Treatment (AMM) | ✓ | NA | NA | ✓ | NA | HEDIS 2024 | P4P | ||
| Asthma Medication Ratio (AMR) | ✓ | NA | ✓ | ✓ | ✓ | HEDIS 2024 | P4P | ||
| Breast Cancer Screening (BCS-E) | ✓ | NA | ✓ | ✓ | NA | HEDIS 2024 | P4P | ||
| Cervical Cancer Screening (CCS, CCS-E) | 2 | ✓ | NA | ✓ | ✓ | NA | HEDIS 2024 | P4P | |
| Child and Adolescent Well-Care Visits (WCV) | ✓ | NA | NA | NA | ✓ | HEDIS 2024 | P4P | ||
| Childhood Immunization Status - Combination 3 (CIS, CIS-E) | 2 | ✓ | NA | NA | NA | ✓ | HEDIS 2024 | P4P | |
| Chlamydia Screening in Women (CHL) | ✓ | NA | ✓ | NA | ✓ | HEDIS 2024 | P4P | ||
| Colorectal Cancer Screening (COL-E) | 2 | ✓ | NA | ✓ | ✓ | NA | HEDIS 2024 | P4P | |
| Controlling High Blood Pressure (CBP) | 2 | ✓ | NA | ✓ | ✓ | NA | HEDIS 2024 | P4P | |
| COVID-19 Immunization Measure (CVS) | 3 | ✓ | ✓ | ✓ | ✓ | ✓ | NYS 2024 | P4P | |
| Depression Remission or Response for Adolescents and Adults (DRR-E) | ✓ | NA | NA | ✓ | ✓ | HEDIS 2024 | P4P | ||
| Developmental Screening Using Standardized Tool, First Three Years of Life (DEV-N) | ✓ | NA | NA | NA | ✓ | OHSU/NYS 2024 | P4R | ||
| Diabetes Screening for People with Schizophrenia or Bipolar Disorder Using Antipsychotic Medications (SSD) | ✓ | NA | ✓ | ✓ | NA | HEDIS 2024 | P4P | ||
| Eye Exam for Patients with Diabetes (EED) | 2 | ✓ | NA | ✓ | ✓ | NA | HEDIS 2024 | P4P | |
| Follow-Up After Emergency Department Visit for Mental Illness (FUM) | 3 | ✓ | NA | ✓ | NA | ✓ | HEDIS 2024 | P4P | |
| Follow-Up After Emergency Department Visit for Substance Use (FUA) | 3 | ✓ | NA | ✓ | NA | NA | HEDIS 2024 | P4P | |
| Follow-Up After High-Intensity Care for Substance Use Disorder (FUI) | 3 | ✓ | NA | ✓ | NA | NA | HEDIS 2024 | P4P | |
| Follow-Up After Hospitalization for Mental Illness (FUH) | 3 | ✓ | NA | ✓ | NA | NA | HEDIS 2024 | P4P | |
| Glycemic Status Assessment for Patients with Diabetes (GSD) | 2 | ✓ | NA | ✓ | ✓ | NA | HEDIS 2024 | P4P | |
| HIV Viral Load Suppression (VLS) | 1 | ✓ | NA | NA | ✓ | NA | NYS 2024 | P4P | |
| Immunizations for Adolescents - Combination 2 (IMA, IMA-E) | 2 | ✓ | NA | NA | NA | ✓ | HEDIS 2024 | P4P | |
| Initiation and Engagement of Substance Use Disorder Treatment (IET) | ✓ | ✓ | NA | ✓ | NA | HEDIS 2024 | P4P | ||
| Initiation of Pharmacotherapy upon New Episode of Opioid Dependence (POD-N) | ✓ | NA | ✓ | ✓ | NA | NYS 2024 | P4P | ||
| Kidney Health Evaluation for Patients With Diabetes (KED) | ✓ | NA | ✓ | ✓ | NA | HEDIS 2024 | P4P | ||
| Oral Evaluation, Dental Services (OED) | ✓ | NA | NA | NA | ✓ | HEDIS 2024 | P4R | ||
| Pharmacotherapy for Opioid Use Disorder (POD) | 3 | ✓ | NA | ✓ | NA | NA | HEDIS 2024 | P4P | |
| Potentially Preventable Mental Health Related Readmission Rate 30 Days (PPR-MH) | 1 | ✓ | NA | ✓ | NA | NA | NYS 2024 | P4P | |
| Prenatal and Postpartum Care (PPC) | 2 | ✓ | ✓ | NA | NA | NA | HEDIS 2024 | P4P | |
| Prenatal Immunization Status (PRS-E) | 3 | ✓ | ✓ | NA | NA | NA | HEDIS 2024 | P4P | |
| Social Need Screening and Intervention (SNS-E) | 3 | ✓ | ✓ | ✓ | ✓ | ✓ | HEDIS 2024 | P4P | |
| Topical Fluoride for Children (TFC) | ✓ | NA | NA | NA | ✓ | HEDIS 2024 | P4R | ||
| Well-Child Visits in the First 30 Months of Life (W30) | ✓ | NA | NA | NA | ✓ | HEDIS 2024 | P4P | ||
| Maternity | |||||||||
| Cesarean Birth (eCQM) (PC-02) | NA | NR | NA | NA | NA | The Joint Commission (TJC) | P4R | ||
| Contraceptive Care - Postpartum | NA | NR | NA | NA | NA | US Office of Population Aff airs | P4R | ||
| Depression Screening and Follow-Up for Adolescents and Adults (DSF-E) | 3 | NA | ✓ | NA | NR | NR | HEDIS 2024 | P4R | |
| Exclusively Breast Milk Feeding (PC-05) | NA | NR | NA | NA | NA | TJC 2020 | P4R | ||
| Incidence of Episiotomy | NA | NR | NA | NA | NA | AMA-PCPI* | P4R | ||
| Live Births Weighing Less Than 2,500 Grams (LBW-CH) | 1 | NA | ✓ | NA | NA | NA | Centers for Disease Control & Prevention (CDC) | P4R | |
| Postpartum Depression Screening and Follow-up (PDS-E) | 3 | NA | ✓ | NA | NA | NA | HEDIS 2024 | P4R | |
| Prenatal Depression Screening and Follow-up (PND-E) | 3 | NA | ✓ | NA | NA | NA | HEDIS 2024 | P4R | |
| Preventive Care and Screening: Tobacco Use: Screening and Cessation Intervention | NA | NR | NR | NR | NA | NCQA 2024 | P4R | ||
| HARP | |||||||||
| Continuing Engagement in Treatment Alcohol and Other Drug Dependence (CET) | NA | NA | ✓ | NA | NA | NYS 2024 | P4R | ||
| Preventive Care and Screening: Body Mass Index (BMI) Screening and Follow-Up Plan | NA | NA | NR | NR | NA | CMS 2024 | P4R | ||
| Statin Therapy for Patients with Cardiovascular Disease (SPC) | NA | NA | ✓ | ✓ | NA | HEDIS 2024 | P4R | ||
| Use of Pharmacotherapy for Alcohol Abuse or Dependence (POA) | 3 | NA | NA | ✓ | ✓ | NA | NYS 2024 | P4R | |
| HIV/AIDS | |||||||||
| Sexually Transmitted Infections: Screening for Chlamydia, Gonorrhea, and Syphilis | 1 | NA | NA | NA | NR | NA | NYS 2024 | P4R | |
| Children | |||||||||
| Follow-Up Care for Children Prescribed ADHD Medication (ADD-E) | NA | NA | NA | NA | ✓ | HEDIS 2024 | P4R | ||
| Use of First-Line Psychosocial Care for Children and Adolescents on Antipsychotics (APP) | 3 | NA | NA | NA | NA | ✓ | HEDIS 2024 | P4R | |
| Weight Assessment and Counseling for Nutrition and Physical Activity for Children/Adolescents (WCC) | 2 | NA | NA | NA | NA | ✓ | HEDIS 2024 | P4R | |
* AMA-PCPI - American Medical Association - Physician Consortium for Performance Improvement
✓ - Required to Report NA - Not Applicable to the Arrangement NR - (Purple Shading) - Not required to be reported
1. There are no reporting requirements for this measure. NYS will calculate the measure result for MY2024
2. For measures that you may have reported using hybrid sample in the PLD for QARR, we request that you report the administrative/ECDS denominator and numerator for VBP per measure specifications.
3. This measure is being reported via your QARR data, you do not need to report it on the PCMH file.
IV. File Specifications - Mainstream VBP
NYS PCMH SCORECARD PATIENT-LEVEL DETAIL FILE
Please use your 2024 QARR/HEDIS data warehouse as the source for this information. Do not recalculate or update measure results. However, in addition to the measure elements that you reported for QARR/HEDIS for 2024, please include the provider/practice information that was attributed to the member using your plan's attribution methodology. Please continue to report the provider and practice site of the service as outlined in layout request, specifically two separate fields for TIN: Practice TIN and Contractor TIN. The NYS Patient-Centered Medical Home (NYS PCMH) file is modeled after the NYS 2024 Patient-Level Detail file (PLD) that you prepared as part of your QARR submission, and many of the data elements in the NYS PCMH file follow the same definitions and format as used to define the data elements in the PLD. You may find it helpful to use the PLD as a resource or starting point in completing the NYS PCMH file. We ask that you populate the NYS PCMH with all Lines of Business that you serve (e.g., Medicaid). Once completed, please upload the file to IPRO SEND site. A subfolder in the "QARR" folder where you will upload your 2024 QARR files entitled "NYS PCMH 2024" will be created for your submission. If someone other than your QARR liaison will be responsible for NYS PCMH reporting, please contact the VBP Team at OHSQAVBP@health.ny.gov for access to the FTP site. Please note that the deadline for submission is Friday, July 25, 2025.
Exceptions to the PLD file are noted below:
- The NYS PCMH file requests Medicare HEDIS data, which is not required for QARR reporting.
- The Plan ID is not your plan's QARR ID. The Plan ID field should be populated with the Organization ID that you used to submit the IDSS to NCQA.
- Note that the Organization ID is different from the Submission ID. Submission ID which is specific to a Line of Business.
- The Organization ID provides six digits. If your plan's ID is smaller, please right justify.
- For Medicaid, HARP, and HIV/SNP we are asking that you populate the member's CIN in the ID field and not an internal ID number. For EP use the NYHX ID, and for all other products, please use an internally-defined ID number. In order to receive credit for VBP reporting, the Medicaid CIN must be populated for Medicaid, HARP, and HIV/SNP members.
- Provider/Practice attribution information is required for NYS PCMH. This information is not required for QARR reporting.
SUMMARY OF CHANGES NYS PCMH FILE:
- Hemoglobin A1c Control for Patients with Diabetes (HBD); name and specifications REVISED by NCQA, now: Glycemic Status Assessment for Patients with Diabetes (GSD).
- Follow-Up Care for Children Prescribed ADHD Medication (ADD) non-ECDS version RETIRED by NCQA, ADD-E version will be collected.
- Ambulatory Care (AMB) RETIRED by NCQA.
- Colorectal Cancer Screening (COL) non-ECDS version RETIRED by NCQA, COL-E version will be collected.
- Inpatient Utilization–General Hospital/Acute Care (IPU) RETIRED by NCQA.
- Use of Spirometry Testing in the Assessment and Diagnosis of COPD (SPR) RETIRED by NCQA.
SPECIFIC INSTRUCTIONS FOR NYS PCMH FILE
- PLEASE carefully review the reporting requirements and layout of the NYS MY2024 Patient Level Detail File Specifications and the NYS 2024 Patient-Centered Medical Home (PCMH). Numerous updates to streamline and consolidate reporting requirements have been made to the files.
- Please be aware that although the member ID for all products except Medicaid is an internal number assigned by your plan, you will need to link the member to the provider of service. You should use a naming convention that will facilitate this process.
- If a member is reported for a specific measure in more than one product line (e.g., duals), please report all member details for all applicable product lines.
- A Member ID (Field #3) may be included on the file more than once if the member is in more than one product line during the reporting period.
- For hybrid measures that you reported to NCQA/NYS using the hybrid methodology, which requires calculating the measure based on a sample rather than the entire eligible population, for NYS PCMH only, we are requesting that you report the administrative denominator and administrative numerator (and not the hybrid data), which is populated on the IDSS.
- Members in the file must be in at least one measure.
- Measures that are not applicable to the member should be zero-filled.
- A valid Practice Tax ID (TIN)(Field #6) is nine characters. If the TIN is not available, set the field value to "999999999".
- Practice Name must be populated in the Practice Name Field (Field #9) only.
- Practice Address Line 1 (Field #10) must contain the street address of the Practice, not the Practice Name.
- For Fields #7-22, leave these fields blank if the member cannot be attributed to any provider or you are not able to identify the provider. Member-level details should not be removed from the file submission, even if a provider is not attributed.
- For Field #21, populate with valid TINs only. If a member is NOT attributed to a VBP Contractor set to '999999999'.
- Retired measures were removed from the PCMH 2024 File Layout.
- Follow-Up Care for Children Prescribed ADHD Medication ECDS-version (ADD-E) was added. The denominators (Fields #25, 27) and numerators (Fields #26, 28) have been updated for MY2024.
- Hemoglobin A1c Control (HBD) was revised to Glycemic Status Assessment for Patients with Diabetes (GSD). The denominator (Field #80), numerator for Glycemic Status <8.0% (Field #81), and Glycemic Status >9.0% (Field #82) have been updated for MY2024.
- Only MCOs reporting their Medicaid Line of Business need report the following 8 VBP specific measures:
- Statin Therapy for Patients with Cardiovascular Disease (SPC),
- Diabetes Screening for Schizophrenia or Bipolar Disorder Who Are Using Antipsychotic Medications (SSD),
- Initiation of Pharmacotherapy upon New Episode of Opioid Dependence (POD-N),
- Weight Assessment and Counseling for Nutrition and Physical Activity for Children/Adolescents (WCC; Administrative rate),
- Follow-Up Care for Children Prescribed ADHD Medication (ADD-E),
- Prenatal and Postpartum Care (PPC; Administrative rate),
- Depression Remission or Response for Adolescents and Adults (DRR-E) and
- Well-Child Visits in the First 30 Months of Life (W30).
For questions regarding this request, please contact the VBP Team in the Office of Health Services Quality and Analytics at: OHSQAVBP@health.ny.gov.
PATIENT ATTRIBUTION FILE
The Department is asking insurers to provide an attribution file for all members enrolled in a VBP arrangement during the 2024 Calendar Year per the methodology specified in your Department-approved contract. The attribution file will be used in combination with other quality measure sources (e.g., 2024 NYS Patient-Level Detail File) to aggregate quality results for the 2024 Category 1 population-specific measures by VBP Contractor.
NOTE: MLTC attribution instructions are different than for other populations. Please follow the instructions in the MLTC attribution file subsection of this manual.
FILE FORMAT:
Submit a comma-separated values (CSV) file with the following specifications:
- The file must not have additional columns beyond those shown in the following table. (Refer to companion excel file.)
- Data must include column names. The first row in the file must be the column names as documented in the following table.
- Please be advised that significant changes have been made to the data elements for MY2024 VBP Attribution file, as outlined in the table below. Please carefully review the updated element table and ensure the data is populated accordingly.
- All fields are mandatory. Do not leave any fields blank.
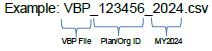
Naming Convention:
VBP_PlanID_2024.cvs (Refer to field 1 in the table below.)
All files are due no later than Friday, July 25, 2025.
| Element # | Name | Direction | Allowed Values | Data Type | Length | Start | End |
|---|---|---|---|---|---|---|---|
| 1 | Plan_ID# | Organization ID is used to submit the IDSS to NCQA. This ID is consistent across all Lines of Business. | ###### | VARCHAR | 6 | 1 | 6 |
| 2 | Product_Line | A member's product line at the end of the measurement period. | 01 = MEDICAID 02 = SNP 11 = HARP |
NUMBER | 2 | 7 | 8 |
| 3 | Unique_Member_ID# | Medicaid Client ID Number (CIN) *The field is alphanumeric and should be treated as a text field. |
VARCHAR | 8 | 9 | 16 | |
| 4 | Practice_Tax_ID# | Populate with valid TINs only. | ######### | NUMBER | 9 | 17 | 25 |
| 5 | Provider_NPI | National Provider Identifier - 10 Digit ID | ########## | NUMBER | 10 | 26 | 35 |
| 6 | VBP_Contractor_Tax_ID# | Populate withvalid TINs only. Please include the TIN of the VBP Contractor. If the member is NOT in a VBP level 1 or higher arrangement set to '999999999'. | ######### | NUMBER | 9 | 36 | 44 |
| 7 | VBP_Contractor_DBA_Name | Enter the DBA name listed on your VBP contract/arrangement. | VARCHAR | 50 | 45 | 94 | |
| 8 | VBP_Contractor_Type | 1 = Provider/ Hospital 2 = IPA 3 = ACO 9 = Unknown |
NUMBER | 1 | 95 | 95 | |
| 9 | VBP_Arrangement_Type | Refer to Section C, #2b of the DOH 4255 -Provider Contract Statement and Certification form. | 1 = TCGP 3 = HARP 4 = HIV/AIDs 5 = Maternity 6 = Children's 7 = Off Menu |
NUMBER | 1 | 96 | 96 |
| 10 | DOH_VBP_Contract_ID# | The number provided by the Department in the Agreement approval letter begins with DOH ID #### | #### | NUMBER | 4 | 97 | 100 |
| 11 | MCO_Unique_Contract_ID# | Plan generated ID used to submit contract to DOH; Section A, #3 of the 4255. | VARCHAR | 50 | 101 | 150 | |
| 12 | Prov_Att_start_date | MMDDYYYY - Must be between 1/1/2024 and 12/31/2024 | MMDDYYYY | DATE | 8 | 151 | 158 |
| 13 | Prov_Att_end_date | MMDDYYYY - Must be between 1/1/2024 and 12/31/2024 | MMDDYYYY | DATE | 8 | 159 | 166 |
| Field # | Field Name | Description/Specifications |
|---|---|---|
| 1 | Plan_ID# | Enter your Organization ID used to submit the IDSS to NCQA. This ID is consistent across all Lines of Business. |
| 2 | Product_Line | Enter the member's product line at the end of the measurement period. Enter the corresponding number (01) Medicaid, (02) SNP, (11) HARP. |
| 3 | Unique_Member_ID# | Enter member's Medicaid Client Identification Number (CIN). The field should be continuous without any spaces or hyphens. The field is alpha-numeric and should be treated as a text field. |
| 4 | Practice_Tax_ID# | Enter the 9-digit Federally assigned Tax Identification Number for the Practice of the member's provider. Populate with valid TINs only. This field is mandatory - do not leave it blank! |
| 5 | Provider_NPI | This is the unique 10-digit National Provider Identifier (NPI) of the provider the member was serviced by during the reporting period. This should be a provider organization that had frequent contact with the member and, therefore, could potentially affect the need for hospitalization or not. A member may be serviced by multiple providers during the same time period (provide one row of data for every provider a member was serviced by). |
| 6 | VBP_Contractor_Tax_ID# | This is the unique 9-digit tax identification number of the VBP Contractor (not the provider) that the member is assigned to a Level 1 or higher VBP arrangement during the reporting period. If not applicable, fill with 999999999. |
| 7 | VBP_Contractor_DBA_Name | The "Doing Business As" (DBA) name is the operating name of a company, as opposed to the legal name of the company. The VBP Contractor may be an ACO, IPA, individual provider, or hospital. |
| 8 | VBP_Contractor_Type | In this field, enter '1' if the contractor is a provider (provider includes hospitals), '2' if the contractor is an IPA, '3' if the contractor is an ACO, '9' if Unknown |
| 9 | VBP_Arrangement_Type | In this field, enter "1" if the VBP arrangement type is a TCGP arrangement, "3" if it is a HARP arrangement, "4" if it is an HIV/AIDs arrangement, "5" if it is a Maternity arrangement, "6" if it is a Children's arrangement, "7" if it is an Off-Menu arrangement. This information can be found in Section C, #2b of the DOH 4255 - Provider Contract Statement and Certification form. |
| 10 | DOH_VBP_Contract_ID# | This is the number provided by the Department in the Agreement approval letter for your VBP arrangement, it begins with DOH ID ####. If you need assistance obtaining the correct DOH VBP Contract Identifier, please email NYS Department of Health VBP mailbox at OHSQAVBP@health.ny.gov |
| 11 | MCO_Unique_Contract_ID# | This is the contract identifier created by your plan, which is a required component of all contracts submitted for review (it can be found in Section A, #3 of the DOH 4255, it is also typically in the footer of your contract documents. If you need assistance obtaining your correct MCO Unique Contract Identifier, please email the VBP mailbox at OHSQAVBP@health.ny.gov |
| 12 | Prov_Att_start_date | This is the attribution start date with the provider when the member was first attributed to the provider. This date must be during the reporting period. It should be in the format of MMDDYYYY with no intervening "-"or "/". The format is the same if data is submitted via a fixed-width file or CSV. |
| 13 | Prov_Att_end_date | This is the attribution end date with the provider when the member was last attributed to the provider. This date must be during the reporting period. It should be in the format of MMDDYYYY with no intervening "-"or "/". The format is the same if data is submitted via a fixed-width file or CSV. |
SUBMISSION EXAMPLES AND DATA REQUIREMENTS CHECKLIST
Please refer to section VII Appendix, Table 6 at the end of this manual or the VBP Attribution Layout Data Dictionary on the Value Based Payment (VBP) website under the VBP Quality Measures tab in the VBP Reporting Requirements Technical Specifications manual section for a layout examples and further instruction on the CSV submission requirements.
FILE SUBMISSION:
Files for all arrangement types are to be submitted to the New York State Department of Health via the Secure File Transfer 2.0 of the Health Commerce System (HCS). Files should be submitted to OHSQA4 VBP Evaluation or OHSQAVBP@health.ny.gov via HCS.
Files must be received electronically by 11:59 p.m. ET; Friday, July 25, 2025.|top of section| |table of contents|
REPORTING GUIDELINES VBP MLTC
INTRODUCTION
The Department is requesting insurers to submit a Patient Attribution file, which will be used to create aggregated quality results by Provider or VBP Contractor. The Department will calculate all reportable Category 1 quality measure results for the arrangements. The attribution methodology and Patient Attribution file layout are included in Section VI of this document.
- Table 2: 2025 MLTC VBP List of Required Measures
- Lists the 2025 MLTC VBP Category 1 measure set and indicates the 2024 measures required for reporting.
MEASURE CHANGES
Changes to the Reporting Requirements for 2025 Measure Sets were made based on the feedback received by the Department from the Clinical Advisory Groups, Measure Support Task Force and Sub-teams, and from other stakeholder groups. In instances where a measure was moved from Category 1 in MY2024 to Category 2 in MY2025 or removed entirely, the Department will not require reporting of the data related to those measures. Those changes are indicated in the publicly posted MLTC VBP Measure Sets.
Table 2: 2024 MLTC VBP List of Required Measures
| Measures | Notes | Arrangement Type | Specifications | Class | |
|---|---|---|---|---|---|
| MLTC | |||||
| Managed Long-Term Care (MLTC) | |||||
| Percentage of members who did not have an emergency room visit in the last 90 days | 1 | ✓ | NYS 2025 | P4P | |
| Percentage of members who did not experience falls that resulted in major or minor injury in the last 90 days | 1 | ✓ | NYS 2025 | P4P | |
| Percentage of members who received an influenza vaccination in the last year | 1 | ✓ | NYS 2025 | P4P | |
| Percentage of members who did not experience uncontrolled pain | 1 | ✓ | NYS 2025 | P4P | |
| Percentage of members who were not lonely or were not distressed | 1 | ✓ | NYS 2025 | P4P | |
| Percentage of members who remained stable or demonstrated improvement in pain intensity | 1 | ✓ | NYS 2025 | P4P | |
| Percentage of members who remained stable or demonstrated improvement in Nursing Facility Level of Care (NFLOC) score | 1 | ✓ | NYS 2025 | P4P | |
| Percentage of members who remained stable or demonstrated improvement in urinary continence | 1 | ✓ | NYS 2025 | P4P | |
| Percentage of members who remained stable or demonstrated improvement in shortness of breath | 1 | ✓ | NYS 2025 | P4P | |
| Potentially Avoidable Hospitalizations (PAH) for a primary diagnosis of heart failure, respiratory infection, electrolyte imbalance, sepsis, anemia, or urinary tract infection | 1, 2 |
✓ | NYS 2025 | P4P | |
✓ - Required to Report NA - Not Applicable to the Arrangement Shading - Purple - Not required to be reported
1 - There are no reporting requirements for this measure. NYS will calculate the measure result for MY2024/2024
2 - NYS will calculate this measure for the community-based providers.
VI. File Specifications - VBP MLTC
MLTC ATTRIBUTION FILE
Starting with MY 2022, quality measures will only be calculated on an annual basis (e.g., MY2024 will reflect measurement period of January 1st - December 31st, 2024). Results will be distributed in Q3 of the following year (October 2025 for MY2024 results).
ATTRIBUTION METHODOLOGY:
MAP/PACE: Plan enrollees who have four or more months of continuous enrollment from April 2024 through June 2025 should be submitted in this attribution file. This attribution should be to provider organizations of CHHA, LHCSA, and, VBP contractor (if applicable) which had the most frequent contact with the member and, therefore, could potentially affect quality measures. Services being received by the member through Consumer Directed Personal Assistance (CDPAS) should not be included in this attribution file.
Changes to the NYS Long-Term Care VBP Initiative for 2021 and forward: MLTC Partial plans have been phased out of VBP as a result of the enacted SFY 2020-21 Budget. Plans are encouraged to continue to submit VBP arrangements for MAP and PACE consistent with standards outlined in the VBP Roadmap and the Provider Contract Guidelines for Article 44 MCOs, IPAs, and ACOs. Please note, MLTC Partial plans will no longer submit VBP attribution data beginning in 2024. As a result, Partial plans will not receive any attributed provider results or be included in the statewide denominator of any Category 1 P4P measures calculated by the Department.
FILE FORMAT:
- Include only members who had four or more months continuous enrollment in an MLTC MAP or PACE plan from April 2024 through June 2025.
- For each member from step 1, list all provider organization(s) that provided at least one service per month, for four or more continuous months from April 2024 through June 2025. The data should be formatted in a long form containing one row of data for each member/provider combination. Please provide at least one row of data for every provider a member was serviced by (see Examples 1 and 2 below). If a member does not have any providers from which they received four or more continuous months of care, THE MEMBER SHOULD NOT BE LISTED.
- The text file must be either: 1) fixed width and named PROVIDERS_MLTC.TXT, or 2) comma-separated values (CSV) and named PROVIDERS_MLTC.CSV.
- Fixed-width files
- Must have column start/end locations as documented in the following table.
- Data must not include column names. The first row in the file must be data.
- CSV files
- Must not have additional columns beyond those shown in the following table.
- Data must include column names. The first row in the file must be the column names as documented in the following table.
- Fixed-width files
- The following table provides instructions on the submission of member-level data.
# Field Name Data Type Length Start Colum End Column Details/Comments 1 CIN Varchar 8 1 8 A Participant's Medicaid client identification number. The field should be continuous without any spaces or hyphens. The field is alpha-numeric and should be treated as a text field. This field may not be NULL. 2 MMIS_ID Varchar 8 9 16 The MLTC Plan's numeric eight-digit ID. This field may not be NULL. 3 Prov_NPI Varchar 10 17 26 The unique 10-digit National Provider Identifier (NPI) for the provider the member was serviced by during the reporting period. 4 Prov_start_date Date 8 27 34 MMDDYYYY - Must be between April 2024 - June 2025 5 Prov_end_date Date 8 35 42 MMDDYYYY - Must be between April 2024 - June 2025 6 Contractor_TIN Varchar 9 43 51 The unique 9-digit tax identification number of the VBP Contractor. Only submit the TIN, if this member is included in a level 2 or higher arrangement with a VBP Contractor. If not applicable or level 1 arrangement, fill with 999999999. 7 Contractor_Type Varchar 1 52 52 1= CHHA, LHCSA, 2= IPA, 3= Hospital, 4= ACO, 8= Other, and 9 = NA. Only submit if this member is included in a level 2 or higher arrangement with a VBP Contractor. If not applicable or level 1 arrangement, fill 9 = NA. 8* DOH_VBP_Contract_# Number 4 53 56 The number provided by the Department in the Agreement approval letter begins with DOH ID ###. *You must populate either field 8 or 9, preferably both fields should be populated. 9* MCO_Unique_Contract_ID# Varchar 50 57 107 Plan generated ID used to submit contract to DOH; Section A, #3 of the 4255. *You must populate either field 8 or 9, preferably both fields should be populated.
FIELD DEFINITIONS:
Prov_NPI: This is the unique 10-digit National Provider Identifier (NPI) of the provider the member was serviced by during the reporting period. This should be a provider organization that had frequent contact with the member and, therefore, could potentially affect the need for hospitalization or not. A member may be serviced by multiple providers during the same time period (provide one row of data for every provider a member was serviced by).
Prov_start_date: This is the service start date with the provider. This date must be during the reporting period. It should be in the format of MMDDYYYY with no intervening "-" or "/". The format is the same if data is submitted via a fixed-width file or CSV.
Prov_end_date: This is the service end date with the provider. This date must be during the reporting period. It should be in the format of MMDDYYYY with no intervening "-" or "/". The format is the same if data is submitted via a fixed-width file or CSV.
Contractor TIN: This is the unique 9-digit tax identification number of the VBP Contractor (not the provider) that the member is assigned to for a Level 2 arrangement during the reporting period. A member can only be assigned to one level 2 or higher VBP contractor at a time. If not applicable or level 1, fill with 999999999.
Contractor_Type: The VBP Contractor may be an ACO, IPA, hospital, or large LHCSA/CHHA that is coordinating services for many LHCSAs or CHHAs. This field is for the VBP Contractor (not the provider) that the member is assigned to a level 2 or higher arrangement during the reporting period. A member can only be assigned to one level 2 or higher VBP contractor at a time. If not applicable or level 1 arrangement, fill with 9.
* DOH_VBP_Contract_#: This is the number provided by the Department in the Agreement approval letter for your VBP arrangement, it begins with DOH ID ####.
* MCO_Unique_Contract_ID#: This is the contract identifier created by your plan, which is a required component of all contracts submitted for review (it can be found in Section A, #3 of the DOH 4255, it is also typically in the footer of your contract documents.
*You must populate either field 8 or 9, preferably both fields should be populated.
DATA REQUIREMENTS CHECKLIST
Please refer to section VII Appendix, Table 8 at the end of this manual, for attribution file checklists for the MLTC attribution file. The checklist is designed to ensure fields in the attribution file are standardized appropriately and are not required to be submitted with the attribution files.
FILE SUBMISSION:
Files are to be submitted to the New York State Department of Health via the Secure File Transfer 2.0 of the Health Commerce System. Files should be submitted to MLTC VBP Evaluation mailbox. Files are to be submitted by close of business on Friday, July 25, 2025.
NOTE: When a Provider/NPI has overlapping service dates for a member, the service dates should be collapsed into one record with the earliest start date and furthest end date. Multiple rows for the same member/provider may be provided only if the provider/NPI has nonoverlapping service dates and each time frame meets the four months of service criterion. (see Example 3 below).
Submission Examples:
Example 1 and 2 below illustrate two different providers, with overlapping service dates, adding a single member from February through June 2024.
Example 1 not covered by level 2 or higher VBP contract:
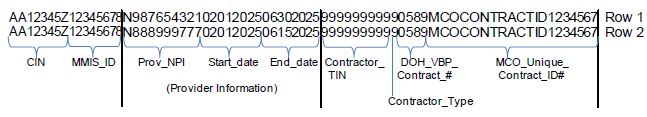
Example 2 covered by level 2 or higher VBP contract:
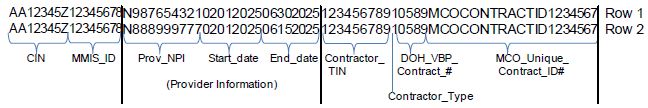
Example 3 below illustrates a member who was continuously enrolled for four or more months in the health plan and received at least one service per month from the same provider organization for four or more continuous months, for two separate non-overlapping time periods and is covered by level 2 or higher VBP contract during April 2024 through June 2024.
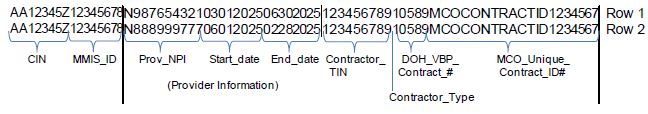
Fully Capitated Plans:
Because the HEDIS and CMS-based P4R category 1 measures cannot be calculated by the Department, plans must calculate and report Plan/Provider-VBP Contractor performance to the Department by July 25, 2025. Files are to be submitted to the New York State Department of Health via the Secure File Transfer 2.0 of the Health Commerce System. Files should be submitted to the MLTC VBP Evaluation mailbox.
Plans should submit an Excel file with the following format. Submit a row for each measure being reported. Plans are required to report on all measures for each plan-provider combination.
| # | Field Name * | Data Type | Excel Column Placement | Details/Comments |
|---|---|---|---|---|
| 1 | MMIS_ID | Varchar | Column A | The MLTC Plan's numeric eight-digit ID. This field may not be NULL. |
| 2* | Prov_NPI | Varchar | Column B | The unique 10-digit National Provider Identifier (NPI) for the provider the member was serviced by during the reporting period. This field may not be NULL. |
| 3 | Measure ID | Varchar | Column C | Use the measure ID from the table below |
| 4 | Denominator for Measure | Varchar | Column D | Report the total number of members included in the denominator for the given measure |
| 5 | Numerator for Measure | Varchar | Column E | Report the total number of members that were included in the numerator for the given measure |
| 6 | Exclusions for Measure | Varchar | Column F | Report the number of members excluded from the given measure |
| 7 | Rate for Measure | Varchar | Column G | Report the rate to the hundredth decimal place |
| 8* | Contractor_TIN | Varchar | Column H | The unique 9-digit tax identification number of the VBP Contractor. Only submit the TIN, if this member is included in a level 2 or higher arrangement with a VBP Contractor. If not applicable or level 1 arrangement, fill with 999999999. |
| 9* | Contractor_Type | Varchar | Column I | 1= CHHA, LHCSA, 2= IPA, 3= Hospital, 4= ACO, 8= Other, and 9= NA. Only submit if this member is included in a level 2 or higher arrangement with a VBP Contractor. If not applicable or level 1 arrangement, fill 9 = NA. |
| 10 * | DOH_VBP_Contract_# | Varchar | Column J | The number provided by the Department in the Agreement approval letter begins with the Department ID ####. *You must populate either field 10 or 11, preferably both. |
| 11 * | MCO_Unique_Contract_ID# | Varchar | Column K | Plan generated ID used to submit the contract to DOH; Section A, #3 of the 4255. *You must populate either field 10 or 11, preferably both. |
| * See Field Definitions under preceding MLTC Attribution File specifications | ||||
| Measure Name | Measure ID |
|---|---|
| MAP P4R measures (Measure Source/ Steward: NCQA/ HEDIS) | |
| Antidepressant Medication Management - Effective Acute Phase Treatment (AMM)* | 1 |
| Antidepressant Medication Management - Effective Continuation Phase Treatment (AMM)* | 2 |
| Colorectal Cancer Screening (COL-E)* | 3 |
| Eye Exam for Patients with Diabetes (EED)* | 4 |
| Kidney Health Evaluation for Patients with Diabetes (KED)* | 5 |
| Follow-up After Hospitalization for Mental Illness - 7 Days (FUH)^ | 6 |
| Follow-up After Hospitalization for Mental Illness - 30 Days (FUH)^ | 7 |
| Initiation of Substance Use Disorder Treatment (IET)* | 8 |
| PACE P4R measures (Measure Source/ Steward: CMS) | |
| PACE Participant Emergency Department Utilization Without Hospitalization | 9 |
| Percentage of Participants Not in Nursing Homes | 10 |
| Percentage of Participants with an Annual Review of Their Advance Directive or Surrogate Decision-Maker AND Percentage of Participants with an Annual Review of Their Advance Directive or Surrogate Decision-Maker | 11 |
| * Included in the TCGP measure set ^ Included in the Health and Recovery Plan (HARP) measure set |
|
VII. APPENDIX
TABLE 3: 2024 MAINSTREAM VBP LIST OF CATEGORY 2 MEASURES
| Measures | Notes | Arrangement Type | Measure Steward | |||||
|---|---|---|---|---|---|---|---|---|
| TCGP | Maternity | HARP | HIV/AIDS | Children | ||||
| Maternity | ||||||||
| Hepatitis B Vaccine Coverage Among All Live Newborn Infants Prior to Hospital or Birthing Facility Discharge | NA | CAT 2 | NA | NA | NA | Centers for Disease Control and Prevention |
||
| Postpartum Blood Pressure Monitoring | NA | CAT 2 | NA | NA | NA | Texas Maternity Bundle |
||
| HARP/Behavior Health | ||||||||
| Asthma Action Plan | NA | NA | CAT 2 | CAT 2 | NA | American Academy of Allergy, Asthma & Immunology: (AAAAI) |
||
| Asthma: Assessment of Asthma Control - Ambulatory Care Setting | NA | NA | CAT 2 | CAT 2 | NA | AAAAI | ||
| Mental Health Engagement in Care - 30 Days | NA | NA | CAT 2 | NA | NA | NYS 2024 | ||
| Percentage of HARP Enrolled Members Who Received Personalized Recovery Oriented Services (PROS) or Home and Community- Based Services (HCBS) | NA | NA | CAT 2 | NA | NA | NYS 2024 | ||
| Use of Pharmacotherapy for Opioid Dependence | NA | NA | CAT 2 | CAT 2 | NA | NYS 2024 | ||
| HIV/AIDS | ||||||||
| Continuity of Pharmacotherapy for Opioid Use Disorder (OUD) | NA | NA | NA | CAT 2 | NA | University of Southern California (USC) | ||
| Hepatitis C Screening | NA | NA | NA | CAT 2 | NA | HRSA | ||
| Housing Status | NA | NA | NA | CAT 2 | NA | HRSA | ||
| Prescription of HIV Antiretroviral Therapy | NA | NA | NA | CAT 2 | NA | HRSA | ||
| Substance Abuse Screening | NA | NA | NA | CAT 2 | NA | HRSA | ||
| Children | ||||||||
| Postpartum Depression Screening and Follow-up (PDS-E) | NA | NA | NA | NA | CAT 2 | NCQA | ||
TABLE 4. 2024 VBP MLTC CATEGORY 2 MEASURES
| Measures | Notes | Arrangement Type | Measure source/Steward |
|---|---|---|---|
| MLTC | |||
| Care for Older Adults - Medication Review | CAT 2 | NCQA | |
| Use of High-Risk Medications in Older Adults | CAT 2 | NCQA | |
| Percentage of members who rated the quality of home health aide or personal care aide services within the last 6 months as good or excellent | 1 | CAT 2 | MLTC Survey/New York State |
| Percentage of members who responded that they were usually or always involved in making decisions about their plan of care | 1 | CAT 2 | MLTC Survey/New York State |
| Percentage of members who reported that within the last 6 months the home health aide or personal care aide services were always or usually on time | 1 | CAT 2 | MLTC Survey/New York State |
- Included in the NYS DOH MLTC Quality Incentive measure set.
TABLE 5 - NYS FIPS CODES BY COUNTY
| County Name | FIPS Code | County Name | FIPS Code | County Name | FIPS Code |
|---|---|---|---|---|---|
| Albany | 001 | Jefferson | 045 | St. Lawrence | 089 |
| Allegany | 003 | Kings | 047 | Saratoga | 091 |
| Bronx | 005 | Lewis | 049 | Schenectady | 093 |
| Broome | 007 | Livingston | 051 | Schoharie | 095 |
| Cattaraugus | 009 | Madison | 053 | Schuyler | 097 |
| Cayuga | 011 | Monroe | 055 | Seneca | 099 |
| Chautauqua | 013 | Montgomery | 057 | Steuben | 101 |
| Chemung | 015 | Nassau | 059 | Suffolk | 103 |
| Chenango | 017 | New York | 061 | Sullivan | 105 |
| Clinton | 019 | Niagara | 063 | Tioga | 107 |
| Columbia | 021 | Oneida | 065 | Tompkins | 109 |
| Cortland | 023 | Onondaga | 067 | Ulster | 111 |
| Delaware | 025 | Ontario | 069 | Warren | 113 |
| Dutchess | 027 | Orange | 071 | Washington | 115 |
| Erie | 029 | Orleans | 073 | Wayne | 117 |
| Essex | 031 | Oswego | 075 | Westchester | 119 |
| Franklin | 033 | Otsego | 077 | Wyoming | 121 |
| Fulton | 035 | Putnam | 079 | Yates | 123 |
| Genesee | 037 | Queens | 081 | Out of State | 000 |
| Greene | 039 | Rensselaer | 083 | Unknown/Missing | 999 |
| Hamilton | 041 | Richmond | 085 | ||
| Herkimer | 043 | Rockland | 087 |
TABLE 6: MAINSTREAM VBP SUBMISSION EXAMPLES
The example below illustrates one member's data submitted as a CSV file. Additional examples and directions can be found in the VBP Attribution Layout Data Dictionary file, posted on the Value Based Payment (VBP) website under the VBP Quality Measures tab in the VBP Reporting Requirements Technical Specifications manual section.
Fields 1-8:
| Plan ID# | Product Line | Unique Member ID (CIN) | Practice Tax ID (TIN) | Provider NPI | VBP Contractor Tax ID# |
VBP Contractor DBA Name |
VBP Contractor Type |
|---|---|---|---|---|---|---|---|
| 123456 | 01 | WA12345X | 123456789 | N987654321 | 123456789 | Health Clinic NY |
1 |
Fields 9-13:
| VBP Arrangement Type |
DOH VBP Contract ID |
MCO Unique Contract ID# |
Provider Attribution Start Date |
Provider Attribution End Date |
|---|---|---|---|---|
| 1 | 2983 | ABC.HealthClinic 4.12.18 | 01012024 | 12312024 |
The example below illustrates one member attributed to two different providers, in the same VBP arrangement, within the reporting period submitted as a CSV file.
Member Data, attributed to Provider 1 from 1/1/2024 to 04/30/2024
Fields 1-8:
| Plan ID# | Product Line | Unique Member ID (CIN) | Practice Tax ID (TIN) | Provider NPI | VBP Contractor Tax ID# | VBP Contractor DBA Name | VBP Contractor Type |
|---|---|---|---|---|---|---|---|
| 123456 | 01 | WA12345X | 123456789 | N987654321 | 123456789 | Health Clinic NY | 1 |
Fields 9-13:
| VBP Arrangement Type |
DOH VBP Contract ID |
MCO Unique Contract ID# |
Provider Attribution Start Date |
Provider Attribution End Date |
|---|---|---|---|---|
| 1 | 2983 | ABC.HealthClinic 4.12.18 | 01012024 | 04302024 |
Member Data, attributed to Provider 2 from 5/1/2024 to 12/31/2024
Fields 1-8:
| Plan ID# | Product Line | Unique Member ID (CIN) | Practice Tax ID (TIN) | Provider NPI | VBP Contractor Tax ID# |
VBP Contractor DBA Name |
VBP Contractor Type |
|---|---|---|---|---|---|---|---|
| 123456 | 01 | WA12345X | 123456789 | N123456789 | 123456789 | Health Clinic NY | 1 |
Fields 9-13:
| VBP Arrangement Type |
DOH VBP Contract ID |
MCO Unique Contract ID# |
Provider Attribution Start Date |
Provider Attribution End Date |
|---|---|---|---|---|
| 1 | 2983 | ABC.HealthClinic 4.12.18 | 05012024 | 12312024 |
TABLE 7: MCO ATTRIBUTION FILE - DATA QUALITY CHECKLIST
| Data Quality Check | Value | Notes |
|---|---|---|
| Value used for Plan_ID# is the Organization ID used to submit IDSS to NCQA | ☐ Yes ☐ No |
|
| Every record includes a valid Medicaid Client Identification Number (CIN) | ☐ Yes ☐ No |
The field is alpha-numeric and must be a valid CIN. Do not use internal organization member identification numbers. |
| Total number of records submitted | ||
| Number of unique members included in file | ||
| Number of unique members by product line | MC (01) = SNP (02) = HARP (11)= |
|
| All records include a valid Practice_Tax_ID# | ☐ Yes ☐ No |
|
| All records include a valid Practice_Name | ☐ Yes ☐ No |
|
| All records include a valid VBP_Contractor_Tax_ID# (if the member is not in a VBP level 1 or higher then the value is set to '999999999') | ☐ Yes ☐ No |
|
| For members in a VBP level 1 or higher arrangement, the VBP_Contractor_Tax_ID# represents the higher umbrella Tax ID # of the Contractor organization | ☐ Yes ☐ No |
|
| All records include a valid VBP_Contractor_DBA_Name (if the member is not in a VBP level 1 or higher than the value is set to '999999999') | ☐ Yes ☐ No |
|
| Number of members assigned to each VBP_Contractor_Type | Provider/Hospital (1) = IPA (2) = ACO (3) = Unknown (9)= |
|
| Number of members in each VBP_Arrangement_Type | TCGP (1) = HARP (3) = HIV/AIDs (4) = Maternity (5) = Children's (6) = Off Menu (7) = |
|
| Every record includes either a valid DOH_VBP_Contract_ID# OR a valid MCO_Unique_Contract_ID# | ☐ Yes ☐ No |
You must populate either the DOH_VBP_Contract_ID# field or the MCO_Unique_Contract_ID# field. Preferably, both fields should be populated. If you need assistance obtaining your correct DOH VBP Contract Identifier, please email the VBP mailbox at: OHSQAVBP@health.ny.gov |
TABLE 8: MLTC ATTRIBUTION FILE - DATA QUALITY CHECKLIST
| Data Quality Check | Value | Notes |
|---|---|---|
| Value used for MMIS_ID is the MLTC Plan's numeric eight-digit ID. | ☐ Yes ☐ No |
|
| Every record includes a valid Medicaid Client Identification Number (CIN) | ☐ Yes ☐ No |
The field is alpha-numeric and must be a valid CIN. Do not use internal organization member identification numbers. |
| Total number of records submitted | ||
| Number of unique members included in file | ||
| All records include a valid Prov_NPI number | ☐ Yes ☐ No |
The Prov_NPI is the unique 10-digit National Provider Identifier (NPI) for the provider the member was serviced by during the reporting period. |
| All records include a valid VBP_Contractor_Tax_ID# (if member is not in a VBP level 1 or higher, set the value to '999999999') | ☐ Yes ☐ No |
|
| All records include a valid VBP_Contractor_DBA_Name (if member is not in a VBP level 1 or higher then the value is set to '999999999') | ☐ Yes ☐ No |
|
| Number of members assigned to each VBP_Contractor_Type | CHHA, LHCSA (1) = IPA (2) = Hospital (3) = ACO (4) = Other (8) = NA (9) = |
|
| Every record includes either a valid DOH_VBP_Contract_# OR a valid MCO_Unique_Contract_ID# | ☐ Yes ☐ No |
You must populate either the DOH_VBP_Contract_ID# field or the MCO_Unique_Contract_ID# field. Preferably both fields should be populated. If you need assistance obtaining your correct DOH VBP Contract Identifier, please email the NYS DOH VBP mailbox at: OHSQAVBP@health.ny.gov |
| All members are assigned to only one Level 2 (or higher) VBP Contractor at a time | ☐ Yes ☐ No |
_________________________________
1. HEDIS® is a registered trademark of the National Committee for Quality Assurance (NCQA).1
|table of contents|
Follow Us